Do you have all of the symptoms of hypothyroidism but have been told your Thyroid lab tests are “normal”?
I’ve got some news for you…
Chances are VERY high that your thyroid lab tests are in fact NOT normal and that you are NOT crazy.
But it can feel like you are crazy when you go to Doctor after Doctor and you’re told the same thing.
So why is it that every Doctor is telling you that you are fine, despite how you feel?
Let’s talk about why your thyroid lab tests are anything but “normal”…
7 Reasons why your Thyroid Lab Tests are NOT normal
By the time most patients finally come to see me, they’ve seen 5+ different Doctors and they’ve all been told the same thing.
It can get very disheartening to hear it over and over.
It’s not uncommon for patients to come to me on anti-depressants because other endocrinologists and primary care doctors think that’s really what’s going on.
And while hypothyroidism can cause depression, most of the time I find that my patients really are suffering from hypothyroidism – they just don’t fit the typical “mold” and so they are misdiagnosed.
Let me show you why your doctor may be missing your hypothyroidism…
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
#1. Your Doctor isn’t Ordering a Full Thyroid Panel or he isn’t Interpreting it Correctly
There are 2 situations that I see commonly in my office:
- Doctors aren’t ordering the right tests and they are misdiagnosing the patient
- Patients are asking for the right tests, but the doctors (and the patients) aren’t interpreting the labs correctly.
Do you fall into one of these categories?
It’s CRITICAL to not only order the right tests but to understand how to interpret them correctly.
Otherwise, you will miss the diagnosis!
That being said…
What tests do you need to order?
The “Complete” Thyroid Blood Panel
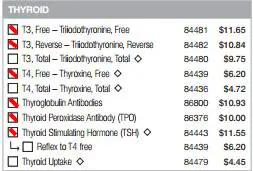
This is my “complete” thyroid blood panel that I order on every patient, let me break it down for you and why it is important…
- TSH – The TSH gives you an idea of how the pituitary is responding to serum levels of Thyroid hormone. The pituitary has different deiodinases than the rest of the body so it can’t be used a marker for tissue levels of thyroid hormone, but it can be helpful if elevated.
- Free T3 – How much active thyroid hormone is floating around in the blood. Free T3 is the free and active thyroid hormone and, perhaps, the most important thyroid lab test.
- Free T4 – This gives you an idea of what kind of thyroid “store” your body has. T4 is the reservoir hormone your body uses to create reverse T3 or free T3. Remember that not all T4 will turn into T3 and in the presence of inflammation, leptin resistance, or nutrient deficiencies your body may turn T4 into Reverse T3.
- Reverse T3 – This gives you an idea of what kind of stress the body is under, how much inflammation is going on, and what nutrient deficiencies you may be experiencing. High levels of reverse T3 are associated with thyroid resistance and tissue-level hypothyroidism.
- Thyroid peroxidase and thyroglobulin antibodies – High antibodies are associated with thyroiditis and autoimmunity. If elevated, treatment should be targeted at reducing these values. These antibodies can also cause issues in other tissues including the breast (1) and brain (2).
- Sex hormone binding globulin – This can be used as a surrogate marker for Tissue levels of thyroid hormone. Only two hormones increase this protein, estrogen and thyroid hormone.
- Iron studies – Iron studies are critical for the proper interpretation of thyroid function. In the presence of low Iron thyroid hormone will be less active.
Now, what are the “optimal” levels for these tests?
- TSH – TSH should be < 2. A TSH < 2 does not necessarily mean that your thyroid function is normal. It’s not advisable to use TSH to track thyroid hormones as newer studies show this method to be flawed (3). In addition, the pituitary has location-specific deiodinases (4) which make it different from other tissues in your body in terms of how sensitive it is to thyroid hormone.
- Free T3 – Optimal levels are usually in the upper 1/3 of the reference range.
- Free T4 – Optimal levels are usually in the upper 1/3 of the reference range. Note that Free T4 levels may drop dramatically on pure T3 hormone replacement therapy like liothyronine, Cytomel, or sustained release T3.
- Reverse T3 – Optimal levels are as LOW as possible. If > 15 I will start thinking about thyroid resistance at the cellular level or that leptin and/or inflammation are blocking thyroid hormone from getting into the cells. In the presence of High levels of reverse T3, your free T3 levels may look falsely “normal”.
