This is actually a fairly contentious topic but we are going to dive in headfirst.
There are many doctors, and patients included, who believe that the TSH is the single best way to assess thyroid function in your entire body.
I am going to argue that this is completely false and that using the TSH is not only unhelpful for thyroid patients but that it also leads to serious problems in thyroid management.
Patients who rely solely on the TSH as a means to determine whether or not their thyroid is actually functioning well will find themselves being undertreated and continuing to suffer from hypothyroid symptoms despite having “normal” levels.
You may have been told by your current doctor or endocrinologist that the TSH is the ONLY test that you need to evaluate your thyroid and if you were told that, you aren’t alone.
But today I am going to talk about a better way to look at the TSH test in the setting of those with existing hypothyroidism.
You are going to learn:
- Why TSH testing fails to actually test for thyroid function
- What TSH levels you should be aiming for
- Why an “optimal” level is not the right way to look at your TSH
- How I look at the TSH when determining how much medication thyroid patients should be on
- And more
Let’s jump in…
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Why Hypothyroid Patients get Frustrated with the TSH
Remember:
This article is dedicated to people who already have low thyroid conditions such as hypothyroidism or Hashimoto’s thyroiditis.
If you do not have a known diagnosis of hypothyroidism or Hashimoto’s then you would want to look at this article about TSH instead.
Interpreting the TSH level in people who are taking thyroid medication is much different compared to people who are NOT on any thyroid medication.
Back on topic.
Thyroid patients often get incredibly frustrated with their doctor when it comes to TSH.
Why?
Because their doctor is constantly trying to tell them that their TSH is normal even though they are experiencing low thyroid symptoms such as fatigue, weight gain, constipation, etc.
How can you experience low thyroid symptoms while simultaneously being told that your thyroid is “fine”?
Something doesn’t make sense here. Either you are lying (which is obviously not true) or your doctor is wrong when they say that the TSH is a measure of thyroid function.
And, unfortunately, it’s not that you are lying but that your doctor is wrong.
To further complicate the picture, the reference provided for interpreting TSH is incredibly broad.
The standard reference range that your doctor will use to determine if your TSH is “normal” typically ranges from around 0.5 to 5.5 (or something similar).
And your doctor will consider you “normal” if you are anywhere in this range.
Many thyroid patients have realized that this range is far too broad and have found that narrowing the range may help improve how people feel.
This has led to the “optimal” ranges that you see so frequently floating around (you can read more about what I mean by optimal thyroid lab ranges here).
But there’s a big problem with that method as well:
It doesn’t take into account individual variability among thyroid patients.
While it’s generally a good idea to narrow the reference range and shoot for a tighter TSH reference range, you can still run into problems with this approach.
Instead of favoring this “optimal” range that so many thyroid patients are shooting for, I recommend using guidelines to help you determine where your TSH should be.
These are the same guidelines that I use when I treat thyroid patients and they have helped me to treat and manage thyroid conditions in hundreds of thyroid patients.
What is a Normal and Healthy TSH Level for Thyroid Patients?
A healthy TSH level for people taking thyroid medication is much different from those people who are checking to see if they have thyroid problems initially.
A healthy TSH level is somewhere in the range of 0.2 to 2.5.
This is a good measure to use if you are just trying to figure out how you compare yourself to healthy adults.
But we cannot as easily use this reference range if you are taking thyroid medications.
Why?
Because thyroid medications interfere with the TSH system and cause suppression of that system.
In addition, we know that taking thyroid medication and lowering your TSH does not automatically mean that your free thyroid hormone levels are optimized.
And in terms of impacting how you feel, your free thyroid hormone levels are much more important than your TSH.
What to Aim For Instead:
As I mentioned above, instead of focusing on an optimal TSH range you should consider these GOALS.
These goals give you more leeway in what range your TSH should fall into.
They also give you leeway outside of the standard reference range which is going to be required to help EVERYONE feel better.
There are some people who will feel great with a TSH of 2.0 and other people who feel great with a TSH of 0.1.
Figuring out where you fit can be complicated but these guidelines should help get you there:
#1. A TSH Level of more than 2.5 is a problem.
The first thing to know and understand is that the highest you would ever want your TSH to be is around 2.5 (1).
There will always be a small percentage of people who feel great with a TSH higher than this 2.5 range but this percentage represents less than 1% of the total.
For the other 99% of people, consider a TSH of 2.5 to be the highest you would ever reasonably want your TSH to go.
Why this range?

Because you are unlikely to see a HEALTHY adult with a HEALTHY thyroid gland ever have a TSH higher than this 2.5 range.
And as a thyroid patient taking thyroid medication, you want to ensure that your thyroid function closely approximates the same level that someone with a healthy thyroid gland would have.
So regardless of the amount of thyroid medication that you are taking, aim to make sure that your TSH is no HIGHER than 2.5.
#2. A low TSH is Okay if you have hypothyroidism and if you are taking thyroid medication.
We just talked about the high end of the reference range and now we are going to focus on the low end of the reference range.
Some thyroid patients are scared to go below that normal range because they believe that if they do they will automatically become hyperthyroid.
This isn’t true.
