Did you know that losing weight with hypothyroidism doesn’t have to be impossible?
As a specialist in helping patients with Hypothyroidism and Hashimoto’s, I’ve been able to personally help hundreds of patients lose weight. And today I want to share with you how I do it.
I’m going to teach you how to lose weight with hypothyroidism by giving you the recommendations that I give to my patients.
I will also go over case studies of real-life patients that I’ve been able to help and provide you with what tests you need to get from your doctor to get to the root cause of your weight loss resistance.
So let’s jump in…
Why Weight Loss is so Difficult with Hypothyroidism
Does this scenario sound familiar…
You’ve been restricting your calories to try and lose weight but every time you do you get more fatigued than normal. You’ve been able to lose 5-10 pounds by doing this but once you start eating normally again your weight pops RIGHT back up to where it was.
This is something that I’ve seen over and over again and it’s something that we need to discuss.
Calorie-restricted diets are not the best way to lose weight and they can actually be harmful to those with hypothyroidism.
And this really shouldn’t come as a surprise.
After all, how many times have you tried these types of diets? How many times have they worked for you? And, did they actually help you lose weight and keep it off?
You know that they don’t work, even without looking at the numbers, but in case you were wondering, you have about a 1 in 200 chance of losing weight and keeping it off by using this type of diet.

But why is this? Why is it so hard to lose weight? Why do some people say it’s impossible?
Much of this may have to do with the way that we look at weight loss, what causes weight gain and how we approach treatment.
For instance:
We know that restricting calories results in changes to your thyroid function which may result in a reduction in your metabolic rate (1).
This effect is mediated through the changes that your body goes through during starvation and how those changes impact your hypothalamus and TRH (parts of the thyroid axis).
If you’re trying to lose weight, do you really want to lower your metabolism in the process?
Of course not, but it appears that thyroid function may be a casualty in the dieting process.
By limiting your calories you’re actually telling your body that you don’t have enough calories to survive, so your body starts to lower your metabolism to protect itself.
It lowers your metabolism by reducing the active amount of Thyroid hormone or Free T3 Levels (2).
It also does this by increasing reverse T3 levels (3)!
Oddly enough, all of these changes are also seen in a condition known as euthyroid sick syndrome which occurs when people are critically ill.
It’s certainly possible that dieting creates a metabolic process that mimics the same process that occurs when you are sick or fighting off an infection.
And the problems don’t stop there:
Most physicians, while well-meaning, tend to prescribe the ‘eat less exercise more’ mantra which may potentially make the problem worse.
So if losing weight isn’t about restricting calories, then how do you do it?
- Bottom Line: Do NOT restrict your calories if you have Hypothyroidism for weight loss. It will only make your thyroid function worse in the long term.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Losing Weight is About Balancing your Hormones
While calorie restriction may be an important part of losing weight, you have to look beyond the calories and into your hormones.
If losing weight was as simple as burning more calories than you consume we wouldn’t see graphs like this:
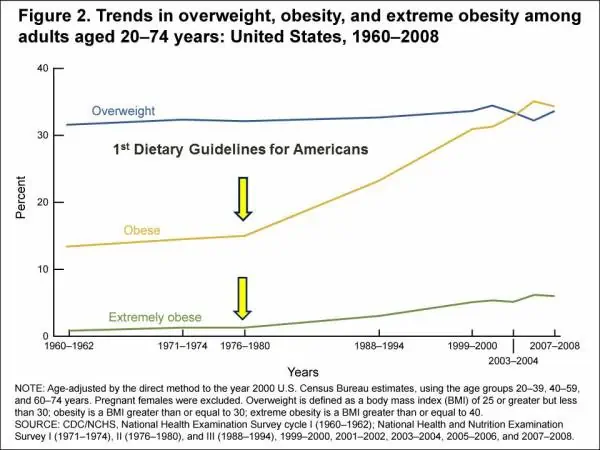
Because we know that people have been exercising more than ever and cutting back on the number of calories that they consume and they’ve been doing this for 30+ years.
So, back to the hormones for a minute.
Your hormones are incredibly powerful and they play an important role in how your body processes calories.
You can think of your hormones as gate-keepers that direct calories to the tissues that need them.
For instance:
Under the influence of insulin, your body may direct calories to your fat cells for storage as opposed to your skeletal muscles (4).
In this setting, you wouldn’t want to have increased insulin because that would result in fat cell growth.
Under the influence of testosterone, on the other hand, your skeletal muscles take up calories and energy to burn it and produce muscle growth (5).
Would you rather have your fat cells take that energy or your muscle cells?
The answer is obvious, but what you don’t realize is that the distinction between these two events is not the number of calories that you consume but the absolute level of each hormone.
When you understand this simple idea it’s easy to understand how you can gain fat mass despite eating a “normal” amount of calories.
Losing weight and keeping it off is, therefore, about optimizing the relative concentrations of these hormones to help put your body in a state in which it can burn calories without storing them.
And, this process is well-studied and not very difficult to follow.
The problem is that the vast majority of physicians are not trained in how to manage hormone imbalances, it’s just not what they were trained to do.
But that doesn’t make this information any less valid as there’s plenty of research to confirm how these hormones influence fat mass, muscle mass, and weight gain.
Let me go over some examples of how this works to help you understand what I’m talking about here.
Real Patient Case Studies & How They Lost Weight
These are all real-life patients from my practice. Once you have the right understanding of why people can’t lose weight, and you know what to test for, it becomes easy to treat patients with weight loss resistance.
Before we get into the most common hormonal imbalances we need to start with the basics.
If you want to lose weight you will have to optimize your thyroid function FIRST.
None of the other hormonal systems will come into balance if your thyroid function looks like this…
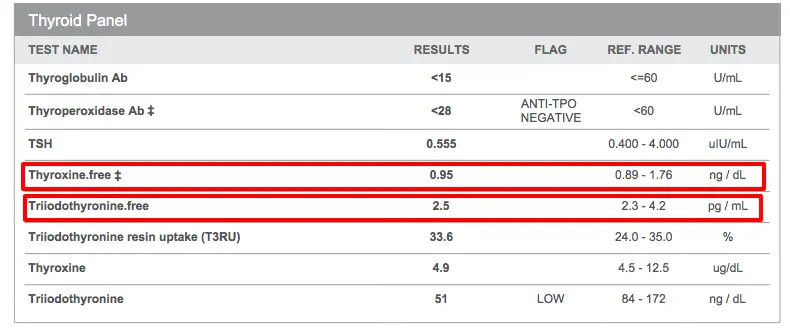
This is technically a “normal” test, but this patient had ALL of the symptoms of hypothyroidism, and yes was told her labs were “normal”.