- Thyroid peroxidase and thyroglobulin antibodies – Optimal levels are as low as possible. I recommend tracking these values if you are being treated for Hashimoto’s.
- Sex hormone binding globulin – Optimal levels for Women = 70-80 range. Optimal levels for men = 20-30 range. You can follow the SHBG to see if thyroid hormone is entering the tissues (in this case the liver). As you increase the dose of thyroid hormone this value should increase as well.
- Iron studies – I find that most hypothyroid patients feel better with Ferritin levels in the 70-80 range and percent saturation levels in the 35-38% range.
Remember:
Interpreting your test results is MORE important than simply ordering the right tests.
#2. Blood levels of Thyroid Hormone are not necessarily what we care about
This is another huge problem so let me explain…
I explain it this way to my patients:
The bloodstream in your body is just a way to move nutrients and hormones to the places that actually need them.
Your tissues and organs.
The amount of thyroid hormone in the blood is only helpful to us if we KNOW for sure that the hormone and nutrients are making it into your cells.
Most doctors check your blood levels of hormones and assume that if blood levels are “normal” your tissues must be getting the right amount of hormones.
But, obviously, that isn’t the case.
What’s more important than your blood levels of thyroid hormone is the answer to this question:
Are your tissues actually getting the right amount of thyroid hormone?
And we are somewhat limited in how we can actually test this, short of doing a biopsy at the target tissue and it certainly doesn’t make sense to biopsy muscle, heart tissue, or brain tissue to diagnose your hypothyroidism.
Instead, we can use a couple of surrogate markers to evaluate if your tissues are getting enough thyroid hormone:
- Your basal body temperature – This can give us an idea of what kind of total energy your body is producing. If your temperature is low, you may have a problem getting thyroid hormone into your cells. You can read more about how to test your basal body temperature and how to follow this value while taking thyroid medication here.
- Sex hormone binding globulin levels – Read above for more information. This will give us an idea if your Liver tissue is getting enough thyroid hormone.
- Your subjective symptoms! Symptoms come from a tissue-level deficiency of thyroid hormone and if you still have symptoms despite being on thyroid medication, you might not be getting enough hormone inside your cells.
- The relaxation phase of Deep Tendon Reflexes – One of the most sensitive tests to look at is the relaxation phase of deep tendon reflexes (5). This can actually be tested using sophisticated devices to give an exact number.
If you focus completely on serum levels of thyroid hormone you are going to miss hypothyroidism at the tissue level (6).
This may not be an issue for EVERY patient but it will certainly be a problem for many patients – especially those with “normal” thyroid levels but almost every hypothyroid symptom in the book.
#3. Other hormones influence the action of Thyroid hormone
If you want to treat your thyroid properly you can’t look at each organ system in isolation.
Your body is like a spider web.
When you pull one string, does the entire spider web magically stand still?
No!
The same thing is true in your body when a hormone system is out of balance.
The other hormonal systems will eventually crash after trying to “stabilize” the problem as much as possible.
It’s like limping on your left leg after you hurt your right leg. After 10 days of favoring your left leg, both of your legs are eventually going to start hurting!
In the case of your thyroid, the two most common hormonal imbalances that can impact and worsen thyroid function include:
- Adrenals and Cortisol Levels
- Estrogen balance with Progesterone
Cortisol and Adrenal Fatigue
Your adrenals and thyroid function are intricately linked (7).
Changes in your TSH cause changes in your cortisol and vice versa.
And this can be a good thing in the short term, but after prolonged elevation, you may eventually start to experience the symptoms of Adrenal Fatigue.
Adrenal Fatigue is a condition in which you have put excess strain on your body and compromised its ability to produce stress hormones.

If you try to evaluate thyroid function without taking into account Cortisol and adrenal function, you are making a huge mistake.
Not treating associated adrenal-related issues is one of the main reasons that patients fail to improve after starting thyroid hormone.
Do NOT neglect your adrenals!
You can address adrenal function by focusing on several key areas:
- Attempting to reduce or eliminate the primary sources of stress in your life.
- Practice stress-relieving techniques such as meditation (8).
- Take adrenal adaptogens or other adrenal supplements designed to improve your stress response.
- Evaluate and test your serum cortisol levels (you can also test salivary cortisol as well).
Estrogen Dominance and Low Progesterone
Thyroid hormone, specifically T3, helps your body produce Progesterone (9).
