Are you a thyroidectomy patient struggling to feel better after your thyroid removal?
If so, then this article may help to explain why you are feeling the way that you do.
Article highlights:
- Those without a thyroid are in a unique situation which is different from other thyroid patients.
- Up to 20% of those without a thyroid do not achieve normal free thyroid hormone levels on standard medications such as levothyroxine.
- This reduction in free thyroid hormones can be tested for by looking at the free T3 and free T4 levels.
- Using other thyroid medications, such as Cytomel and liothyronine, may improve this problem.
The Unique Situation of Thyroidectomy Patients
Today I want to focus on a special group of thyroid patients, namely those without a thyroid.
If you fit into this category then you know that even though you are technically still hypothyroid you are still in a ‘class’ of your own.
Those people who don’t have a thyroid find it more difficult to lose weight, find it harder to normalize their symptoms, and overall struggle with a more intense version of hypothyroidism.
And, by the way, the information in this article is relevant to ALL people who do not have a thyroid.
This includes people who have had their thyroid removed through surgical means, it includes those born without a thyroid, it includes those who have had their thyroid ablated from RAI, and it includes those with end-stage Hashimoto’s thyroiditis.
But, back to the question at hand, why are these thyroid patients so much different from those who have a sub-optimal but still functional thyroid gland?
It has to do with the combination of hormones that the thyroid gland produces in a healthy state.
Under healthy and normal conditions, your thyroid produces a combination of both T4 and T3 thyroid hormones.
Even patients who have a sluggish thyroid are still able to produce at least SOME of both of these hormones which are then supplemented by thyroid medication.
But people without a thyroid are not able to produce EITHER of these hormones. And these patients often only receive T4 only thyroid medication.
So, in effect, they are losing two thyroid hormones and only replacing those lost hormones with one.
And, it turns out, this is a big problem for up to 20% of patients who do not have a thyroid gland.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
T4 Therapy Does Not Always Normalize Free Thyroid Hormone Levels
The study I want to focus on for this article can be found here (1).
Among the many important points illustrated by this study is the fact that it showed a certain sub-group of patients without a thyroid are not able to maintain normal free thyroid hormone concentrations with T4-only thyroid medication.
If this sounds confusing to you, don’t worry because we are going to break it down into simple understandable terms.
As a patient without a thyroid, you are probably aware that you need to be on thyroid medication for the rest of your life.
The medication you are probably taking is either levothyroxine or Synthroid as these are the most commonly prescribed medications to treat this condition.
Both levothyroxine and Synthroid contain thyroid hormone but they only contain T4 which is considered the inactive thyroid hormone.
This study showed that up to 20% of patients without a thyroid who are taking these medications are not able to reach the normal healthy levels of thyroid hormone seen in normal controls.
And this promotes a big problem, especially for the 20% of people who fit into this category.
It means that this sub-group of patients will likely experience persistent symptoms of hypothyroidism despite being treated “adequately”.
Understanding the Connection Between TSH and Your Symptoms
As a thyroid patient, you are probably well aware of the thyroid lab test known as the TSH.
You’ve probably been told that this is the most sensitive and best marker for assessing thyroid function.
And while this may be true for some people, it’s not true for all people.
While TSH can be a helpful marker of thyroid sensitivity in the body, it’s certainly not a perfect test.
And relying upon your TSH as the only marker of thyroid function may lead to inappropriate treatment.
In fact, the study that I mentioned previously helps to break down and compare how your free thyroid hormone levels fluctuate based on your TSH level if you don’t have a thyroid.
It also compares these values to those of “normal” healthy adults with a functioning thyroid gland.
This information really helps to visualize the difference in thyroid conditions and highlights the importance of measuring other thyroid hormones such as free T3 and free T4.