Once she was given thyroid hormone (Armour thyroid in this case), she lost weight and had an almost complete resolution in her symptoms.
This concept holds true for patients that are being under-treated or are being treated with the wrong type of medication too!
Before you check other hormones, start with your Thyroid function.
You can find 4 simple tests to see if your thyroid function is up to par here.
I’ve found that most patients do better on some form of T3 in their thyroid hormone.
That means Natural Desiccated Thyroid or some form of Liothyronine either by itself or with Levothyroxine.

Once you feel your thyroid function is optimized then you can jump into evaluating and testing for other hormonal imbalances.
#1. Insulin Resistance, Elevated Blood Sugar, and Pre-Diabetes
We are discussing insulin resistance first because it’s incredibly common and many patients aren’t aware that they suffer from it.
From a purely statistical standpoint, you have about a 1 in 2-3 chance (or 50%) of having pre-diabetes or diabetes as an adult in the US.
The CDC estimates that around 84.1 million people in the United States have pre-diabetes and around 30.3 million people have diabetes.
Insulin resistance is the condition that leads to diabetes, pre-diabetes, high blood sugar, heart disease, Alzheimer’s, and so on.
The reason that this condition can go unnoticed is that, initially, insulin levels tend to rise before blood sugar rises.
So, if you are only looking at blood sugar then you may miss the early diagnosis of insulin resistance.
One of the best ways to identify insulin resistance early is by evaluating serum fasting insulin levels (in addition to blood glucose).
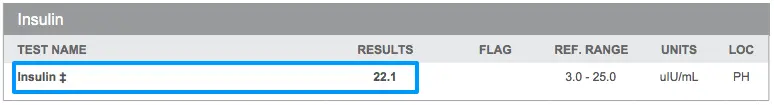
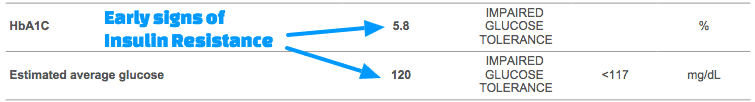
In this example, you can see that this patient has pre-diabetes based on her Hgb A1c, but she also has an extremely high fasting insulin of 22.1 uIU/mL.
The best “range” for weight loss, when it comes to insulin, is as low as possible but ideally less than 5 uIU/mL.
Excessively high levels of insulin will block your body from burning fat as an energy source and it does this by manipulating an enzyme known as hormone-sensitive lipase (6).
The net result will be an increased appetite and the need for frequent snacking in order to maintain blood glucose.
As you can see from the image above, in order to burn fat as an energy source insulin levels must be low.
In this patient, we were able to help drive down your insulin levels by focusing on a number of treatments including:
- Intermittent fasting regimen (7) (variation of calorie restriction)
- Medications designed to lower insulin resistance
- Supplements designed to lower blood sugar and insulin resistance
- Exercise routine (8) (strength training and interval training)
- Changes to her diet
These strategies work incredibly well for many patients and even work for those suffering from diabetes (9).
Quick tips to remember if you are suffering from insulin resistance:
- Lab Tests: Check fasting insulin levels (this should be < 5), Hgb A1c (should be less < 5.3), and fasting glucose levels (should be < 85). If you are doing a fasting protocol make sure to check your fasting insulin level at the end of your fast to ensure that your level is < 5. Do NOT attempt fasting if you are on insulin as it may cause harm due to hypoglycemia.
- Treatment: Find a Functional Medicine doctor who will work with you on the following: LCHF diet (if appropriate for your thyroid function and adrenal function), intermittent or prolonged fasting programs, and high-intensity interval training. If you are looking for supplements I recommend the following: Berberine and Curcumin. Berberine has been shown in studies to be as effective as Metformin in lowering Hgb A1c (10) and Curcumin has been shown to prevent the onset of diabetes from pre-diabetes for 9 months (11).
#2. Thyroid Resistance and Leptin Resistance
Thyroid resistance and leptin resistance are both seen in patients who have undergone metabolic damage from repeated yo-yo dieting.
Yo-yo dieting refers to a state in which your body weight is constantly fluctuating.
Each time you undergo a new fad diet you are able to lose some weight but that weight returns after you stop the diet.

This process continues on and on over years and the constant fluctuation causes a series of hormone changes that can be measured and tracked in your body.
Repeated weight loss and weight gain result in leptin resistance.
Your fat cells are supposed to tell your brain when they are “full” which is supposed to trigger your brain to increase metabolism to burn up the extra fat.
The repeated weight loss/weight gain cycle disturbs this communication and results in a condition where your brain becomes less sensitive to the hormone leptin.
Your fat cells produce leptin but your brain is resistant to the message.
So your brain thinks that leptin levels are low when, in reality, they are very high.
This results in a reduction in your metabolism and an increase in your appetite (13) which are the hallmark symptoms of leptin resistance.
Leptin also appears to have an impact on your thyroid function and vice versa.
We know that your thyroid helps to control your metabolism and we also know that leptin plays a role in regulating both metabolism and thyroid hormone.
In addition, studies have shown that calorie-restricted diets tend to cause changes to your thyroid function which limit the active thyroid hormone T3 (14).
It could be that dieting and repeated weight gain and weight loss cause the following chain reaction:
- Dieting causes low free T3 and high reverse T3
- These changes in thyroid hormone trigger the release of leptin to try and improve metabolism
- The brain becomes resistant to increasing leptin levels and you become leptin resistant
- The more you continue to diet to lose weight the more damage to your thyroid you incur which worsens leptin resistance
Your lab results, if you suffer from this condition, may look something like this:

An elevated fasting leptin, in the presence of obesity, is a sign that you may be suffering from leptin resistance.
You’ll probably also find if you order a complete thyroid lab panel, that your free t3 and total T3 are probably also low.
The lab results you see above are from a patient who had a history of repeated HCG dieting.
These diets are notorious for causing damage to your metabolism and may ultimately lead to leptin resistance.