When you have low thyroid hormone, you may also experience low progesterone levels which can lead to an imbalance known as Estrogen Dominance.
This imbalance helps explain why many women with hypothyroidism may experience irregular menstrual cycles, decreased libido, and infertility.
Don’t neglect other hormone systems when evaluating your thyroid!
#4. If you have Leptin Resistance or High Reverse T3 Levels TSH can’t be Trusted
Inflammatory states and leptin resistance cause chaos to the entire thyroid system (10).
Leptin resistance, a condition characterized by increased cellular resistance to the hormone leptin, may cause a reduction in thyroid hormone production (11).
Conditions that cause leptin resistance may lead to weight gain (and weight loss resistance), changes to your appetite, and a reduction in thyroid conversion.
Through these mechanisms, leptin resistance may also contribute to an increase in the reverse T3 metabolite.
As reverse T3 levels rise, your body will have a hard time utilizing free and active hormones effectively.
They are, in a sense, blocked from entering the cells, and because of this, they may stay floating around in the bloodstream.
This can lead to so-called “normal” blood levels of thyroid hormone which can actually drive down the TSH tricking you into thinking that your lab tests are completely “normal” when, in reality, your cells are starving for thyroid hormone.
If you have inflammation or Leptin resistance, the TSH cannot be used as the only lab test to evaluate your thyroid.
As a result, you will need to ensure that you order a complete thyroid lab panel and aim for optimal lab values.
#5. Don’t practice “Reference Range Endocrinology”
Reference range endocrinology is a term given to the art of practicing hormone management based solely on lab results.
Many physicians, and patients, tend to approach hormone management in this way.
This type of practice is flawed for several reasons:
#1. There is no evidence to suggest that each person requires the same amount of hormones.
The exact opposite is true:
After all, do we all look the same? Do we all react to medications and supplements in the same way? Do we all have the same genetics?
Why would we all require the same amount of hormones?
#2. The standard reference range is too wide and doesn’t take into account the age or medical health of the patient.
When you are comparing yourself to some “standard”, don’t you want that standard to be age-matched and healthy when compared to yourself?
Or would you rather compare yourself to someone who is 30 years your senior with multiple medical problems?
The answer is obvious:
When evaluating your hormones, you should aim to compare yourself to a young and healthy version of yourself.
The problem with standard reference ranges is that they do not take these variables into account and instead create ranges based on people of various ages and health statuses.
Lastly, the ‘standard reference range’ contains a wide range of ‘normal’ making it difficult to discern between ‘optimal for your age’ and ‘normal’.
Consider this example:
If you order a hormone test and your result comes back in the bottom 5% of the ‘normal reference range’ you would be considered normal even though there is massive room for improvement.
And that is a huge problem.
There is a big difference between being “normal” and being “optimal”.
There’s also a huge difference in what being “optimal” means between different individuals!
There will always be people that feel better at lower levels of thyroid hormone, but there are just as many (if not more) that NEED higher levels of the hormone to function at 100%!
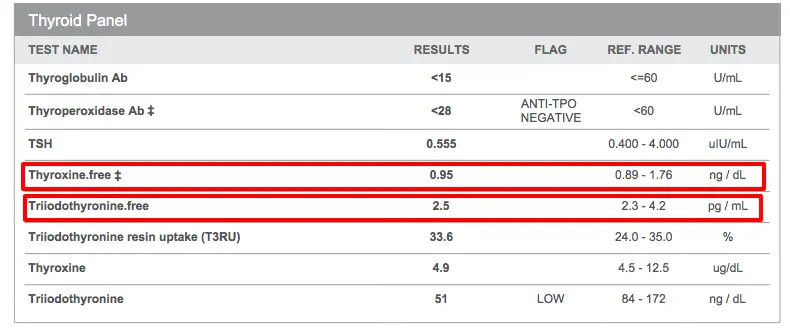
Above is a classic example of a patient suffering from Hypothyroidism with “normal” lab results, even though her labs are barely within the “normal” range.
You can see that the Thyroxine free (A.K.A. Free T4) is a result of 0.95 and the range varies from 0.89 to 1.76 ng/dL.
While the 0.95 result is very close to being abnormal it is technically still within that broad range and, as a result, many physicians may opt against treatment.
Unfortunately, most Doctors (including Endocrinologists) practice this way!
