Are you undergoing thyroid treatment but not getting better?
Do you have ALL of the symptoms of hypothyroidism but normal “thyroid labs”?
Is T4 making your symptoms WORSE or are you gaining weight while taking this medication?
If so, hypothalamic obesity disorder may be the underlying cause of your symptoms.
This condition mimics hypothyroid-like symptoms but the treatment is completely different, and what’s worse is that thyroid treatment may make this condition worse.
What is Hypothalamic Obesity Disorder?
New research has shed light on yet another reason that not only causes weight gain but also makes weight loss almost impossible if not treated.
The condition is known as hypothalamic obesity disorder (1).
But what is it?
This condition is unrelated to your thyroid, but it tends to present with the exact same symptoms as hypothyroidism leading patients to believe that they have hypothyroidism when they really don’t.
Why?
Because they have EVERY symptom of hypothyroidism but they have “normal” labs.
This leads them to believe it MUST be a thyroid problem so they bounce around from Doctor to Doctor until they can get treatment.
The main problem is that patients with this condition also tend to be unresponsive to thyroid treatment – meaning their symptoms do NOT go away with proper thyroid treatment.
What’s worse is that taking thyroid medication, if you have this condition, may make your weight gain worse.
This is true even when taking NDT and/or T3-containing medications like Cytomel.
Because of this, it’s really important to understand what this condition is and how to actually treat it…
Your hypothalamus helps control several important factors as it relates to your current weight including your basal body temperature, your resting metabolic rate, how much heat you produce, your appetite, and finally your daily rhythms.
The hypothalamus is normally supposed to “sense” through hormones like leptin when the body has extra fat.
Signals are then sent to your fat cells to increase fat oxidation, burn extra fat and increase your metabolism to keep normal homeostasis and reduce body weight.
With hypothalamic obesity disorder, this regulatory process becomes dysregulated.
Essentially your neurological system and hypothalamus do not sense the normal regulatory factors and they wrongly assume that your body is in a state of starvation.
This results in changes in the hypothalamus which slows down your metabolism, increases your appetite, lowers your body temperature, reduces heat production and energy production, and causes the body to constantly store calories as fat – even in the presence of calorie restriction.
This condition is well known by obesity Doctors but it’s usually only a problem after severe trauma to the brain.
Newer studies now indicate that this condition can be caused by other environmental and lifestyle factors – meaning you don’t need some sort of trauma to cause the condition.
So what causes hypothalamic obesity disorder?
We don’t have all of the answers, but the following behaviors tend to increase your risk of developing this condition:
- Recurrent yo-yo dieting and calorie-restricted diets
- Untreated hypothyroidism
- Binge eating or eating disorders
- Leptin resistance
- Chronic stress
- Constant and persistent lack of sleep
As research continues we will likely have a better understanding of this condition and what causes it, but for now, it’s best to completely AVOID these behaviors if at all possible.
If you have the risk factors listed above AND you also haven’t felt better while taking thyroid medication, then hypothalamic obesity disorder should be considered.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Symptoms of Hypothalamic Obesity Disorder
While I’ve suspected that this condition is much more common than most physicians think it is, there hasn’t been any research to confirm how common it actually is.
Recently, however, researchers tested the prevalence of hypothalamic obesity disorder (2)…
To do this they studied 50 people who presented with typical “hypothyroid” like symptoms.
Some patients were previously treated with thyroid medication to “optimal” blood levels but still remained symptomatic.
The researchers then deemed hypothalamic dysfunction was “likely” if patients exhibited three or more symptoms (listed below) and “definite” if they had four or more symptoms.
The most common symptoms of hypothalamic obesity disorder include:
- Fatigue (76%)
- Temperature dysregulation (68%)
- Weight change (88%) –> constant weight gain despite changing your diet and exercising and/or inability to lose weight
- Changes in sleep (70%)
- Pain (72%)
- Mood disorders 80%)
- Libido issues (38%)
- Sympathetic or parasympathetic complaints (74%) –> dizziness, lightheadedness, inability to exercise, etc.
Of these 50 patients 68% were determined to have hypothalamic dysfunction (meaning they had 4+ symptoms) and 22% were considered to “likely” have hypothalamic dysfunction (meaning they had 3 symptoms).
That totals 90% of patients referred to this study! Making this condition far more common than previously thought.
The problem with these numbers is that MOST of the patients who fall into this category tend to be labeled by the medical community as those who try to “game” the system (malingering), or those who have mood disorders (borderline personality disorder/depression/anxiety, etc.).
When in reality these patients have a real condition that is poorly understood by physicians and the medical community in general.
This makes it VERY important for you to have an understanding of this condition and understand the symptoms so you can advocate for yourself if necessary.
