If you have Hashimoto’s or hypothyroidism and feel like losing weight is impossible, then this patient case study should give you some hope.
The following is a walk-through of a Hashimoto’s weight loss success story in a patient who was able to lose over 50 pounds throughout a period of about 6 months.
I know losing weight can be difficult (or feel impossible) if you have a thyroid problem.
But the truth is, as long as you take the right approach, you will see results.
It’s not uncommon for me to receive emails like these:
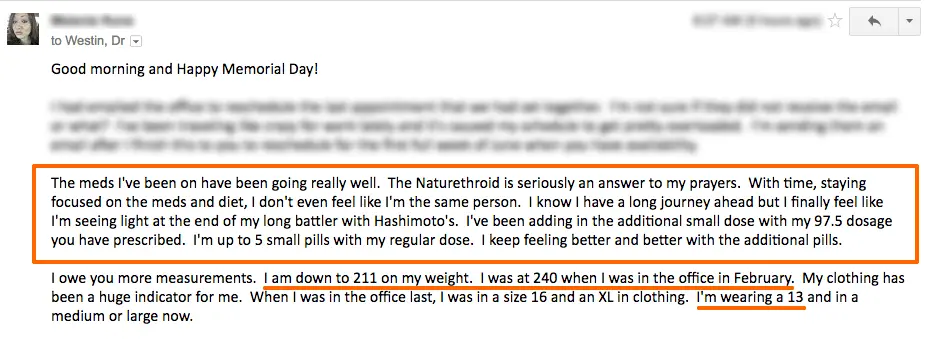
But for many patients out there suffering and looking for help from standard doctors or endocrinologists, it can feel like you are smashing your head against the wall and the one winning is the wall.
Unfortunately, the most effective therapies (including the ones that we are going to be discussing soon) are not the type of treatments you will get from these types of doctors.
That doesn’t mean they aren’t effective or won’t help. In fact, it’s the opposite.
But in order to get them, you may have to spend some time and energy looking for the right type of doctor (more on that below).
With all this in mind, let’s talk about what it takes to lose 50+ pounds, drop over 40 inches, and reduce Hashimoto’s symptoms by almost 100%.
Before we do, you can take a look at the before and after pictures of this patient below:
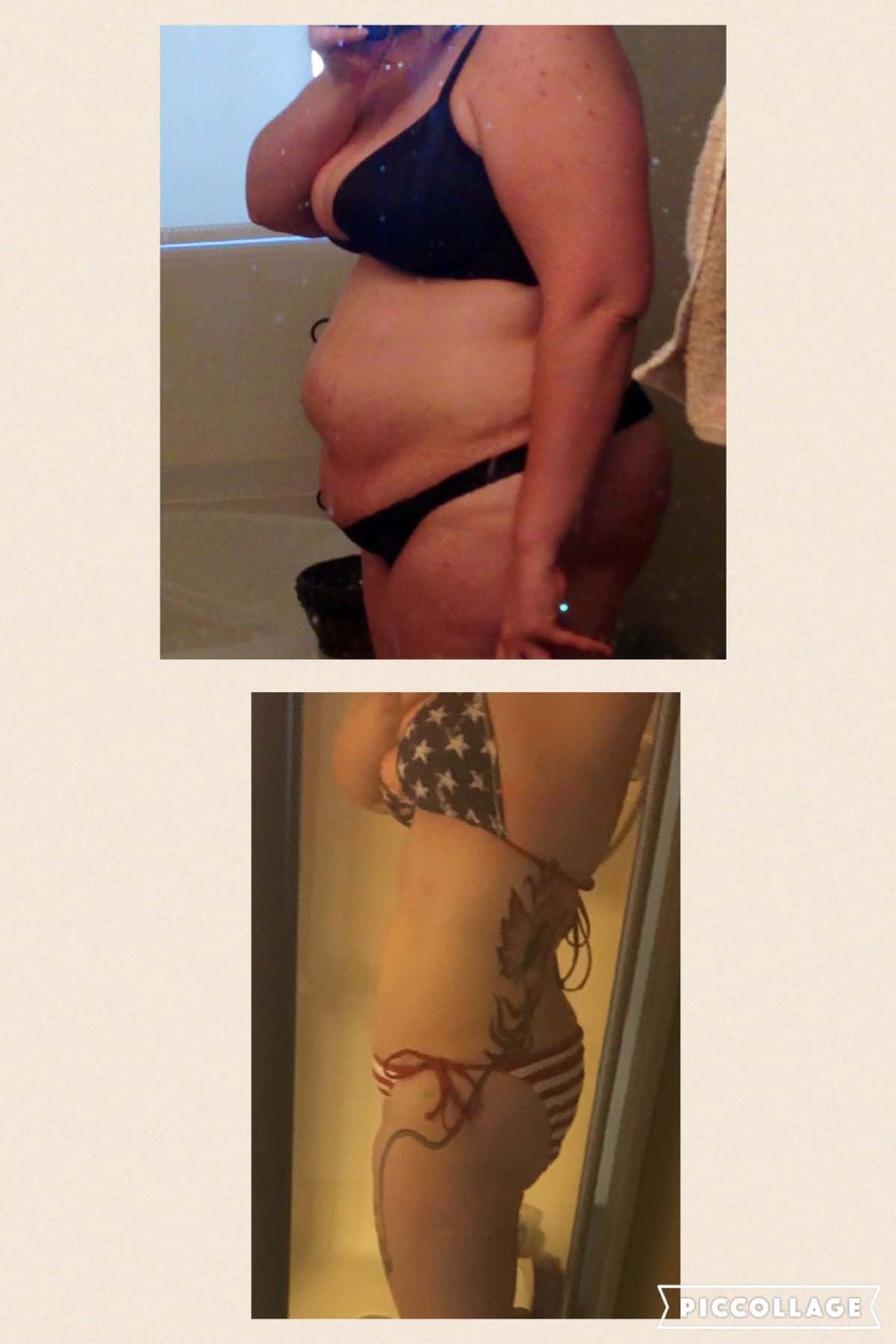

Hashimoto’s Weight Loss Case Study
Here’s what you need to know about her:
This patient has a family history of thyroid problems (all of which were undertreated or misdiagnosed), and ever since she was a child she had issues with weight, fatigue, and decreased energy.
At an early age, she underwent radioactive iodine ablation, but 30% of her thyroid remained functional as estimated by her doctors at that time.
As a result of the ablation and her almost normal thyroid lab values, she was placed on a low dose of levothyroxine and felt terrible for about 20 years.