In these situations, treatment must focus on both thyroid dysfunction and leptin dysfunction.
T3-containing medications are particularly effective at improving free T3 and total T3 levels while other medications, such as GLP-1 agonists, can help treat leptin resistance.
Think you have Leptin resistance or thyroid Resistance?
Here’s what you need to do:
- Lab Tests: Check fasting serum Leptin levels (< 12 is considered normal), anything > 12 is considered Leptin resistance. Check your Free T3/Reverse T3 ratio. This will tell you if you have too much thyroid-blocking hormone relative to free and active Free T3. Your ratio should be > 0.2 (anything less is thyroid resistance).
- Treatment: Thyroid resistance responds best to NDT and/or Liothyronine or sustained release T3. You should monitor Reverse T3 levels regularly while on T3 to find out when you “wash” out the reverse T3 levels. Once they go down to < 5 you can back down on Free T3 levels. About 2/3 of patients respond to NDT and about 1/3 will need Pure T3.
#3. Estrogen Dominance & Low Progesterone
Estrogen and progesterone are both considered to be sex hormones and very important for female growth and development.
Think about it:
Estrogen helps to develop breast tissue, and ovarian tissue (15), helps regulate your menstrual cycle (16), and the decline in estrogen is what triggers menopause (17).
Excessively high estrogen is a condition that results in PCOS, menstrual irregularity, PMS/PMDD, endometriosis, and so on.
This condition is often referred to as ‘estrogen dominance’ which simply means that you have an excessively high level of estrogen in your body.
The main problem with excess estrogen is that it can lead to weight gain and fat cell growth.
This growth is usually concentrated in specific areas of the body including the hips, butt/gluteal region, and thigh region.
This fat cell growth is a good thing when it’s under control. After all, it is the growth of these areas which gives women their curves and the characteristic female phenotype.
But, when the growth is excessive then it becomes a problem.
Estrogen dominance is also becoming more and more common.
Obesity, lack of exercise, insulin resistance, declining progesterone, and hypothyroidism can all lead to excess estrogen.
Estrogen dominance tends to occur in 3 different ways (and each is important for understanding how to treat it):
1. Too much estrogen with “normal” progesterone levels.
2. Too little progesterone with “normal” estrogen levels.
3. Excessive exposure to xenoestrogens from the environment with “normal” estrogen and progesterone levels.
Usually, most women know if they have an estrogen/progesterone imbalance simply based on their symptoms alone.
High levels of estrogen tend to cause very specific symptoms which are hard to miss.
Testing for both estrogen and progesterone can be done through routine bloodwork.
However, when testing for estrogen and progesterone, it’s important to remember that these levels are constantly in flux due to the menstrual cycle.
The best time of the month to test for these hormones is during the mid-luteal phase or between days 19-21 of the menstrual cycle.
You should then look at the relative difference between both estrogen and progesterone to determine if your values are “normal”.
It’s helpful to have an idea or a baseline set of labs to compare your results with considering that each woman will have a different definition of “normal”.
More advanced testing also exists:
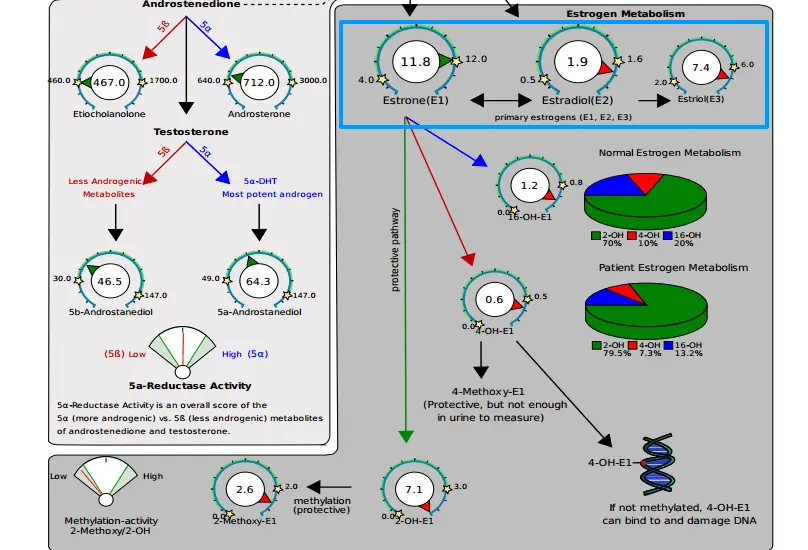
Urinary levels of both estrogen and estrogen metabolites (estradiol, estriol, and estrone) can help you understand how your body is processing and metabolizing estrogen.
In this example above you can see that estrogen is being blocked at the last stage of elimination.
Once we optimized her liver function, put her on herbs to help eliminate estrogen down the protective 2 hydroxy pathway (18), and opened up her ability to methylate with activated B vitamins, she was able to lose weight and eliminate excess estrogen.
If you think you are suffering from estrogen dominance you can do the following:
- Lab Tests: Check serum estradiol and progesterone at the same time on days 19-22 of your menstrual cycle. You can also order more advanced tests via urinary estrone, estradiol, and estriol plus metabolites (16-hydroxy Estrone, 4-hydroxy Estrone, and 2-hydroxy Estrone) on day 19-22 of the mid-luteal phase of your menstrual cycle.
- Treatment: Clean up and improve liver function, increase consumption of cruciferous vegetables (19), consider FAR infrared sauna use, and consider supplementing with DIM or Indole-3-Carbinol to help metabolize excess estrogen through the liver. Depending on progesterone levels you may also benefit from using Bio-identical Progesterone cream.
#4. Low Testosterone with Insulin Resistance
We often tend to think of testosterone as a male sex hormone but it’s very important for women too.
In women (and men), testosterone helps build lean muscle mass, helps promote fat loss, helps control your libido (20), and helps regulate your mood.
Women with low testosterone may feel “flabby”, find it difficult to gain muscle mass, find it difficult to lose weight, and may experience mood problems like irritability or depression.
Low testosterone can even contribute to a low sex drive or decreased libido!