Fortunately, the diagnosis of this condition is very easy:
This study supports the idea that hypothalamic obesity disorder can be easily diagnosed clinically (meaning based on symptoms) and is the MOST common in patients who present with the typical hypothyroid symptoms but do NOT improve with thyroid hormone replacement.
How to diagnose hypothalamic obesity disorder:
- Hypothalamic obesity disorder is present if you have 4+ of the symptoms listed above (which has implications for your treatment)
- Hypothalamic obesity disorder is VERY likely if you have 3 symptoms (listed above)
- Hypothalamic obesity is likely to present if your hypothyroid symptoms do NOT improve after taking thyroid medication
Treatments for Hypothalamic Obesity Disorder
While knowing you have this condition IS important, it’s really just the beginning.
You will NEED to get the proper treatment.
Because of the reasons discussed above (and the fact that most physicians don’t understand this condition), you may have difficulty getting the proper treatment from your primary care physician or endocrinologist.
In addition, the treatments for this condition are less conventional than traditional “weight loss” therapies which means your physician will need to read up on newer medications and studies to understand the treatment.
The presence of hypothalamic obesity disorder usually indicates that significant damage has been done to your metabolic and hormone systems over time.

This means that you will likely have to be aggressive in terms of treatment.
Many of the treatments for this condition will require a physician, and for best results, I recommend layering these therapies on top of each other.
You can learn more about the various treatments for hypothalamic obesity disorder below:
#1. Injectable diabetes medications
I’ve discussed the value of these medications in previous posts, but it’s worth spending some time here as well.
The injectable medications I am referring to here directly help to lower both insulin and leptin – both hormones which tend to be dysregulated in hypothalamic obesity disorder.
In addition, they also help in the following ways:
- By reducing appetite
- By increasing beta cell proliferation
- By reducing insulin resistance
- By reducing gastric emptying and reducing sugar cravings
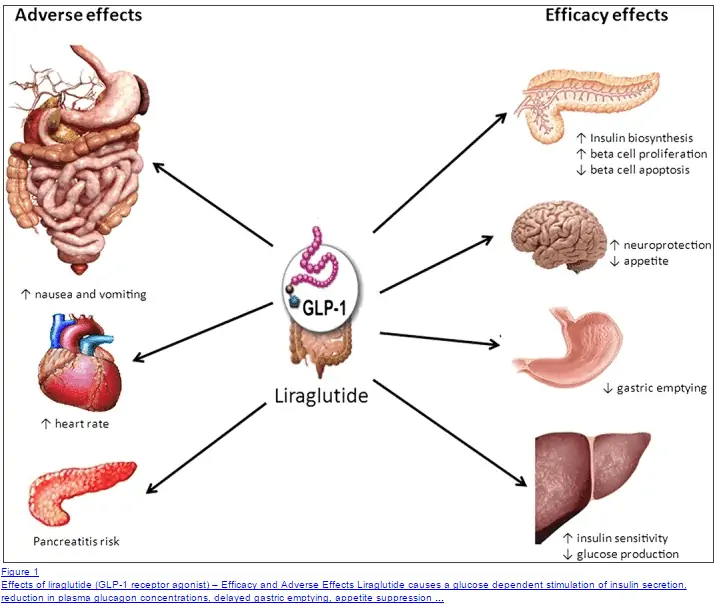
These medications have been shown in multiple studies to directly help with weight loss (even if used in non-diabetic patients).
The problem with using them is that they are currently only FDA-approved for the treatment of type II diabetes and not for hypothalamic obesity disorder.
For this reason, it can be difficult to get your Doctor to prescribe them for you and for insurance to cover the medication.
In my weight loss guide, I discuss how to use these medications, how to titrate them correctly, and how to get them for the best possible price.
As an example of how effective this medication can be I’ve included an image below:
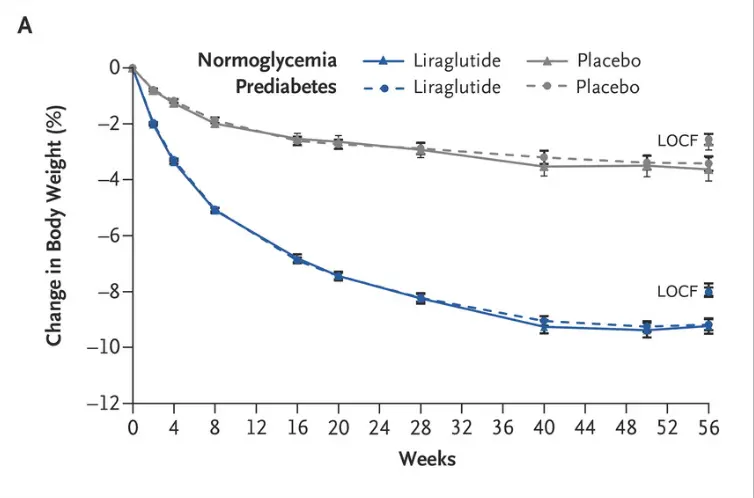
This graph represents a study that showed that people taking Saxenda lost almost 10% of their body weight (3) over several months.