Let’s take a look at this image from the study first:
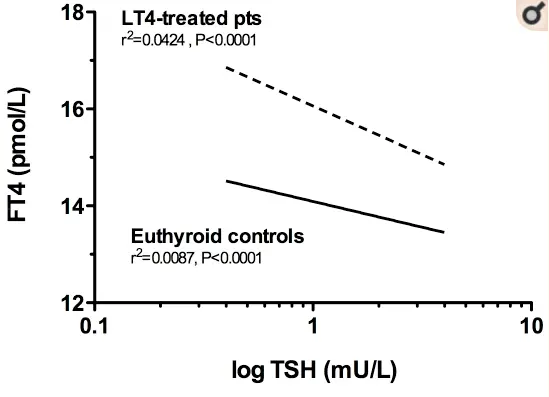
Here you can see the TSH on the X-axis and the FT4 on the Y-axis.
The dotted line represents patients who are being treated with LT4 (which is another name for levothyroxine or Synthroid) and the solid line represents healthy adults.
As you might suspect, as you take more thyroid medication by mouth you would expect your free T4 level to increase and your TSH to decrease.
This is perfectly normal and that is exactly what we see here.
In fact, we see that patients who take T4 medication by mouth actually have a higher free T4 level than those who do not take thyroid medication.
This might seem surprising to you, and you may even think that it’s a good thing, but it isn’t once you understand the function of T4 in your body.
T4 only has potential and hardly has any activity by itself (2).
In order for all of that free T4 in your body to be utilized, it MUST be converted into the active thyroid hormone known as T3.
In order for this to happen your body must take and convert it in a process known as peripheral thyroid conversion.
It’s okay for your free T4 to be high, but only if your free T3 level is also high.
If that were the case then we would be happy and we would expect that you would probably feel well and good.
But that isn’t what we see at all:
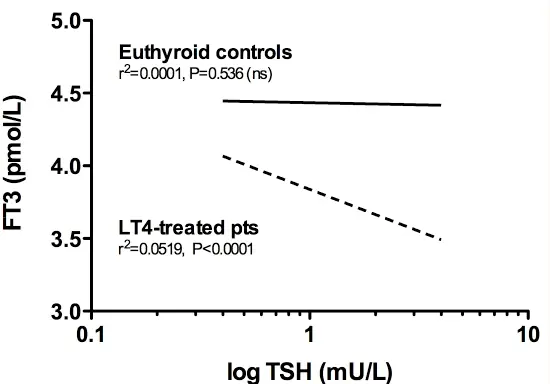
This graph is similar to the other one except on the Y-axis is FT3 or free T3.
In addition, we also see a much different pattern here compared to the free T4 graph.
Here we see that as TSH drops (meaning the more medication you take) the free T3 level increases but it never actually approximates the healthy levels seen in controls.
What does this mean?
It means that a large percentage of patients without a thyroid is not able to adequately utilize the thyroid medication that they are taking by mouth.
The thyroid hormone that they are taking is being absorbed in their intestinal tract, it’s being taken through the blood to the pituitary gland, and it’s even helping to reduce the TSH but it is NOT being converted into the active T3 thyroid hormone.
And T3 is really the only thyroid hormone that we care about because it has all of the biological activity (3).
Put another way:
There seems to be a blockage or something preventing the body from taking the T4 that you are ingesting by mouth and activating it by the body.
And, if you think about it, this makes perfect sense.
After all, why does your body produce both T4 and T3?
There must be an important reason and it probably has to do with the fact that not everyone can function well on one type of thyroid hormone.
The good news is that this appears (so far) to only be a problem for roughly about 20% of patients without a thyroid but it is a big problem for those people.
Symptoms Indicating Your Medication May Be Insufficient
How do you tell if you are among that 20% (or so) of patients without a thyroid who are not doing well on the “standard” treatment?
It’s actually fairly easy and that’s exactly what we are going to discuss now.
For starters, perhaps the easiest way to identify whether you fit into this category has to do with your thyroid lab tests.
If you are someone who doesn’t have a thyroid (because it has been removed or because you were born without one or because it has been destroyed with radioactive iodine) then you should be paying close attention to your lab tests.

But not just the standard lab tests such as TSH as this will not give you the information you are looking for.
At a minimum, you should be looking at TSH in conjunction with both free T3 and free T4.
Remember:
These free thyroid hormones may be the only sign that your body is having trouble converting T4 into T3 so you must check for this.