Testosterone can be easily tested in the serum by ordering free and total testosterone:
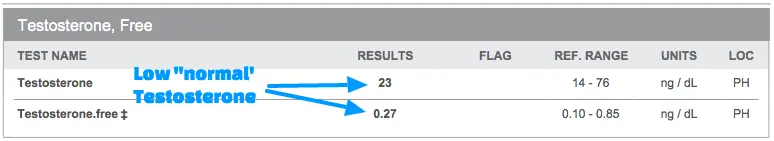
Low testosterone is very common among women as they age (much like men) and in certain medical conditions including hypothyroidism.
This patient has low-normal testosterone lab tests but was experiencing symptoms including decreased libido and weight gain.
Upon replacement, these symptoms subsided rapidly.
In addition, testosterone (especially in women) can be impacted by other hormones such as insulin.
Insulin resistance and high blood sugar can negatively impact testosterone and lead to low testosterone or high testosterone (21) (depending on the woman):
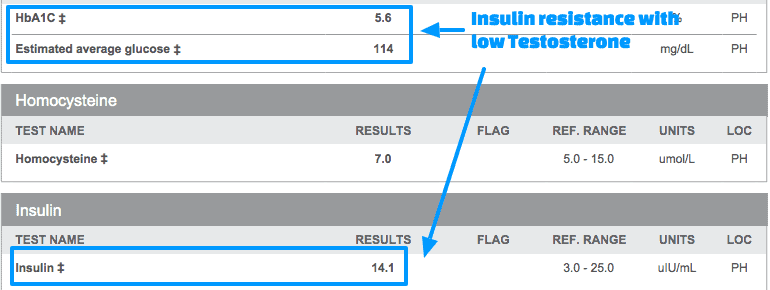
This particular patient was suffering from both Low testosterone and insulin resistance.
Insulin and resistance and testosterone dysregulation are often seen together and it’s very important to treat both if weight loss is your goal.
In this patient, once we gave her some bioidentical low-dose testosterone she was able to lose weight, build muscle, and improve her mood.
In addition, it was easier to reverse her insulin resistance as opposed to using dietary measures alone.
If you think low testosterone and/or insulin resistance is contributing to your weight loss resistance consider these steps:
- Lab Tests: Check free and total Testosterone. Optimal levels depend on the patient and their symptoms, however, in general, I like to see testosterone in the mid-range for women unless they have a history of autoimmune disease or Hashimoto’s. Patients with autoimmune disease tend to have both low DHEA (22) and testosterone levels and may do better with high-normal levels.
- Treatment: If Testosterone levels are low I would consider using bio-identical testosterone cream. Start low dose and check testosterone levels after 4-8 weeks. Also, check for insulin resistance and treat aggressively if present, treating insulin resistance may cause a natural increase in Testosterone levels.
#5. Adrenal Fatigue with Elevated Cortisol
Adrenal fatigue is another extremely common hormonal imbalance in patients with hypothyroidism.
Cortisol is a hormone that your body calls upon in times of stress and why it is considered to be the ‘stress hormone’.
One of the main issues with cortisol is that it appears to be connected or linked to thyroid hormones in some way.
As thyroid hormone changes it impacts cortisol.
In hypothyroid states, it’s possible for cortisol to become dysregulated either in absolute value or at the receptor level.
In either event, the end result may be decreased weight loss or weight loss resistance.
Excessively high levels of cortisol also contribute to hormone imbalances such as insulin resistance.
And long-term exposure to cortisol has been shown to contribute directly to weight gain, especially in the belly area (23).
Patients with cortisol dysregulation often experience the following symptoms:
- Extreme fatigue
- Weight loss resistance
- Weight gain especially in the belly
- Food cravings for sugar and salt
- Feeling “wired but tired”
- Anxious or jittery feeling
You can test for cortisol with a simple serum blood test but there are also many other ways to assess for cortisol including urinary and salivary levels.
Always start first with an 8 am serum cortisol level and then work your way into other tests as necessary.
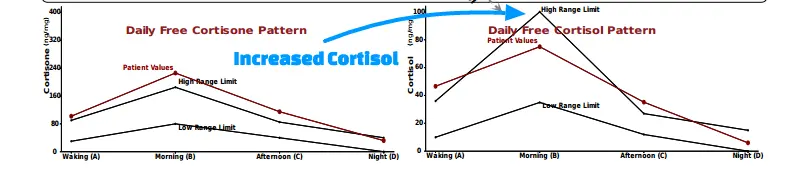
The image above represents a series of 4 cortisol urinary tests throughout the day.
You can see that the cortisol levels spike in the early morning around the time that most people consume coffee or caffeine.
This type of pattern is common among those with high-stress jobs, those who sleep 6 or fewer hours per night, and those who are under constant stress.
This particular patient was experiencing persistent weight gain and dealing with the other symptoms of adrenal fatigue.
Treating cortisol dysregulation can be accomplished with adaptogenic herbs and supplements, by reducing your exposure to stress and by cutting back on caffeine.
If you suspect that you have abnormal cortisol levels then consider these steps:
- Lab Tests: Start with serum cortisol. From there you can determine if salivary or urinary cortisol is necessary.
- Treatment: If Cortisol levels are elevated consider a combination of the following: removing caffeine and stimulants, adding higher doses of salt into your diet, eating smaller more frequent meals, using stress reduction techniques, and supplementing with adrenal glandulars or adaptogens. All of these therapies have been shown to be effective at reducing the negative impact stress has on the body.
How to Test for these Hormonal Imbalances
If after reading the above section you think you have a hormonal imbalance simply go down to the area and look at the tests.
It will show you which tests you need to order to evaluate your hormones and show you the reference levels your results should fall into.
Remember that there is a big difference between being “normal” and being “optimal”.
Don’t let someone tell you that your labs are “normal” if you feel like crap. It’s not that your labs are normal, it’s that the doctor isn’t ordering the right tests or he/she isn’t interpreting them correctly.