Before you use this medication remember this:
These medications will NOT work unless they are coupled with other therapies.
#2. Low dose naltrexone +/- Wellbutrin
Remember that hypothalamic obesity disorder is a problem in your brain.
That means you need medications (and therapies) designed to balance your brain to help normalize your appetite and hormones.
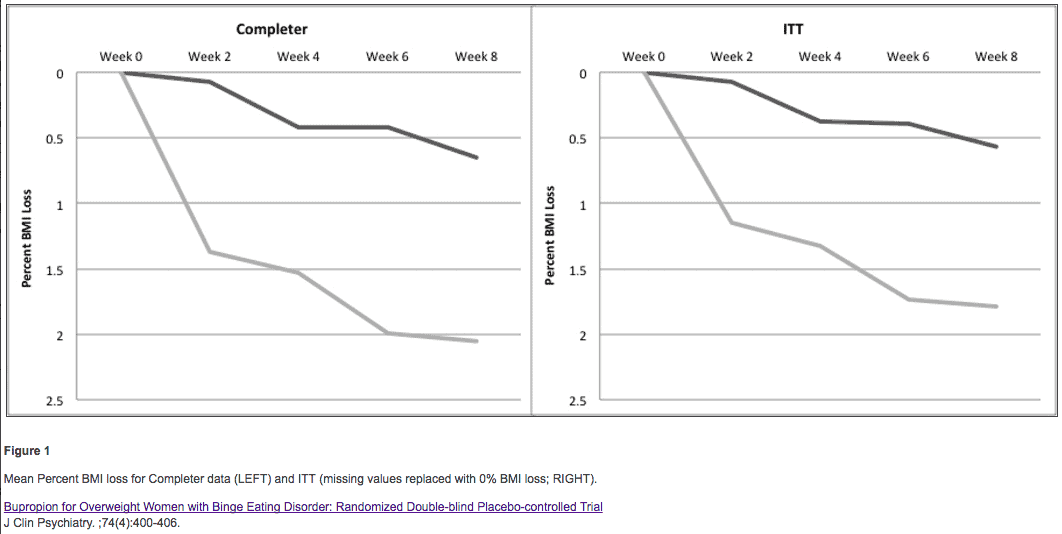
Buproprion and Wellbutrin do just this.
The combination of these medications is known as Contrave (which I’ve discussed previously), but they can be used by themselves or in conjunction with one another to help treat hypothalamic obesity disorder.
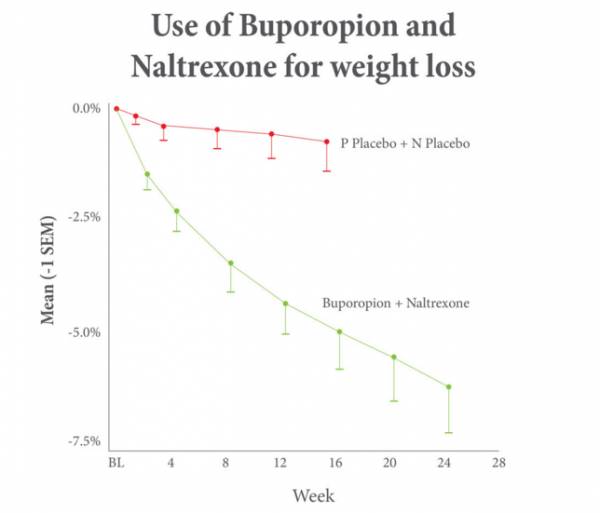
These medications work by modulating neurotransmitter levels and by normalizing both your appetite and metabolism.
I’ve discussed the benefits of using LDN for autoimmune disease and inflammation in previous posts, but it also helps directly reduce weight loss.
Wellbutrin, on the other hand, has been shown in studies to help modulate appetite and reduce both cravings and binge eating (4).
#3. Mediterranean style diet
People tend to get this one wrong frequently:
While diet is important if you are trying to lose weight it is NOT the most important factor.
You have to realize that there is no “perfect” diet that will magically make you lose weight.
Instead, you need to consider that your diet should be adapted to your current situation.
This means that you need to manage your macromolecule ratios and the type and quality of your food depending on what is going on in your body.
When it comes to hypothalamic obesity disorder the best diet tends to be a Mediterranean-style diet.