A low TSH does NOT automatically guarantee that you are in a hyperthyroid state.
In fact, there are a great many thyroid patients with a low TSH who still remain HYPOthyroid with all of their hypothyroid symptoms to prove it.
On the flip side, you have some people who believe that a low TSH isn’t a problem at all and they almost intentionally suppress their TSH.
This isn’t true either but we will talk more about that in a minute.
What’s important to understand here is the difference between a LOW TSH and a suppressed TSH.
A low TSH is any TSH level that is NOT suppressed but which is under the low end of the reference range provided on your lab tests.
Here is an example:
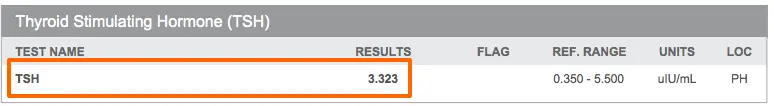
The reference range provided in this example ranges from 0.350 to 5.500.
In this example, any TSH value UNDER 0.35 would be considered “low”.
A suppressed TSH is defined as any TSH level that is undetectable by standard lab testing assays and is usually reported as a value that is less than some specified amount.
If your TSH is suppressed it will come back as < 0.005 or < 0.001 or something similar.
What you need to understand here is that there is a big difference between a LOW TSH and a suppressed TSH.
There have never been reported consequences of a LOW TSH but this isn’t true of a suppressed TSH (more on that below).
The bottom line?
Don’t be afraid if your TSH is low (but not suppressed) and, in fact, this may be something that you want to aim for.
I know from experience that many thyroid patients feel really good when their TSH is flagged as “low” on their lab tests.
The more thyroid medication you take the lower your TSH will go until eventually it becomes suppressed.
If possible, try to get it as low as possible until you feel better and before it becomes suppressed.
#3. A suppressed TSH is probably okay for a short period of time.
The last thing you should understand is that even though suppressing your TSH is not necessarily desirable, it may not be as bad as you are thinking.
As I mentioned before, some thyroid patients believe that a suppressed TSH is of no consequence and may even be desirable.
This is definitely not true as suppressing your TSH absolutely does come with some risks (2).
But those risks may be worth risking depending on your situation.
Consider these examples:
Example #1. A thyroid patient who is 100 pounds overweight.
If there’s an argument to be made for suppressing the TSH it definitely makes sense in the setting of weight loss.
We know for sure that being 100 pounds overweight will increase a person’s risk of diabetes, cancer, heart disease, stroke, and more.
We also know that suppressing the TSH with certain thyroid medications is much more likely to help her LOSE weight.
In my opinion, it makes sense to temporarily suppress her TSH to help her lose 50+ pounds to permanently decrease her risk of these conditions.
Yes, she will experience some increased risk from the TSH suppression but I would argue that this risk is much less than the guaranteed risks she would experience from being 100 pounds overweight.
Example #2. Treatment-resistant bipolar disorder or depression that is negatively impacting your quality of life.
In this situation, we have someone who is suffering from severe depression and bipolar disorder which has negatively impacted her quality of life and may increase her risk of side effects such as suicide.
TSH suppression in these cases, especially with medications such as T3, can dramatically improve both depressive and bipolar symptoms and, in some cases, even reverse them.
I would argue that reducing these depressive symptoms is of paramount importance as the side effects of severe depression may lead to loss of life through suicide.
So doesn’t it make sense to deal with the consequences of TSH suppression for this benefit?
Example #3. A Pre-menopausal woman with severe hypothyroid symptoms that impact her quality of life.
Lastly, there’s a strong argument to be made for TSH suppression in any woman who is pre-menopausal.
It appears that the younger you are, and if you are still menstruating, that the side effects of TSH suppression such as osteoporosis and atrial fibrillation are essentially non-existent (3).
So if you are a pre-menopausal woman AND you are suffering from severe quality of life issues then TSH suppression may be worthwhile.
I absolutely believe that there are some situations in which TSH suppression is beneficial and in which the benefits outweigh the potential consequences.
But, before you suppress your TSH, you better be completely aware of these consequences so you know what you are getting into.
You should have a discussion about the risks versus the rewards with your doctor before jumping in.
Final Thoughts
Optimizing your TSH levels in hypothyroidism is not as easy as you might think.
Instead of focusing on an “optimal” value, I would recommend focusing on THESE guidelines:
- Keep your TSH lower than 2.5
- Don’t worry about a LOW TSH
- A suppressed TSH may be okay in certain circumstances
These guidelines are the same guidelines I use when helping thyroid patients and they have allowed me to help hundreds of thyroid patients feel better and take control of their life.
I should also point out here that even though the TSH has value, there are other thyroid tests that should also be ordered.
These tests include free T3, total T3, free T4, and reverse T3.
If you aren’t able to get these tests then you can at least use the guidelines in this article to help manage your thyroid function.
Now I want to hear from you:
Are you struggling to get your TSH level optimized?
What was your most recent TSH level?
How are you feeling at that level?
Are you planning on trying to push your TSH even lower? Are you planning on suppressing your TSH?
Leave your questions or comments below!
Scientific References
#1. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3267517/
#2. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6416151/
#3. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4746080/