Testing For Hormonal Imbalances
| Test | Optimal Levels for Health | |
| Thyroid Deficiency | Blood: · TSH, Free T3, Free T4, Reverse T3, Thryoglobulin Antibodies, Thyroperoxidase Antibodies, Sex Hormone Binding Globulin (SHBG), Ferritin, TIBC, Serum Iron | TSH: < 2 Free T3: 1/3 of reference range Free T4: 1/3 of reference range Reverse T3: < 15 Thyroglobulin: <15 Thyroperoxidase: < 15 SHBG: · Male: 20-30 · Female: 70-80 Ferritin: 70-80 Serum Iron: Mid range TIBC: 35-38% |
| Estrogen Dominance | Urine: · Estrone, Estradiol, Estriol, 16-hydroxy Estrone, 4-hydroxy Estrone and 2-hydroxy Estrone | Optimal levels highly variable, must be compared to Progesterone and in the setting of symptoms. Generally 2-OH Estrone should be preferred over other pathways. |
| Progesterone Deficiency | Blood: · Progesterone Urine: · Pregnanediol | Check on day 19-22 of Menstrual cycle if menstruating. Progesterone levels should be higher than Estrogen levels during days 19-22 (see image below). |
| Insulin Resistance | Blood: Insulin (Fasting and 2 hours after meals), Hemoglobin A1c (Hgb A1c), Fasting blood sugar (FBS), Uric Acid, Fasting Triglycerides, Fasting HDL | Insulin: · Fasting: < 5 · 2 hours after meal: < 30 Hgb A1c: < 5.3 FBS: < 85 Uric Acid: < 5 Fasting trig: < 100 Fasting HDL: > 60 |
| Leptin Resistance | Blood: · Leptin levels · Thyroid studies (above) · Insulin tests (above) | Leptin: < 12 |
| Cortisol and Adrenal Fatigue | Urine: · Cortisol and Cortisone x4 Salivary: · Cortisol x4 Blood: · AM Cortisol (Not very accurate) | Range is dependent upon the person and is relative. If Cortisol levels are low = Late stage adrenal fatigue. If cortisol levels are high = Early stage adrenal fatigue. |
Conclusion
Weight loss is definitely possible if you have thyroid disease but it takes the right approach.
This approach includes the evaluation of your hormones, including those beyond your thyroid.
By evaluating, diagnosing, and treating these imbalances you will be able to not only lose weight but keep it off.
While some of this information may be new to you just remember that many of these conclusions have been drawn as the result of clinical research and real-patient experiences.
You may need to read through this one or more times to let everything sink in.
It is also helpful to grab your own set of labs and compare your lab results to the patients listed in this guide.
From there you can determine the similarities or differences between you and them which may be able to help guide your treatment.
But, remember, that you are an individual and even if your test results may look similar, it doesn’t mean that you need the same treatment.
Ensure that you get the proper work-up if you think your hormones are out of balance because you shouldn’t have to go through life feeling like you’re crazy because your labs are all “normal”.
Many patients feel vindicated when they realize they actually do have abnormalities in their lab results, they just needed someone with the right knowledge to evaluate them.
Now it’s your turn:
Are you suffering from hypothyroidism?
Is it also difficult for you to lose weight?
Has anything worked well for you?
If not, why?
Leave your questions or comments below so that we can continue the conversation and continue to help future people!
Scientific References
#1. https://www.ncbi.nlm.nih.gov/pubmed/1436373
#2. https://www.ncbi.nlm.nih.gov/pubmed/10378389
#3. https://www.ncbi.nlm.nih.gov/pubmed/3757921
#4. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC380258/
#5. https://www.ncbi.nlm.nih.gov/pubmed/2917954
#6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC333098/
#7. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5394735/
#8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4625541/
#9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3168743/
#10. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2410097/
#11. http://www.ncbi.nlm.nih.gov/pubmed/22773702
#12. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4069066/
#13. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3281561/
#14. https://www.ncbi.nlm.nih.gov/pubmed/12055988
#15. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3652894/
#16. https://www.ncbi.nlm.nih.gov/books/NBK279054/
#17. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2717878/
#18. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4505810/
#19. https://www.ncbi.nlm.nih.gov/pubmed/1656396
#20. https://www.ncbi.nlm.nih.gov/pubmed/26358173
#21. https://www.ncbi.nlm.nih.gov/pubmed/18319314
#22. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2701249/
#23. http://www.ncbi.nlm.nih.gov/pubmed/11020091









It sounds like I have the leptin issue. My T3,T4 are normal. My TSH was 3.9, but now I am on the lowest dose of Armour and last I checked it was 2.7. I am wanting to go off my medicine and heal it. I eat very healthy and am having a hard time losing the weight I gained from this. What do I do to deal with the leptin?
Hey Heather,
The best way to find out if you are suffering from leptin resistance is to check it in the serum. I recently wrote an article about treating and reversing Leptin resistance and thyroid resistance which typically go hand in hand. You can check out the article here: http://www.restartmed.com/leptin-resistance-thyroid-resistance/
I also recently wrote about how to increase free T3 levels naturally which may be beneficial to you as you go off of your medication, you can check that one out here: http://www.restartmed.com/increase-free-t3-naturally/
Good luck!
I had the radio active iodine treatment 20 years ago I was hyperthyroidism Gained 30 lbs after and have felt like a yo-yo since I can’t lose weight .. my TSH is 0.25 I’m on levothyroxine 188mcg I’m still waiting for my dr to order a new dosage to help me hoping this booster will help I just purchased from you and received it today
Hi Priscilla,
T3 Conversion Booster likely won’t help you lose weight but it will likely help improve your thyroid. I would recommend reading this article for more information on the topic of weight loss post-RAI: https://www.restartmed.com/weight-loss-after-thyroid-removal/
Hi Dr. Childs my doctor has me on a higher dose of T3 , what would be you limit on T3 per day ? I guess what I am asking is do you feel 100 mcgs of T3 a day a lot or have you given that much before ?
Hey Ellen,
It depends on the patient. I’ve gone as high as 100mcg per day but it’s not something I would keep a patient on long term.
Thanks I am trying to finish my year out with my doctor and will be contacting you if my $$ allow ! I have Hashimotos , very overweight , high insulin and leptin . Right now more worried about all the weight more so then anything . I do not convert well , how long would you keep a patient on a high dose of T3 ? How long is safe ? And also I have read that high doses cause muscle wasting ?
Also following AIP diet , I read in your page that you don’t really go with AIP what do you follow ?
Thanks
That concerns me as my Dr. just upped my dose to 100 mcg and she seems fine with me being on it forever. She is, according to my chart, treating my hypothyroidism and not the Hashimoto’s she diagnosed me with last week. I got your book, and plan on healing myself since my Dr. seems unconcerned.
Hey Kate,
Read through it and check out some of the other resources on my site, they can help give you some direction.