If you find that your TSH is “normal” (this will typically be defined in various ways by your physician but most physicians agree that a TSH between 1.0 and 2.0 is “normal”) and if you find that your free T3 and free T4 are low then you likely fit into this situation.
But how do we define a low free T3/free t4?
The study listed above helps to define this range but basically, you should be looking for these values to match those found in healthy adults with a functioning thyroid.
If you find that your free t3/free t4 are in the bottom 30% of the reference range or even off the charts low, then this is a problem.
Let’s use an example to help drive this point home:
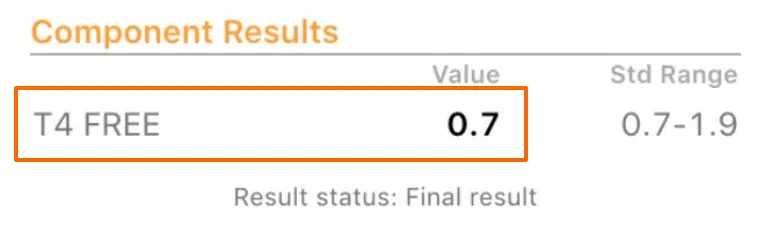
The image above is an example of a free T4 level from a patient of mine.
You can see here that her result is 0.7 while the actual range is 0.7 to 1.9.
Her 0.7 value does fall within the “normal” range but you can clearly see that she is at the very bottom of this range.
Using the reference range of 0.7 to 1.9 and the 30% optimal range I gave you above, you can see that any free T4 value that falls within 0.7 and 1.06 would be considered suboptimal and is probably an indication that T4-only thyroid medication is not sufficient for you.
The 0.7 to 1.06 range was calculated by taking the difference between 0.7 and 1.9 (which is 1.2) and then calculating 30% of the 1.2 value which is 0.36 and then adding 0.36 to the low end of the range 0.7.
This gives you the bottom 30% of the reference range that I previously mentioned.
You can apply this same calculation to your free T3 level.
If you find that one (or both) of your free T3 and free T4 levels are suboptimal AND you are feeling persistent symptoms of hypothyroidism then you are someone who doesn’t fit this standard mold.
While testing is very important (and it is something you should be doing), it’s not the only way to find out if your medication is working for you.
The second way you can tell is by assessing your clinical symptoms.
If you have hypothyroidism and you are receiving treatment for this condition then you should not expect to have continued symptoms with your treatment, assuming your treatment is appropriate for you.
The studies are clear on the matter. They show that the classical symptoms of hypothyroidism track well with thyroid status and thyroid lab tests (4).
This means that you should NOT be experiencing the following hypothyroid symptoms with your treatment:
- Fatigue
- Weight gain
- Constipation
- Musculoskeletal pain
- Cold intolerance
- Weakness
- Depression
- Brain fog
- Memory loss
The presence of these symptoms indicates that your body is not getting sufficient thyroid hormone.
If you have any of these symptoms then your next step should be to evaluate your TSH, free T3, and free T4 as outlined above.
The more difficult part is not identifying that you need further therapy but instead trying to convince your doctor that you don’t fit into the “standard” mold and require different therapy.
Understanding Thyroid Treatment Beyond T4 Medications (What to do next)
If levothyroxine (or Synthroid) isn’t working for you then what are you supposed to do?
This might seem like a big problem, especially if you are inundated with the conventional medical model, but I’m here to tell you that there are MANY thyroid medications that exist beyond levothyroxine.
In fact, I’ve written extensively about these medications in various blog posts throughout the years.
The key to improving your situation is to use medications that contain a combination of BOTH T4 and T3.
T3 is an FDA-approved thyroid medication, just like levothyroxine, to treat those people with hypothyroidism and those without a thyroid.
And T3 can be safely added to your existing dose of levothyroxine or Synthroid (5) to help brute force your free thyroid hormone up to higher levels.
The only problem?
Despite the fact that this is an FDA-approved medication (6) to treat your condition, your doctor may be hesitant (or just downright resistant) to use it.