If you want to find a Doctor who doesn’t you will typically have to look outside of the traditional model.
#6. Failure to Diagnose and Appreciate Nutrients Required for Thyroid Function
It’s silly but outside of the hospital doctors don’t appreciate the value of nutrients and supplements in treating disease.
Inside the hospital, your Doctor is intimately familiar with something as simple as magnesium: it serves to help stop pre-term labor (13) and it can even bring your heart back into a stable rhythm when given intravenously (14).
Outside of the hospital, however, it’s another story entirely!
The truth is your thyroid needs several different nutrients (that are commonly depleted in most people) to function at 100%.
Some of the most common include:
- Iron – To check the iron status you’ll need to obtain ferritin (15), serum iron, and TIBC. Iron deficiency results in decreased thyroid function.
- Zinc – This nutrient helps T4 to T3 conversion (16) and acts as an anti-inflammatory agent, and may help improve your immune system. A deficiency in zinc leads to a hypothyroid-like syndrome which is ameliorated with zinc supplementation. The best way to determine if you are zinc deficient is with a trial of zinc supplementation.
- Selenium – This nutrient also helps with T4 to T3 conversion, may help decrease autoimmunity (17) and antibody levels in Hashimoto’s, and is required for thyroid hormone production.
- B Vitamins including B2 and B6 – Activated B vitamins are required for thyroid hormone production and the production of adrenal hormones. Stress and other lifestyle factors can increase the demand of B Vitamins and may lead to a deficiency.
- Vitamin D – Low levels are associated with an increased risk (18) of autoimmune disease and may also contribute to fatigue (19).
- And many more which you can read about here.
If your “thyroid” labs look normal, but you still aren’t feeling great make sure to check out these common nutrient deficiencies which may also play a role.
#7. Not appreciating the effects that Endocrine Disrupting Chemicals have on Thyroid Function
Endocrine-disrupting chemicals have been shown to reduce T4 to T3 conversion, and lower T3 levels in the serum all while NOT affecting the TSH (20).
Nowadays, detox really needs to be part of your treatment regimen.
At the very least you should actively be avoiding these chemicals that may potentially cause thyroid problems.
I would go a step further and recommend that you not only actively avoid these chemicals, but that you also try to eliminate them from your body!
You can do this by following some very simple steps:
- Drinking from filtered water only
- Avoid plastics of any kind – especially avoid microwaving your food in plastics!
- Eat organic, hormone-free foods
- Drink out of glass containers, and store your food in glass containers
- You can find more tips on how to eliminate and detox here.
Conclusion & What to do next
If, after reading this, you believe you may not be getting the appropriate treatment I would recommend you seek out a Functional Medicine Trained practitioner for further assistance.
When it comes to thyroid health, I would generally recommend that you find someone skilled at both prescribing thyroid medication and someone that is knowledgeable in treating the thyroid naturally.
Your goal, whenever possible, should be to get off and stay off of prescription medication – but realize that isn’t always the case.
And some patients may feel significantly better with the right medication to get the ball rolling.
I’ve created a resource here that you can use to find a doctor if you are struggling with your current medical plan.
Now I want to hear from you:
Do you feel like you’ve been properly diagnosed and treated?
Are you experiencing hypothyroid symptoms despite having “normal” lab tests?
What information do you have to share with others who are in the same position as you?
Leave your comments or questions below!
Scientific References
#1. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5422478/
#2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4401150/
#3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5763098/
#4. https://www.ncbi.nlm.nih.gov/pubmed/16131331
#5. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC2492977/
#6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3169863/
#7. http://www.ncbi.nlm.nih.gov/pmc/articles/PMC3520819/
#8. https://www.ncbi.nlm.nih.gov/pubmed/25995404
#9. http://www.ncbi.nlm.nih.gov/pubmed/9846161
#10. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4802023/
#11. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC377492/
#12. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2605414/
#13. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5690360/
#14. https://www.ncbi.nlm.nih.gov/pubmed/11105328
#15. http://www.ncbi.nlm.nih.gov/pubmed/16500878
#16. http://www.ncbi.nlm.nih.gov/pubmed/8157857
#17. http://www.ncbi.nlm.nih.gov/pubmed/23046013
#18. http://www.ncbi.nlm.nih.gov/pubmed/17699936
#19. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4158648/
#20. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5751186/