I was diagnosed Underactive 10 years ago but know that I was subclinical previous to that but Dr’s wouldn’t treat because my test result didn’t show it. I have struggled with maintaining a healthy weight and do eat healthy. Currently I’m battling with many symptoms I feel are thyroid related including the inability to shed weight. I was running marathons last year and doing 25 miles week in training with absolutely no reduction in size. I cannot recall a time that I have had anything but TSH done and wonder if it’s time I suggested further tests to my GP without been fobbed off.
Hey Sarah,
It’s unlikely, if your Doctor knew their value he would have ordered them long ago.
I don’t understand your response. So many women, myself included, only got the standard test which indicated “normal” range. Problems were persistent and finally I found a Doctor who would listen. I saw the site Stop the Thyroid Madness…
I have been getting help with my wild lab results. I am still not losing weight even though I am on 115 of T3 and a slew of other supplements like cortisol, adrenal repair, vit d, liver support etc…please do go to a Dr. who has more insight than your regular GP. Good luck!
Very interesting stuff. I have no thyroid, they removed the whole thing because they said it was 85% its cancer. It wasnt, it was some kind of follicular neoplasm….anyways i gained 15 lbs the 1st 2months, then up total 28lbs by the 5th month and i gained in 10mths 56lbs. Do u help people with no thyroid?
Hey Andrea,
Yes, I have helped many patients post thyroidectomy lose weight.
Hi Andrea
It’s pointless to even ask about losing weight after losing your thyroid “no one gets it” Im like you I lost my thyroid to cancer and managed to magically packed on 50lbs like its been my part-time job and I get no help or answers and lets not forget the MASSIVE AMOUNTS of body pains that have also hitched a ride after my thyroidectomy 2 yrs and I walk like I’m 90 I’m only 48.
Thyroidectomy is a life sucker.
Hi Grace,
All of those symptoms can be addressed, you just need to find someone with the right approach. The general solution to both problems is to use the right amount of T3 thyroid hormone. The main issue is that most conventional doctors (including endocrinologists) do not take this approach. You can find more information on both topics in these articles:
https://www.restartmed.com/weight-loss-thyroidectomy/
https://www.restartmed.com/hypothyroidism-chronic-pain/
https://www.restartmed.com/low-t3/
I was recently diagnosed with hypo. My TSH was 5.88 and Doctor started me on 25 mg Levothyroxine. Going back to get Free T4 checked. I’ve gained 60 pounds in a year. Struggling to lose weight. My daughter also has Hypo and Hashimoto’s and is insulin resistant. I’m more worried about her since she’s 18 and hasn’t lost any weight in the 4 years since being diagnosed. She’s on 125 mg Levo. Any suggestions? Should we try Armour?
Hey Martha,
If your only treatment so far has been a small dose of levothyroxine you are not heading in the right direction, I would recommend looking for someone who is hormone literate to help you further.
Hi,
I’ve always been overweight but several years ago, I lost over 130lbs but am still in the obese category being 240lbs and 5′ 8”. I was diagnosed with hypothyroid about 7 years ago. Was first on levothyroxine but I asked to be changed to Armour almost 2 years ago. My TSH is 3.53, T3 is 142 and thyroxine, serum free was 0.79 in Sept. The last number is low but my doctor decided not to change my dosage because he said it would raise one of the other levels too high (?) and I had also lost 7 lbs during that visit. I did have a morning cortisol test in 2015 and it was 10.4 UG/DL but he didn’t discuss what this means. But the same few pounds keep coming back instead of losing more. So, I continue to struggle to lose weight. Whats even more frustrating is that I am a fitness instructor and teach 4 spin classes a week and 2 water aerobics classes and am VERY disciplined with my eating and track daily. I eat enough, not too little and not too much, more on the low carb end. I don’t understand whats going on. Any advice?
Hey Delo,
You can find more information about weight loss here: https://www.restartmed.com/hormone-mastery/
Hi there!
I have Graves Disease which put me into thyroid storm at 30, and I eventually I had to go through RAI. The disease attacked the fatty tissues behind my eyes and I have pressure every now and then, which seems to reduce after acupuncture. (I’m pretty lucky…double vision has disappeared completely). Anyway, I’m on NDT and feel so much more alive. Like the fog has lifted. The problem is that I’m tired and wired, and I most often feel too tired to be active or work out. My hair is not growing back. I have plantar fasciitis and back aches. I experience heavy periods monthly, a dull complexion and sensitive shins. What are the best supplements for these issues? I’m thinking B12, selenium, vitamin D…but do you recommend others?
By the way, Do you recommend anyone in Ohio? A lot of our Cleveland Clinic doctors are close-minded. I found one who agreed to NDT, but they won’t consider looking into anything else for me. I really need someone like you…God bless you for all of your hard work and talent!
Hey Lauren,
I don’t know anyone in Ohio who practices like me.
Lauren,
I realize your question was for doc but I had heavy periods myself for a LONG time until this….My doctor(s) told me I was anemic for years and told be to supplement with iron. I was very wishy washy with taking it until I started having heavy periods. I ran across a YouTube video and found out that taking the iron (along with some vitamin C to help absorption. I take a chewable with it or orange juice) would completely fix this issue. And it did! Now I take my iron religiously and NO MORE heavy periods! So, even if you haven’t been told you are anemic, ask your doc to check. This will also help with your being tired. Iron is what delivers oxygen to your blood.
Just my two cents.
Thank you…I will definitely look into that Delo!
Hi: I have Hashimoto’s and am on 100 mg. Synthroid and 5 mcgs of Cytomel for about almost six years. I can’t seem to lose any weight. I do lose about 5 lbs, as you say, and then that’s it. I gain it right back. And my weight always goes back to the same weight. Do you know anyone in CT who practices the way you do or do most Naturopaths treat as you do?
Thanks in advance.
Grace
Hey Grace,
I am not a naturopath so I can’t speak to how they practice, but I can tell you that the information you see here is self taught/researched, as a result I don’t know anyone who practices this way.
Ok then. Would a naturopath who practices functional medicine be able to help me? I understand about the information being self taught but you still need someone to order the right tests? do you not? Isn’t that an important part of the whole problem?
Do you know someone in Ct who practices functional medicine that also understand how this works?
Thanks.