Over this time period, she gained weight and never saw symptomatic improvement despite taking levothyroxine faithfully so she eventually stopped taking her thyroid medication altogether.
This was not a good idea (as we will soon discuss) because she was operating with only about 30% function from her thyroid gland.
In other words, the 30% of her remaining thyroid gland was trying to keep up with the permanently damaged 70% which led to all of these problems.
She was kicked around from doctor to doctor until she was at her highest weight of 270 pounds.
Not satisfied with this result, and like a true champion, she took matters into her own hands and was able to lose 30 pounds by changing her diet and adding in exercise despite feeling exhausted 24/7.
She was able to do this with a keto-type diet but eventually hit a plateau and was unable to lose any further weight around 250 pounds.
Even though she was able to lose some weight, she still felt symptomatic from her thyroid and her symptoms remained (remember she was not on thyroid medication during this time).
Optimal vs Normal Thyroid Lab Tests: Why she was undertreated for years
The most interesting part of her story is that she was only ever treated with a low dose of levothyroxine despite seeking care from multiple endocrinologists and primary care physicians.
She was always told her lab tests were “normal” but after her insistence of stating she didn’t feel normal, she was finally given some thyroid medication even though it didn’t make a difference.
And this is where things get very interesting.
One of the primary reasons that she was never treated correctly is because her doctors were most likely using the “standard” reference range for determining if her thyroid was functioning optimally.
What they were failing to appreciate was her body’s remarkable ability to maintain serum levels of thyroid hormone despite missing 70% of her thyroid gland because they were focusing on standard reference ranges and not optimal reference ranges.