If this happens to you, then it may be time to seek out a second opinion or look for a physician who is more willing to work with you.
Dosing T3 in the setting of not having a thyroid can be tricky but it is only slightly more difficult when compared to using T4.
T3 has the same effects (although they are more pronounced) on your TSH levels.
Because of this, you really only need a small amount when compared to T4.
While using T3 be sure to keep an eye on your TSH, free T3, and free T4 levels as we discussed in the previous section.
You should aim to get your free thyroid hormone levels up to higher levels. As they increase you should start to feel your symptoms improve.
Conclusion
What I want you to take away from this article is that not all thyroid patients are alike and that you, as a patient without a thyroid, may need different treatment compared to other people even in your same situation.
If you aren’t feeling well, make sure that you test and look into more than just your TSH. By testing and evaluating your free t3 and free T4 you can find out if you are someone who has trouble with peripheral thyroid conversion.
If you do fit into that category then you will likely need a combination of both T4 and T3 thyroid hormones.
It’s also possible that you may be able to brute force your way into a higher T3 level by using increasingly high doses of T4-only medication such as levothyroxine or Synthroid.
This option, while it may work, is not preferable as it will also cause TSH lowering (or even TSH suppression).
If possible, try to keep your TSH within a normal to low range as opposed to suppressing it unless indicated by something like thyroid cancer.
Now I want to hear from you:
Are you a thyroidectomy patient struggling to feel better with thyroid medication?
Have you had this discussion with your doctor?
Have you tested other thyroid lab tests as described in this article?
If so, did you find that your levels were low?
Leave your questions or comments below! It’s helpful to get as much information as possible to share with other thyroid patients.









I am 9 years post-thyroidectomy for CA. Once I started Synthroid/Tirosint I had a 20 lb immovable weight gain. I have never had a weight problem before this! 2 years ago I became insulin resistant/diabetic–another 10 lbs. Apparently, my doctor was “waiting” for this to happen. Victoza is contraindicated for thyroid CA patients so that’s not an option for me. Even Keto didn’t help much. If I am to remain TSH suppressed for the CA treatment, is there any hope of getting the weight off and should I even be fooling around with my numbers? I know my meds have been adjusted due to anxiety and palpitations. I don’t pretend to understand much of this, because I don’t. I am just frustrated and hopeless in my situation. Is there anything left to do?
Hi Maria,
I would start by assessing your thyroid function and thyroid conversion status. From there you can determine if using T3 is a good option for you.
Hello Dr. Childs, I have been diagnosed as subclinical hypothyroid with a TSH of 1) firstly 5.12 μIU/ml and 2) now, 6.98 μIU/ml. My RT3 is 19.0, SHBG 55 nmol/l and most lab values are in a good range. I have been taking NDT ( Thyro-Gold ) for about a month now and have not seen any changes in whatsoever. I told my endocrinologist I would stop because it kind of feels so unnatural to consume hormones and I feel like it would not make any changes since I’ ve been taking it for over a month anyway. I am a male, 25 years of age. So, considering you are one of the few that have enough knowledge to view it holistically, here are my questions :
1) What do you think is hiding behind subclinical hypothyroidism? How can all of a sudden, so many people have problems with their thyroid?
2) Do you think it can be cured without hormones? Have you ever had a patient that from SCH, returned to his/her normal stage without NDT or T4 replacement therapy?
3) Considering I already work with an endocrinologist, but am thinking of contacting you to evaluate my lab tests, how much would that cost? Something like 1-3 email courses. I am asking because I do not know if you do online consultations at all.
Your articles are of great help. I hope you are doing well and thank you in advance.