Grace
Hi there,
I have been having symptoms of constipation, weight gain, struggling very much so to lose even a pound with exercise and very healthy diet, cold fingers, fatigue and low sex drive for about 2 years now.
I’ve had my TSH checked twice in the last 2 years by my PCP at my physicals just find out they’re “normal” but I still have all these systems with no plan.
Recently (within the last month) I had it rechecked through a local “performance medicine” office and they determined it subclinical (3.14) but also noted my Vitamin D levels were significantly low and my testosterone extremely low and was only 13. She started me on 16.5 of nature-throid, thrysol and Vit D supplements a week later. I am feeling no changes and still gaining weight 3 weeks later. She wants me to stick to this medicine for a full 30 days first before increasing dosage.
I’m curious if the testosterone cream would help as you mentioned above? I was reading about the insulin resistance? How is this checked? I’m also on a low dose birth control (trinessa lo) and am curious if that’s interfering with things also. It’s very frustrating not being able to lose weight when in the gym 4x a week and eating healthy, drinking lots of water and sleeping great. What are your thoughts?
Hey Grace,
You can find more information on how to use testosterone here: https://www.restartmed.com/low-testosterone-women/
Dr. Child’s I am a horrible mess. Diagnosed 17 years ago with hypothyroidism. As I approach mid 40’s my weight has Yo-Yo’d. I read information you provided and I have tried all the diets you mentioned. I am at my heaviest since birth of my daughter 17 years ago. I have been on 100mcg of synthroid since diagnosis. My labs always come back normal. I have requested a referral for a endocrinologist. My doctor seems reluctant on giving me this.( We have tricare) not sure if this matters. I am absolutely at end of my rope. I work out eat healthy but recently fatigue has taken its toll. I am completely exhausted after exercise and just want to lay down. Melancholy has taken over my life as well.
Hello!,
Thanks for the article! VERY eye opening! I have a question about #4. You mention that if “insulin resistance is present, treat aggressively.” How do you suggest doing this??
Thanks.
Hey Danielle,
You can find more info here: https://www.restartmed.com/insulin-resistance-diet/
Hello Dr Childs,
First of thanks for great insights and sharing this knowledge! God bless you!
I have a quick question regarding estrogen metabolism…. I have done my DUTCH test and it shows methylation ratio [2-methoxyestrone/2-hydroxyestrone] = 0.2 (low)
How can i improve this ratio? Can Lipotropic shots help? I have much more fat on hips/thighs and side hips…
My other rations are low too:
1) 2hydroxyestrone/16hydroxyestrone = 1.5 (low)
2)Andro/Etio (5 reductase) = 0.5 (low)
3) DHT < 0.3
4) 5 alpha -THF/THF (5 reductase) = 0.4 low
How can improve on above?
Please advice
Thanks.
hi dr child’s.
i wonder how much of all this info is valid for men too?
Hi George,
All of it is relevant except the focus on estrogen/progesterone.
Do you have a DR that you recommend in the Twin Cities area. I have been trying to lose weight for 3+ yrs. I have been diagnosed with Hashimotos, and I would like to work with someone who would follow what you say above?
Hi Amy,
Unfortunately I don’t know anyone in that area to recommend.
Great article! I have a question about estrogen dominance. I was diagnosed mildly hypothyroid and placed on Nature Throid about 3 years ago – luckily only about 10-15 pounds overweight.
I have a lot of other probably related diagnoses – premature ovarian failure since the age of 26 which has had me on and off hormone replacement therapy for nearly 25 years. Endometriosis, fibrocystic breast tissue, and small fibroids. Decades of IBS-D and SIBO. 7+ years of SSRI’s for chronic anxiety. And a history of calorie restriction, sometimes quite extreme. Oh, and adrenal fatigue.
My FMP at the time helped to treat everything, but said I was estrogen dominant. I understand that some of my history points to estrogen dominance, but part of my POF diagnosis was that my estrodiol was consistently at zero (or unmeasurable levels) and my FSH was above 90.
How can someone be estrogen dominant, but not make any measurable level estrogen? Thank you!
Can you recommend anyone in the Maryland, DC, Virginia area? I am on Armour, finally, after many fails with doctors not wanting to put me on it. I don’t get headaches anymore but I keep gaining weight. I have about 40 lbs that I need to lose. I can’t lose it no matter what and have a cravings for sugar. If you have anyone near me you could recommend, that would be great. Thanks.
Hi Jacqueline,
Unfortunately I don’t have anyone that I can refer you or I would gladly give you that information!
You might find further help here: https://www.restartmed.com/hormone-mastery/
Check out Dr. Denise Bruner in Arlington, Va. She is open to this type of information and gives some of it as well.
I have had my thyroid removed due to cancer. I have gained 40 lbs in 2 years. I have considered Optavia but am hesitant. Is there anything that can assist for people w/o throid?
Hi Tammy,
You can find more info on how to lose weight after thyroidectomy here: https://www.restartmed.com/weight-loss-thyroidectomy/
You can also find more info related to hyperthyroidism here: https://www.restartmed.com/category/thyroid/hyperthyroidism/
I was initially diagnosed with Hashimoto, and was put on thyroxine 50mcg. Now I take 100mcg 3 times a week and I feel better in many ways but my weight has been steadily increasing and I find it extremely hard to lose weight. Been on a very clean diet and exercise 6times per week for 3 weeks now and lost 1 kg!!
I have had this for 41/2 years and increased about 15kgs over the last 4 years.
Had bloods done last week n the doctor only did tsh, free t3 and free t4 even though I asked for everything including hormones etc.
Results
Tsh – 0.22
Free t3 – 4.6
Free t4 – 19
Hi Grace,
You’ll also want to evaluate your sex hormones (estrogen and progesterone). Changes to these hormones can worsen thyroid function and lead to weight gain in perimenopause/menopause.
Thanks Dr Westin for the recommendation. I am 33years old, but got the estrogen & progesterone test done anyway.
My results are:
FSH 2.1
LH 4.2
Progesterone 35.2
Oestradiol 502
HDL Cholestrol 0.97
Throperoxidase Antibodies >1300
Ferritin 38
Hi. I need some help. I had thyroid cancer and a thyroidectomy. I take levothyroxine. My doctor keeps my thyroid function at 0 to try to keep cancer from returning. I have PCOS, I am diabetic and have a fatty liver. I fight a battle with weight loss. Is there anything I can do to help with the weight loss? I am currently doing weight watchers with very little results.