When you take a closer look at her thyroid lab tests, you can see some obvious issues:
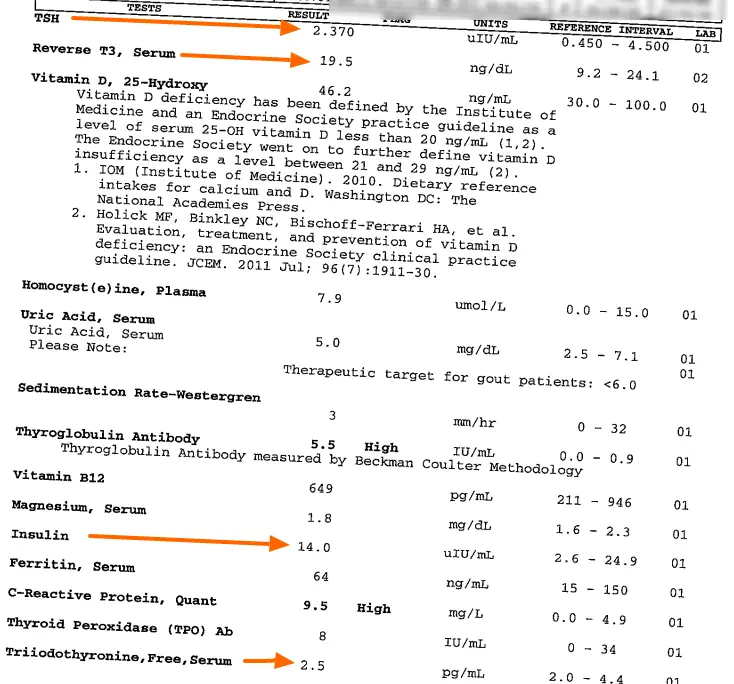

As you can see the majority of her lab tests do fall within the “normal” range with the exception of her CRP and thyroglobulin antibody levels.
But let’s go over the rest of the labs to help you understand the difference between “optimal” and “normal” and why she had great results when we finally interpreted these lab results correctly.
Her list of abnormal lab results includes:
- Suboptimal TSH: When not on thyroid medication optimal TSH levels should be < 2. This range is based both on anecdotal evidence as well as some newer studies (you can read more about why TSH levels can be inaccurate here).
- High Reverse T3: Indicating poor thyroid conversion. Reverse T3 should generally be < 15 for optimal thyroid function.
- Elevated thyroglobulin antibodies: Indicating a component of autoimmune thyroiditis contributing to poor thyroid function. You can read more about how to lower antibody levels here.
- High fasting insulin: Fasting insulin should be < 5. High levels contribute to weight gain and weight loss resistance and may make reverse T3 levels higher.
- Elevated CRP: Indicating inflammation is present in the body, optimal levels should be as low as possible.
- High serum leptin levels: High levels make TSH less accurate and promote high reverse T3 levels and also contribute to weight loss resistance.
Compare this evaluation to the previous notion that she was completely “normal”.
Does she sounds or look “normal” to you?
Definitely not, and you may find yourself in this same situation.
Using these functional and optimal reference ranges, it’s easy to see that she is in fact NOT normal and that she has multiple hormone abnormalities contributing to both her thyroid symptoms and inability to lose a significant amount of weight despite eating a healthy diet.
So what is happening in her body and how does this explain her symptoms?
It’s hard to know for sure but based on what we are seeing here the likely answer is tissue-level hypothyroidism.
Tissue level hypothyroidism refers to a state where there can be adequate thyroid hormone in the body and bloodstream but that thyroid hormone is not responsive at the cellular level.
It’s also sometimes referred to as thyroid resistance (although this would be a form of acquired thyroid resistance and not a genetic version of thyroid resistance).
In this specific situation, thyroid medication was definitely the answer.
We know that based on her labs and her history of radioactive iodine ablation.
Even though she had some remaining thyroid function (approximately 30%) that tissue was not able to keep up with the demands of her body.
As a result, she experienced hypothyroid symptoms as well as weight gain.
Putting her on thyroid medication was definitely the answer but, unfortunately, her doctors used a low dose of the wrong type of thyroid medication.
Because her body had a hard time converting the T4 from levothyroxine into T3, she was never really able to meet the demand of her tissues or resolve her hypothyroid symptoms.
This persistent hypothyroid state then set the stage for her to develop other issues such as leptin resistance and insulin resistance as seen in her lab tests.
In a vicious cycle, these hormone imbalances then made her thyroid conversion worse and contributed to her high reverse T3 levels.
This scenario is bad by itself but it doesn’t stop there.
We also know that she has Hashimoto’s thyroiditis (she was diagnosed with this a long time ago) and even though she was placed on levothyroxine to try and treat her hypothyroidism, the underlying cause of her Hashimoto’s was never addressed.
We would then expect that over time she would see more damage to the remaining 30% of her thyroid gland tissue due to inflammation and destruction from her own immune system (the hallmark of Hashimoto’s).