Dr. Childs,
Thank you for the information in your blogs. I started out with Graves disease about 20 years ago. Had the RAI treatment with it determined that 100% of my thyroid was gone. Ever since I have been on Synthroid or Levothyroxine. I am currently on Levothyroxine 200mcg. All these years I have never felt “Well” and still have all the signs of hypothyroid. I am dieting faithfully, with light exercise but cannot drop the weight. I will lose 2 pounds one week, to gain back 1.8 the next, on the same diet. I am gluten free and low carb, whole foods. After reading your blogs I think I need to add T3 to my regimen. Would you recommend adding T3 or switching 100% to T3 in similar cases? My doc still hasn’t called me on my results so I will be seeking out an integrative med doc, but will have to wait for an opening. I just want to start feeling better/normal. Here are my current labs:
FT4: 1.69
T3: 95
TSH: 0.116
FT3: 2.3
RT3: 30.5
TPO: 15
TPA: 2.0
DHEA-S 536.9 (increasing yearly)
Leptin: 41.1 (not fasting)
I am in the same boat, even my labs are simalar. I started on 5 of t3 for 3 mo. More energy but and dropped a few pounds. But probably time to up the dose a little. My Dr had to be convinced it wasn’t easy but she agreed to try low dose for symptoms.
Dr. Childs,
It’s hard for me to believe that I am still struggling with a thyroid problem at the tender age of 85. I was diagnosed with a hypothyroid condition many years ago, at age 38, and treated for the following 15 years with a prescription for Proloid, 5 grains.
I then moved to an area where there was no one interested in me or my medication, but for a few months, I continued to receive Proloid until it was removed from the market. It was replaced by Euthroid which was quite simply the perfect medication for me. It, too, was then taken off the market. A pharmacist’s attempt to compound did not work.
Then, I was on Armour Thyroid for the next 25 years until my doctor closed her practice and was replaced by an endocrinologist. I had since learned that endocrinologists did not believe I had ANY thyroid problem, and that doctor was no different.
I, unfortunately, am in the care of another doctor who believes in the TSH as a guideline, and I have been on 0.088MG levothyroxine for the last year and a half.
My energy level has dropped significantly, I have no nails, I have no balance, and I fall asleep whenever and wherever I sit down. There is no doctor in this area that I know of, and I cannot travel to an area where there might be one.
Any ideas, or do I just slowly fade away?
Hi Ellie,
The only option I can see for you would be to find a physician who can give you a different prescription. I would do whatever it takes to find one even if it means traveling. To me, it would seem that the sacrifice is probably worth the improvement in your quality of life.
Hi, Dr. Childs,
I had a total thyroidectomy 18 months ago, after my latest bout with Graves 2 years ago when the ATD just wasn’t working this round. I was originally diagnosed with graves 15 years ago.
I’ve been fighting the battle with medication ever since my surgery and finally left my endo office to a new one because they were medicating me solely based on my TSH and were ignoring my symptoms. Sluggish, weight gain, hair loss by the handfuls, low temp, etc.
My TSH has remained suppressed since surgery and they can’t get it to go above .012. However, my FT3 and FT4 consistently stay low normal range, below the 30 percent. They continuously fluctuate a few points each draw.
My new dr has finally climbed on board and is now beginning to assume my pituitary is just sluggish and that he needs to focus more on the FT4 and FT3. He did have me stop my Cytomel cause he was concerned that was causing my TSH suppression. But now he is on a hunt to try to prove that I am NOT hyperthyroid like my labs suggest. He ordered sex binding hormone and prolactin. I haven’t gotten the results on the SBHG but my prolactin came back normal.
I’m wondering what your opinion is on this. Is this true that my pituitary could just not be responding well and creating tsh like it should from my Synthroid? Does it sound like we are on the right track running all these other tests? Should I encourage him to let me start up cytomel again to try and increase my FT3? I still feel sluggish and can’t seem to lose weight. I’m a high endurance athlete and exercise regularly and eat low carbs.
Are there any other things you can recommend to assist with conversion? Would your supplement help with this and help to increase my suppressed TSH and increase my
T3 and T4?
Thank you for all your wise information on navigating this life without a thyroid.
Hello Dr. Childs,
I had a total thyroidectomy about 10 years ago. Currently taking both T4 (100ug Euthyrox) and T3 (20mcg Tertroxin). My lab results however indicate very low TSH (0.13 uIU/mL) low T4 (0.73 ng/dL) and low T3 (3.12 pg/mL). Based on the information, I should lower my T4 intake to increase my TSH, but the FT4 is also low – what to do now?