Hi Misty,
Unfortunately, weight watchers isn’t likely to work because it is based on calorie restriction. I would take a look at this post which should help: https://www.restartmed.com/weight-loss-thyroidectomy/
Thanks Dr Westin for the recommendation. I am 33years old, but got the estrogen & progesterone test done anyway.
My results are:
TSH 0.22
Free T3 4.6
Free T4 19
FSH 2.1
LH 4.2
Progesterone 35.2
Oestradiol 502
HDL Cholestrol 0.97
Throperoxidase Antibodies >1300
Ferritin 38
I am struggling to lose weight even after following a very restricted diet. I am now avoiding gluten, lactose, cruciferous vegetables, coffee and processed food & rice(I eat quiona & brown rice occasionally). I am also doing HIIT workouts and go for walks when time permits (2-3 times/week). Lost just over 1Kg after 1 month of the above.
I don’t understand why you don’t put people on cytomel long term as long as it is slow released why would you not if they are not converting right? You could be chasing your tail a long time with a t4.
Hi Ashley,
I’m a little confused by your comment. I do put people on T3 long-term but some people don’t need it long-term and can be taken off of it. Perhaps you are confused about the reasons why you wouldn’t need to be on it long-term vs short-term.
Hi Dr. Childs,
I had a total thyroidectomy about 2.5 years ago. I can’t lose weight no matter what I do. Most recently I barley lost 5lbs doing the keto diet for about 4 months 🙁 I know something is off, I just don’t know what. I am planning on doing the phone consultation with you, but I was wondering if I need any other labs? I went to the “what labs do you need” section, but is that all the labs we need or is there any additional ones? Also, if our doctor is unable to get these labs done for us, do you know where we can get these done? If you have a package where we can purchase the labs too, that would be fantastic!
Thank you!
Hi Diana,
After thyroidectomy, the most common reason for weight loss resistance is insufficient thyroid hormone replacement with T3. This isn’t universal but it holds true for most patients. Unfortunately, I don’t have a package which includes labs at this time!
What kind of doctor is best to determine all these levels?
Hi Kim,
I would take a look at this article for more information on that exact topic: https://www.restartmed.com/thyroid-doctor/
Amazing information, Dr. Childs. I wish more practitioners approached medical tests and results the way you do. It’s refreshing to say the least. Thank you for this tremendously helpful information!
Hi Gianna,
No problem and glad you found it helpful!
Hi Dr. Westin,
I have low t3 and t4.. Gained weight and have swelling in my body hands and feet and ankles. I am on nature throid, and I just ordered your leptin resistance. Any suggestion in how to loose weight and get rid of the swelling and inflammation?
Hi Maria,
I would start with a complete thyroid lab panel + insulin + leptin to see where your main issues are and then target those hormone imbalances.
i am summing that the tpo of 166 is not good?
i am having such a issue getting the right care for thyriod
issues, i am now on amour , but losing my hair , still can not lose weight, tired all the time .
Dr. Childs I am a little confused. My glucose is 100 with an arrow going up. Not sure if this means it is more than 100 but my Hemoglobin A1C is 4.9 and my fasting insulin is 3.7.
Why would my insulin and A1C be normal and my glucose be higher? I do not eat sugar and simple carbs, and I eat a lot of good fats.
Hi Brenda,
Blood sugar changes hour to hour whereas your A1C is a long term reflection of your blood glucose level.
Good Afternoon,
I have been following you on youtube and I’m in desperate need of help.
My endocrinologist recommending I do a Laparoscopic sleeve gastrectomy since I have hypothyroidism & Hashimoto. Also for past two months I order from your website the
Product Price
Hypothyroid Bundle (5 Supplement Combo for FULL Thyroid Support) &
ltra Biotic X100 – Daily Potent Probiotic with 100 Billion CFU/Serving 1
rtg001 Raw Thyroid Glandular+ 1
thy001-1 Thyroid Adrenal Reset Complex – #1 Adrenal and Thyroid Support Supplement designed especially for Hypothyroid patients – Vegan & Non-GMO – 60 Day Supply 1
tcb001 T3 Conversion Booster – Naturally Support T4 to T3 Conversion 1
FFV001 Functional Fuel Complete – Thyroid Friendly Protein Powder for Hypothyroidism & Hashimoto’s on Aug 07th 2021.
Hi Evadne,
I would strongly recommend that you look at this program and do it in its entirety before opting for surgical interventions for weight loss: https://www.restartmed.com/hormone-mastery/
If you use that program you should be able to avoid the sleeve gastrectomy which is always preferred.
I was diagnosed with Hypothyroid during my second pregnancy when I was 23. 2.5 yrs ago I was diagnosed with Hashimoto’s, I went into surgery for a parathyroidectomy, because I had hyperparathyroidism, they removed 2 of my parathyroid’s and half of my thyroid. I have had so many blood tests of the last 26yrs and I think I can remember one test where my tsh levels were in range. The last test I had was the end of April and my TSH was 64.198 and Free T4 was 0.95. I take 325 mcg of levothyroxine a day. I have constant fatigue, constant muscle aches, I feel like Im 90 yrs old but I’m 46. I have gained over 100lbs and no matter what diet I try (aip, paleo, keto, ect) I cannot loose weight and keep it off. My dr has suggested lap band, or gastric, which I refuse because I know too many people who have had too many complications. I have been put on Adipex multiple times and I will lose and then gain it right back. I asked my dr the last time I was there to check my hormone levels because I just feel off all the time. He didnt do it. I adopted a 4 yr old out of the foster care system and at this point I dont know if ill be around to watch him grow up. I am not used to all this access weight which has also caused osteoarthritis in both knees and they are talking total knee replacement of both knees by the time im 50 if i cannot loose the weight. But i have literally tried everything, fasting, diets, causing myself so much pain by doing things my body shouldnt be doing. Im at loss.
Hi
Seems like every 6 months my thyroids is low after taking 188mcg levothyroxine TSH IS TESTED ONLY by my doctor (pcp)my TSH WAS 0.25 and I’m now waiting for my dr to contact me to see what new dosage of levothyroxine he will order for me next
I’m always sluggish and cannot lose weight