This adds fuel to the fire mentioned above.
Ultimately, after years of struggling, she presented with these lab results which are what you are seeing now.
One final point worth mentioning is how reverse T3 impacts the function of thyroid hormone.
When we discuss serum levels of thyroid hormone we are more concerned about how much thyroid hormone is getting into the cells and not necessarily how much thyroid hormone is floating around in the serum.
“Normal” levels of thyroid in the blood do NOT mean that the tissues are getting enough thyroid hormone and this was certainly the case in this patient.
Her serum levels of free T3 and free T4 remained relatively preserved but she remained quite symptomatic despite this.
For this reason, the most sensitive measure of thyroid function in this patient is the relationship between free T3 and reverse T3, otherwise known as the free t3 to reverse T3 ratio.
And this patient is just screaming that she is hypothyroid with a ratio of 0.128!
The secret to diagnosing and treating many hypothyroid patients is this ratio because it will identify most hypothyroid patients when all other lab tests are “normal”.
This ratio can be helpful in cases of “normal” thyroid lab tests because it starts to become abnormal before any other thyroid lab tests make it outside of the normal reference range.
Treatment Plan + How to Approach a patient like this
The most important part of this patient’s evaluation is her management.
What I mean is how she was treated.
We can wax philosophical about her history, what is going on in her body, how she got there, and so on, for a long time.
But that doesn’t do us any good if we don’t fix it!
Many patients believe that if they can get all the “right” tests that their doctor will finally treat them appropriately or change their medication or increase their dose.
This rarely happens.
If your doctor isn’t willing to order the right thyroid blood tests then it likely means they don’t really know their purpose or how to interpret them.
And when it comes to getting results like this patient you really need to find someone who is willing to not only order and interpret the right tests but also provide appropriate treatment.
This means you need a thyroid-literate doctor.
If you are struggling to find one, you can use this resource to help.
So how do you approach a patient like this with multiple problems who is severely undertreated?
You have to take a comprehensive approach that includes treating the following areas:
- Hormones and prescription medications
- Supplements and botanicals
- Inflammation and autoimmunity
- Detoxification
- Diet and exercise (lifestyle factors)
- Stress Reduction
If these areas are not all addressed at some point then you’re not really treating the problem.
And this is a REALLY important point:
Make sure you don’t get what I call “thyroid tunnel vision”.
This is the idea that every problem that exists in your body is related to your thyroid and the solution is to simply change/increase/swap thyroid medication until you see a resolution.
Patients tend to fall into this category especially when they have extra weight to lose.
They wrongly assume that increasing their thyroid medication will result in significant weight loss.
At most changing or adding in thyroid medication will result in an average 5-10 pound weight loss.
If you are like many hypothyroid patients then you probably have more weight to lose than just an extra 5-10 pounds.
But I can assure you that the extra weight is almost always related to other factors.
Let me use this patient as an example to help illustrate this point:
Over a 9-month period of time, this patient experienced the weight loss you are seeing here as well as almost complete resolution in her low thyroid symptoms.
But what is interesting is that her hypothyroid symptoms were almost completely gone within the first 3 months of her treatment, but she only lost 20ish pounds or so during that time.
The remainder of her weight loss came in months 3 through 9 and without changing her thyroid medication.
She was able to lose this weight because during those months we focused on the other hormone imbalances that were a result of decades of low thyroid function but not directly due to her low thyroid state.
Yes, her initial low thyroid state set the stage for the weight gain but it wasn’t solely responsible for it which is why optimizing her dose of thyroid medication resolved her symptoms but not all of her extra weight.
In this way optimizing your thyroid medication dose is necessary to lose weight but will not cause all of the weight itself.
And this is an important distinction that you should be aware of if you are trying to lose weight.
- Bottom line: When searching for a provider to help with your Hashimoto’s/Hypothyroidism make sure your provider also understands hormone imbalances that contribute to and potentiate weight gain and weight loss resistance.
T4 vs NDT & Reverse T3
Why did this patient respond so well to Nature-throid when she didn’t respond to levothyroxine previously?
A big part of the reason has to do with conversion mechanics between T4-only medications and T4/T3 combination medications.
T4-only medications (like levothyroxine, Synthroid, and Tirosint) can work for some people but fall short in patients who have high levels of inflammation or insulin/leptin resistance.