Thank you for very informative articles.
I had my thyroid gland removed 18 years ago because of papillary thyroid cancer. Had no problems for approx. 10 years and then various different problems, bone loss, inability to deal with heat, aches & pains in muscles. etc I take 100 mcg levothyroxine daily ( I used to take 150mcg in the early days after thyroidectomy). I realize that with Levo I get no T1 & T2 (do I need these trace hormones)? I would like to try Armour or another type of NDT but am scared because of my history and not sure how to change over. Also, my Dr who I see once a year thinks NDT dangerous and unreliable and possibly would not see me at all if I went down that route. I do worry that my body has had no T1 & T2 for 18 years. Thank you.
Male 58 years. I had the thyroid removed in 2nd operation following nodule removal. Pearl size spot of papillary cancer found after 2 biopsies… No treatment required other than total removal. I have consistently had terribly bad reactions to all brands and doses of t4 and Armour. Debilitates me. Can’t work. After Tirosint, neck hurt and diagnosed with deteriorating cervical spine. Kills me. Nausea, severe itching, sweating, double blurry vision. with any dose. Not taking anything but supplements right now. Will my liver eventually take over production of T3 on its own?
Thanks for caring about us. Few really care or understand the magnitude of this disability.
Ok total thyroid removal 30 yrs ago, ups and downs, TSH always low so the dr says I’m getting too much synthroid. I will not lower synthroid because on this dose I feel good, do you still suggest Cytomel?
Margerite
Hi Dr Childs,
I am in my 9th year of post-thyroidectomy. What a journey! Synthroid only therapy was not for me. I managed to get to optimal on WP+liothyronine, as well as on NP+liothyronine, but shortly after I reached optimal levels, NDT formulation changed. I am currently figuring out what my next step should be in terms of treatment. For someone who has issues with fillers, as well as has to work hard to keep iron and D3 levels at a low end of normal range, what would you recommend? Should I re-try WP + liothyronine? Or would you recommend getting off NDTs and trying Tyrosint or Tyrosint-Sol plus liothyronine? Thanks very much!
I have had thyroidectomy, 2017 . I’ve had a difficult time with finding a dose of synthroid that helps my symptoms. Specialist seem to be uncompasionate about symptoms and only care about the numbers. So I am treating with my gp, she is compassionate but not knowledgeable. So together we have got the numbers good but symptoms persist. I am going to refer her to your findings in hope of receiving t3 supplements. I will let you know of my improvement. Th for this information. GOD bless.
Thank you for a very interesting and informative article. I’m a retired R.N. who had a total thyroidectomy in 1998, with a dx of thyroid papillary carcinoma. I was forty when I had the surgery, and up to that point, in excellent health. Since, I have struggled with chronic fatigue. My FP ran several tests to R/O any disease processes; none were found. I also have very dry, brittle hair and nails, whereas prior to my surgery, I had soft, healthy hair, and strong, hard nails that grew well (now they are fragile and break easily). I do also suffer from peripheral neuropathy in both legs, feet, and hips(and am unable to tolerate meds to help those symptoms, only take Tramadol and Norco for pain, and it only relieves about 50-60% of the pain). Also have a dx of fibromyalgia. I do have a new physician who is willing (FINALLY!!) to have me try taking T3. I am hoping to get relief from my chronic fatigue at last. I just want to thank you for pointing this out for people. Some may not have been aware of this until now.