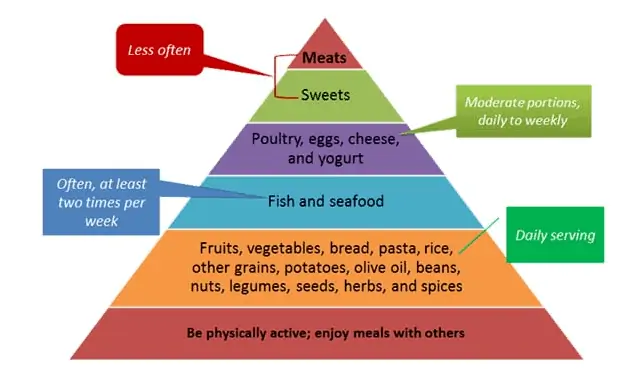
This diet is naturally high in fruits, vegetables, fish, and healthy carbohydrates – which might be confusing to many people.
Another important factor is that it is low in meats and proteins in general.
This style of diet (including macromolecule ratios) tends to work better for people with leptin resistance and can actually lead to weight loss in these individuals.
The Mediterranean diet has also been shown to help with weight loss by itself (5) (but again, it should be coupled with other therapies).
#4. Anti-depressants (see Wellbutrin above)
I’m generally not a fan of using anti-depressants unless they are absolutely necessary and hypothalamic obesity disorder is one of those situations.
One of the big problems with this disorder is that it takes over your appetite and your cravings which can make sticking to a healthy diet very difficult.
Using certain anti-depressants (specifically Wellbutrin) can help “normalize” these cravings.
This allows you to match your caloric intake to your appetite.
Without this medication, your brain might be telling your body to constantly eat more than you should which may result in excessive caloric consumption and therefore weight gain over time.
Taking Wellbutrin has been shown to normalize your caloric intake, reduce cravings, reduce binge eating, and therefore help with weight loss.
#5. HCG
I need to be clear:
I am NOT talking about the HCG diet, but instead, I am talking about using the hormone HCG to boost weight loss.
The HCG diet is a harmful diet that ultimately results in the very condition of hypothalamic obesity disorder.
I see patients all the time who present with high reverse T3 levels, damaged thyroid function and a damaged metabolism as a result of the HCG diet:

But you need to realize that this damage occurs because of the DIET component and NOT the HCG injections.
HCG by itself (if used as a hormone) can enhance weight loss results if used with a healthy diet.
HCG has been shown to improve thyroid function by increasing T3 levels and helps regulate sex hormones like estrogen and progesterone.
HCG is a powerful tool to help with weight loss but it MUST be used correctly and in the right setting and with the right type of diet.
I discuss how to use HCG effectively for long-lasting weight loss in my weight loss guide.
#6. Phentermine
Phentermine is another medication that is misused by most people.
Most physicians and patients use phentermine to suppress appetite and cause temporary weight loss that always comes back after they stop the medication.
But you can use phentermine in unique ways to help with long-lasting weight loss.
Phentermine can be useful in reducing sugar cravings and appetite and can be combined with HCG to enhance weight loss, but it must be used episodically and periodically.
#7. Daily Exercise to Tolerance
Exercising should ALWAYS be a part of a weight loss program, but it is especially important in hypothalamic obesity disorder.
Patients with this condition tend to have debilitating fatigue, but they still must exercise in order to lose weight and paradoxically increase their energy.
Exercising to tolerance means that you exercise to whatever your current limit is.
I recommend using a combination of low-intensity exercise with resistance training.
#8. Thyroid Treatment with T3 (May be temporary)
I mentioned previously that patients with hypothalamic obesity disorder tend to do worse with thyroid medication but that isn’t the whole truth.
Usually, these patients tend to not tolerate T4-only medications very well, but they often do need some element of T3 medication in order to improve long term.
While T3-containing medications can be helpful (medications like Cytomel, WP thyroid, Armour thyroid, etc.) they won’t completely reverse the condition by themselves.
It may also be necessary to temporarily use supraphysiologic doses of T3 medications to help “flush” the system, especially in the presence of thyroid resistance and high levels of reverse T3.
It’s important to realize that this condition is NOT primarily a thyroid problem, but that thyroid medication needs to be part of the solution.
This concept can be confusing for patients because the systems mimic hypothyroidism exactly.
Instead of laser focusing on your thyroid make sure you focus on all of the other treatments and aspects listed above.
Back to you
Over time I think we will find that hypothalamic obesity disorder is much more common than we previously thought.
While this condition can be very difficult to treat it is not impossible to treat.
But it does require a comprehensive treatment plan with multiple therapies.
Most of these therapies are unconventional and may require an open-minded physician to get them all.
Bottom line?
Don’t give up! There is hope for weight loss even in the most difficult patients.
I’ve successfully been able to help patients with this condition lose weight and feel better, but it does take time (sometimes 9+ months of consistent therapy).
But now I want to hear from you:
Do you think you are suffering from hypothalamic obesity disorder?
Are your thyroid labs “normal” on thyroid medication and yet you still have symptoms?
Do you have questions about the treatment?
Leave your questions and comments below!