One of the primary reasons for this is that the body converts T4 into either T3 (active thyroid hormone) or reverse T3 (inactive thyroid metabolite) and this conversion process is influenced by factors like inflammation.
If the body is in a state of inflammation then providing more T4 (in the form of thyroid medication) is like adding fuel to the fire, your body will take the T4 and turn it right into reverse T3 which blocks the action of T3.
You can bypass this problem by taking thyroid medications that contain T3 thyroid hormone.

Natural desiccated thyroid preparations contain a combination of T4 and T3 together. Each grain of Nature-throid contains approximately 38 mcg of T4 and 9 mcg of T3.
The benefit of adding T3 to T4 dosing is that the T3 can directly bypass the conversion pathway and has a direct action on the nuclear receptors of cells.
This means you don’t have to worry (*too much) about the conversion process because providing T3 thyroid hormone bypasses the necessity of thyroid conversion.
*This isn’t entirely true for everyone, though, because NDT formulations still contain more T4 than T3.
Generally speaking, the more inflammation, autoimmunity, stress, and hormone imbalances a person has the better the more likely they will need T3 thyroid medication.
Hopefully, this is making sense!
Beyond using the right type of medication, we still have to worry about the dose.
You can take the right thyroid medication but the wrong dose and not get any of the desired effects you are looking for.
This can be solved with self-titration.
Nature-throid Dosing and Self-Titration – How to Dose Your Medication
This patient was able to find her dose of Nature-throid by utilizing what is called self-titration.
If you’ve never heard of self-titration let me explain:
This is the idea of slowly but steadily increasing your dose every 10-14 days (depending on the patient) based on a combination of symptoms, lab results, and other factors (like resting heart rate/body temperature).
One major benefit of self-titration is that it allows for a slow and steady increase in thyroid hormone over weeks to months which then allows the body to adapt to thyroid hormone to minimize negative side effects that can come from using T3 medication.
While self-titrating it is a great idea to keep track of both basal body temperature and resting heart rate to help monitor the effectiveness of your thyroid dosing.
Monitoring these variables also helps to prevent accidental overdose which is something you definitely don’t want!
The patient in this case study titrated her dose up to a total of 2.5-3 grains of Nature-throid which is around 195mg.
Even though she did great on just pure Nature-throid, some patients need the additional T3 (Cytomel, liothyronine, or SR T3) along with their NDT.
As I mentioned previously, as she increased her dose many of her hypothyroid symptoms disappeared over the first 3 months or so.
Finding the Best Diet: AIP vs Nutritional Ketosis vs Other Diets
Diet is critical to treating and reversing Hashimoto’s and if used correctly it can also directly impact insulin and leptin levels.
What you need to realize, though, is that changing diet is typically not enough to normalize weight by itself.
Just like optimizing your thyroid medication, changing your diet definitely can help, but it must be accompanied by other therapies if you want to lose a significant amount of weight.
Many thyroid patients will lose some weight while trying various types of diets (usually in the range of 5-10 pounds) but this weight never stays off and they typically don’t reach whatever goal they are shooting for.
But this doesn’t mean diet isn’t important if you want to lose weight, the opposite is true.
I’ve written about the various types of diets you can use to help reduce antibodies and inflammation here which I would recommend checking out if you haven’t already.
In this particular patient, I started her on the autoimmune protocol (or AIP diet).

I generally don’t recommend this type of restrictive diet for most thyroid patients but this case is unique in that the patient had more than just one autoimmune disease (Hashimoto’s).
She also suffered from another autoimmune condition known as idiopathic thrombocytopenic purpura (1) which is also known as ITP.
As a result, I started her on the AIP diet and she did have a favorable response with a reduction of inflammation, an improvement in her platelet levels (impacted by her ITP), and a resolution in her thyroid symptoms.
While the AIP diet was effective in this case, it’s not necessary that everyone use it for Hashimoto’s or for weight loss.
Some patients wrongly believe that simply switching to the AIP diet will result in weight loss.
While the AIP may result in reduced inflammation which may improve T4 to T3 conversion, generally patients do not experience significant weight loss with dietary changes alone.
This is especially true in patients with other hormone imbalances (like this patient and probably like you if you are reading this).
Prior to working with me, she had tried the ketogenic diet with minor success.
I’ve talked about the pros and cons of the keto diet for thyroid patients here.
Using LDN for Autoimmunity and Inflammation
LDN, also known as low-dose naltrexone, is another tool that was used.