thyroid removed when I was 17, I’m now 79, been taking some form or thyroid medication all my life, i know the feeling when thyroid is not right. recently dealing with high blood pressure issues, doctor has increased dosage of blood pressure medication, I mentioned my thyroid and said I have experienced some issues with thyroid such as hot flashes, pulsating in my fingers sleeping problems and fingers being subject to getting very cold easily. currently taking levothyroxin, TSH level in december was 0.316. medication recently was changed from 100mcg to 88mcg. my symptoms persist any suggestions
Hi Dr Childs
I had my thyroid removed in 1999 and for the last 3 or 4 yrs been having trouble with hypothroidism my test numbers go up and down I am on 88mg Levexyl and the doctor adjusts it to 1/2 pill extra a week and that works for awhile and I feel good but then I start feeling terrible again and he takes me off the extra 1/2 pill. How can I keep my medication at a good level to keep my test numbers normal.. I get very tired, fast heart beat, weak and cold chills…. Thank you Carole
Hi Carole,
The first place to start is with you a complete thyroid lab panel that includes free T3, total T3, and reverse T3. If you are like most thyroid patients then you will probably find that you need additional T3 thyroid medication (not more Levoxyl). You can read more here: https://www.restartmed.com/normal-thyroid-levels/
I have had my thyroid removed due to cancer, and thru great research have found that I was unable to digest , due to low bile levels, which took my gallbladder , which is how you convert T4 to T3, so I take 1 bile salts tablet in am with synthroid, and at lunch take zinc and selenium to help with conversion as well, this has help immensely with bringing my numbers to what is close to normal, if there ever is a normal,I feel good, and T3 levels seem to be increasing steadily, I hope this helps someone, we are a work in progress ….good luck
Hi Shirley,
Thanks for sharing and glad you found what worked for you!
I had a partial removal and despite that golf ball size adenoma with 10lbs of water bloat I felt fairly normal except for some slight fatigue. Even after my partial I didn’t take Levo until two years later. At that point I had a low appetite and some slight fatigue with a TSH of 5 but I still felt fairly normal and active. I was on a plane to tour Europe when my Dr. office called to tell me that my TSH was 5 and should go on Levo. On that trip I hiked up and down Castle Neuschwanstein with no problems! Once I returned they put me on Levo that’s when all the symptoms started up but it took about six years on T4 only to completely crash.
Hi Sarah,
There are certainly some people with half a thyroid gland who do not require thyroid medication but it seems that those people are much more susceptible to subtle changes in thyroid function compared to those with a full gland. Given that, it’s not surprising that over time your thyroid function could decline and eventually require more thyroid medication. My experience suggests that those with half or all of their thyroid gland removed typically do much better on combo T4 + T3 thyroid medication. Your story of eventually crashing on T4 only thyroid medication is not uncommon, unfortunately.
I am 78 and had my thyroid zapped when I was about 50 when I was diagnosed as having a goiter and Graves’ disease. Since then I have been on the thyroid merry-go-round. I currently take 100mg of levothyroxine and 10mg liothyronine. Because my TSH is less then .02 my endocrinologist says I am hyperthyroid. At the same time I have far more symptoms of hypothyroidism: difficulty losing weight; constipation; headaches; and muscle and joint pains. I had a DNA test that showed a DIO1 gene defect.
My mother at my age also had thyroid problems, having been diagnosed at the age of 6 or 7 as having no functional thyroid. On her 70s her doctors told her she was hyperthyroid (TSH test) and when they continued to decrease her medication she became hypothyroid and developed hardening of the arteries and a number of related health problems. She was miserable up until she died.
My medical tests show that my heart is in great shape. I try to walk 30 minutes four or five times a week and feel fair overall. I was diagnosed with osteopenia in my hip several years ago.
Thyroid problems run in my family. Three of my mothers’s aunts had thyroid problems (father’s side). My daughter was diagnosed with thyroid problems when she was 12 and had RAI.
I am just trying to get someone to listen to me and help get my thyroid balanced.
Hi Eileen,
The single best thing you can do is spend some time and energy finding a thyroid-literate doctor! I created this resource to help with just that: https://www.restartmed.com/how-to-find-a-doctor-to-treat-your-thyroid/
Graves autoimmune hyperthyroid disease runs in my family. Many of us had to have RAI and no longer have a thyroid. Problem is, none of us convert the Synthroid (t4) very well. I don’t know what this means. I have T4 levels at the upper range of normal and T3 levels at the lower end of normal. My sister said her DNA test showed a problem with “Deiodinaze” and SNP.
I tried adding T3 Cytomel to my 88mcg of Synthroid and started to have heart “fluttering/palpitations.”