It was prescribed for several reasons:
- The fact that she had a history of multiple autoimmune diseases (both Hashimoto’s and ITP)
- Her joint pain
- Her insulin resistance
- Her high inflammatory levels
- Her issues with weight
She’s definitely a slam-dunk candidate as far as patients with Hashimoto’s go for using this off-label medication.
LDN can act as an immune modulator and help to reduce inflammation in some patients with autoimmune diseases.
It doesn’t work in every patient but I’ve found it to be particularly helpful in patients with autoimmune disease and chronic pain/chronic joint pain.
Studies have shown that LDN can be useful in various autoimmune conditions ranging from multiple sclerosis (2) to fibromyalgia (3).
In low doses, naltrexone may help to regulate immune function and balance multiple different neurotransmitters (4) which translates to symptomatic benefits in many patients.
LDN can also be used as a novel anti-inflammatory agent (5) which may help promote thyroid conversion and thyroid function overall.
In addition to all of these other benefits, naltrexone can help promote weight loss through hypothalamic changes (6) which mediate body set point and appetite triggers.
It should be fairly obvious why she was prescribed LDN because she fits just about every box you can in terms of potential benefits.
At one point during her therapy, she attempted to take herself off of the LDN and noticed a flare-up of chronic pain and joint inflammation, due to this she was placed back on the medication and has been on it since.
The Right Nutrients to Help Thyroid Function
Using the right supplements is almost always an important part of improving overall health and thyroid function.
It’s a rare situation when I look at someone and think that they wouldn’t benefit from some type of supplement.
Why?
Because supplements can be used to enhance the effectiveness of other treatments like diet, thyroid medication, exercise, and so on.
Supplements have the potential to help curb cravings (like protein powder) to keep you from eating unhealthy foods.
They can help you slow down inflammation by providing a direct source of omega-3 fatty acids (like fish oil).
They can provide you with energy which can help you exercise more regularly.
And so on and so on.
Supplements have huge benefits as long as they are used correctly.
They are also important for thyroid function.
Here’s why:
Over 13 nutrients are required for proper thyroid production, conversion, and cellular activation (you can read about all of them here).
And if you aren’t eating real whole foods most of the time, there’s a good chance that you don’t enough of all of these vitamins and nutrients.
In this specific case, this patient needed and did well on the following supplements (she has been on various supplements through the 9 months of treatment but these have remained consistent):
- Vitamin B12 injections – For vitamin B12 deficiency (learn more about why B12 shots are better for patients with Hypothyroidism and Hashimoto’s here).
- Zinc + selenium – Zinc and selenium act to lower inflammation, balance immune regulation, and promote T4 to T3 conversion (helpful in patients with high reverse T3).
- Adrenal support – Cortisol dysregulation is common among patients with hypothyroidism and adrenal function should be treated along with thyroid hormone replacement.
- Probiotics – Decreased motility of the GI tract is common among hypothyroid patients due to thyroid action on peristalsis, GI dysfunction should be a cornerstone of treatment.
- Liquid Vitamin D + K2 drops – To replace low Vitamin D and to promote immune function. They can be used with or without vitamin K2.
Detoxing Endocrine Disrupting Chemicals
Another key to her success was spending some time on detoxification.
A lot of people are accustomed to thinking about detoxification as some sort of woo-woo buzzword that doesn’t mean anything and is only used by scammers.
The truth is that every single human being has built-in detoxification systems in the body to get rid of things we don’t want or need.
Sweat, stool, urine, and breath are the 4 biggest but your body can also eliminate toxins directly through the skin as well.
When it comes to thyroid dysfunction, the thing you should be most worried about is endocrine-disrupting chemicals.
These are chemicals, found in plastics, on receipts, liners of food cans, toys, cosmetics, etc., that are known to directly interfere with thyroid function at the cellular level.
Endocrine-disrupting chemicals, or EDCs for short, are everywhere nowadays, and it’s almost impossible to avoid them.
What’s worse is that some of them are fat-soluble and hide away in your fat cells (7) if they aren’t eliminated quickly enough.
Because they can be hidden away in your fat cells, they can be re-released into circulation as you start to lose weight.
Sometimes this re-release can impair your weight loss efforts and lead to plateaus unless they are actively removed or detoxed from your body.
Not everyone has to put a lot of energy into detoxification therapies, but there are some patients who benefit tremendously from doing so.
This patient was one of those.
She used weekly FAR IR sauna therapy in addition to high-intensity strength training and high-intensity aerobic interval training to promote sweating and toxin elimination.
Sauna therapy combined with this type of exercise promotes hormone balance, more weight loss, and helps eliminate waste through sweating.
Recap of Treatment, Therapies, & Expectations
Thyroid patients who are doing everything correctly should expect a steady 5 to 10 pounds of weight loss each and every month.
There will be some fluctuations in weight loss, though, because weight loss plateaus are not uncommon.
So even though your average weight loss will be 5 to 10 pounds per month, that number can vary slightly.
Many patients nowadays are looking for quick fixes or rapid weight loss.
They want to be able to lose 20 pounds in 1 month or less and believe that if something doesn’t work this rapidly it must not work at all.
This is the exact opposite mindset you want to have when it comes to weight loss.
Weight gain is a slow and steady process (usually) and weight loss is the exact same.
As long as you stay dedicated and consistent with your treatments, you will eventually hit your target weight goal over a period of time.
On average, you should expect it to take somewhere around 6 to 12 months depending on how much weight you have to lose.
To give you a better idea of what this looks like, you can check out the results of this patient over time.
Let’s recap the initial treatment:
| Medications | Supplements | Diet | Detox |
|---|---|---|---|
| Nature-throid | Adrenal Support | AIP | Sauna |
| LDN | Zinc | Ketosis | HIST |
| Selenium | |||
| Vitamin B12 | |||
| Probiotic |
Her results after 3 months included:
30-pound weight loss, 27 inches lost, 80% reduction in symptoms, improvement in hormonal balance by blood tests.
After getting her dose of thyroid medication optimized, we then worked on other hormone imbalances including insulin resistance, low testosterone, and weight loss resistance.
You can see an image of those labs below:

From month 3 to 9 she lost a fairly steady 5-10 pounds per month.
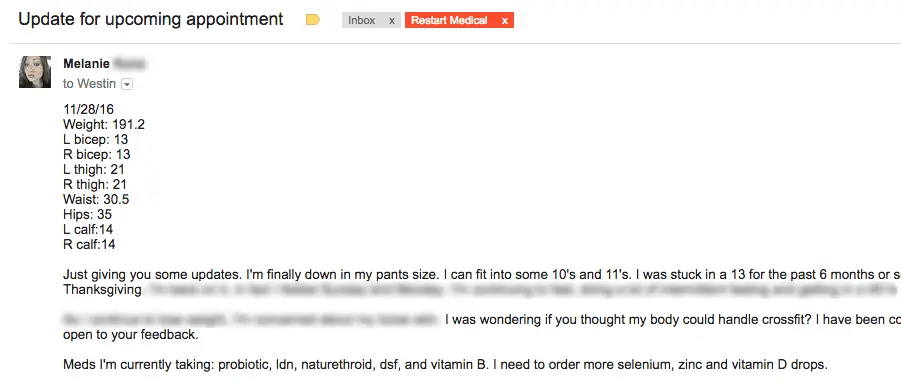
You can see her emails to me including her measurements and results below:


Update #2, 9-month results:
Final Thoughts
I know that losing weight may seem difficult or even impossible if you have Hashimoto’s but it doesn’t have to be.
Hopefully, this walkthrough of this case study highlights this point perfectly.
You can lose the same kind of weight as this patient as long as you are getting and using the right treatments.
The most important part of this patient’s weight loss was targeting her leptin and insulin levels.
Replacing her thyroid hormone resulted in the resolution of her symptoms, but her weight and inches didn’t fall off until we addressed these hormone imbalances.
Now I want to hear from you:
Did anything in this case study surprise you?
Did it all make sense?
Do you see any similarities in your own personal journey?
Are you also struggling to lose weight despite changing up your thyroid medication or changing your diet?
Do you have any questions about this case study?
Leave your questions or comments below!
Scientific References
#1. https://www.mayoclinic.org/diseases-conditions/idiopathic-thrombocytopenic-purpura/symptoms-causes/syc-20352325
#2. https://www.ncbi.nlm.nih.gov/pubmed/21256121
#3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3962576/
#4. https://www.ncbi.nlm.nih.gov/pubmed/19041189
#5. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3962576/
#6. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3138366/
#7. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2726844/