Now I have been told that I have “Hyperdynamic LV Systolic FX > 70%.
I don’t know what this means either, but I am thinking it is somehow connected with the T3 medication.
Hi Mary,
T3 thyroid medication can cause a reversible type of cardiomyopathy but this usually takes a long time to develop and requires very high doses. It may be possible that your T3 is somehow connected to your heart function but it doesn’t appear to be causal, at least not with the information provided.
Hello! I had a follicular neoplasm while I was pregnant in 2011. I had my left lobe removed in my second trimester, then my right lobe removed when my daughter was 3 months old. I’ve felt like crap since!
Being a military spouse, I move every 1-2 years, so it’s nice when my endocrinologist is terrible, but it feels like I’m fighting the same battle over and over.
I’ve had doctors who want me to be in the dead center of the TSH range (like it’s a point) and all my symptoms are just a “coincidence.” I mainly have doctors who have a medicine they push or a spot on the range they like, regardless of how I feel. I did have a doctor in England who kept me suppressed because I never received RAI — I felt pretty good then.
I’ve been on levothyroxine, synthroid, synthroid + cytomel, NP, Armour, and Tirosint. I feel the best on NP, but many pharmacies don’t carry it, so I take Armour as a second choice. My most recent doc required I switch to Tirosint.
During the seven weeks I was on it, I had stomachaches daily, headaches daily, gained 7 pounds, and was so exhausted every day that it was painful — among other problems. After I did my labs, I switched back to Armour and felt better almost instantly. She told me she wouldn’t see me anymore if I wasn’t going to “stick to the plan.” I’m now waiting to get a referral to another endo.
Every doctor takes different labs — most never take free T3. However, my TSH is always suppressed (0.02mcIU/mL). I’ve been told that the level is too low and it could affect my heart. However, I’m to the point where I’d rather drop dead at 50 (11 years from now) and feel good up to that point, as opposed to live to 80/90 and feel terrible every day.
In December, I had a suppressed TSH, high-end of the range free T3, and mid-range free T4 labs done. My February labs were a suppressed TSH and a high-end of the range free T4, without free T3 tested.
I’m a fitness instructor and nutritional coach, so I eat clean and work out a lot — I make sure I walk 7-10 miles on days I don’t work out… but I can’t lose weight to save my life. My brain is foggy and I have trouble getting words to come out of my mouth. I don’t feel like my 135mg of Armour a day is the best dosage for me, but everything else I’ve tried has been exponentially worse. I’m almost 40 and gaining weight is agony because it’s so hard to lose. If I were eating cake and pizza and earning the gained weight, that’d be one thing… but working out, eating clean, and gaining FAT is NOT OK. I know there is something wrong, but I can’t find a doctor who wants to find out what will enable my body to work properly.
I’m to the point where I think all endos should have to have their thyroids removed to even remotely understand our issues!
Hi Jennifer,
I know it’s frustrating, but it’s just very hard to lose weight after thyroid removal unless your thyroid is as close to optimized as you can get. That almost always requires combination thyroid replacement with T4, T3, and T2. T4 and T3 require a prescription but you can get T2 as a supplement: https://www.restartmed.com/product/essential-t2/
I take levothyroxine (100mcg) daily. My thyroid levels were checked recently. My TSH was 0.297. Normal was reported to be 0.45 – 4.5.
My T4 was 1.31 with normal reported to be 0.82 – 1.77.
My T3 was 2.9 with the norm reported to be 2.0 – 4.4.
My dr. Recommended that I skip my levothyroxine one day a week which seems a bit odd to me. And then be retested in 2 months. Does that make sense?
Hi Helen,
Yes, that is a strategy that some doctors use. I think there are far better options available, but every now and then skipping a dose can be beneficial. It’s just a way to average out a lower dose on a weekly basis.
I have no thyroids, I take 0.20 of Levothyroxine(Generic) My TSH Serum plasma is 14 and my T3 is, T4, free serum is 1.03, T3 free is 1.96
Hi Michelle,
It looks like you could use some more thyroid hormone!