Pregnancy alters what is considered “normal thyroid function” in the body.
The changes that occur during pregnancy are, therefore, very important to understand if you have thyroid disease (or suspect you do).
This guide will walk you through everything you need to know about your thyroid and pregnancy including symptoms that indicate you might have thyroid disease, how to manage thyroid medication during pregnancy and what thyroid antibody positivity means.
Let’s jump in:
Does Pregnancy Cause Thyroid Disease?
If you are pregnant or planning on getting pregnant, then there are a few things you need to understand about your thyroid and how it may impact your pregnancy and child.
Your thyroid function is critical to the development of your child.
Why?
Because, in the beginning, your child is dependent upon your thyroid function until it can start to produce its own thyroid hormone.
It’s also been shown that hypothyroidism during pregnancy, even by a small amount, may result in developmental issues including a lower IQ in your child (1) if it is not treated appropriately.
For these reasons, it’s absolutely critical that you have an understanding of how thyroid disease may present in pregnancy, how to identify if you are having issues and how to go into pregnancy with expectations if you have existing thyroid disease.
Because thyroid disease is actually quite common among pregnant women, many women ask the question:
Does pregnancy cause thyroid disease?
The answer is that pregnancy probably does not cause thyroid disease by itself, but rather it sets a situation up in which existing thyroid disease is exacerbated.
It’s not uncommon for some women (and men) to have low-grade thyroid disease, known as sub-clinical hypothyroidism, which isn’t identified or treated.
This type of thyroid disease may be the result of inflammatory diseases, obesity (2), existing autoimmune disease, or nutrient deficiencies.
So, because pregnancy puts increased metabolic demand on the body (3), it may be that small and existing thyroid disease is more pronounced during pregnancy (and after).
So it’s not that pregnancy leads to thyroid disease so much as it reveals existing thyroid problems.
Now it’s certainly possible to develop thyroid disease WHILE you are pregnant as well, but this may be less common when compared to women who start with existing thyroid disease.
So how do you know if you have thyroid disease?
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
How to Identify Thyroid Symptoms During Pregnancy
Luckily, because thyroid function is so critical for the development of your baby testing for thyroid function is considered standard operating procedure once you are found to be pregnant.
So your doctor should automatically assess your TSH during your first set of routine blood tests.
But is this testing enough?
It turns out, and we will talk about this more below, that certain changes occur in pregnant women which makes standard thyroid testing less valuable when compared to other tests.
But in addition to testing, you also want to familiarize yourself with the symptoms of thyroid disease.
Why?
Because these symptoms are often the first sign of trouble (lab tests tend to follow) when it comes to your thyroid.
The problem is that some of the general symptoms of thyroid disease may tend to mimic “standard pregnancy symptoms”.
Often thyroid symptoms tend to be more exaggerated when compared to pregnancy symptoms, and with the addition of lab tests, you should be able to easily identify the issues.
So how do thyroid symptoms manifest in pregnancy?
You want to be familiar with both hyperthyroid (too much) and hypothyroid (too little) symptoms.
Symptoms of hypothyroidism (meaning too little thyroid hormone) include:
- Excessive fatigue
- Excessive hair loss
- Rapid weight gain (more than what is expected)
- Cold extremities and intolerance to cold temperatures (you find yourself wearing sweaters in the summer or wearing socks to bed)
- Very dry skin
- Memory issues or difficulty concentrating
- Slow fetal growth
As you can see, many of these symptoms may mimic normal pregnancy symptoms but you can usually separate the pathologic symptoms because they tend to be more profound and excessive compared to whatever your baseline is.
So if your fatigue is normally a 4/10 on a scale, you might find it jumps up to 7/10 out of the blue and stays there.
Symptoms of hyperthyroidism (meaning too much thyroid hormone) include:
- Rapid heart rate or heart palpitations
- Difficulty breathing or shortness of breath
- Tremors in the hands
- Insomnia or difficulty sleeping
- Weight loss or slower than normal weight gain
- Slow fetal growth
If you are experiencing any of these symptoms then you should have your thyroid lab tests evaluated as soon as possible.
Don’t be afraid to speak up about your existing symptoms.
Even if they show up negative you will have peace of mind knowing that your baby is safe.
The worst thing you could do is to ignore these warning signs and potentially put your baby in harm’s way.
Pregnancy increases Thyroid Hormone Requirements (Why you need to increase your dose during pregnancy)
Another very important point to understand is that the demand for thyroid hormone increases during pregnancy.
What do I mean?
I mean that whatever amount of thyroid hormone that your body produces naturally when it is healthy is INCREASED when you are pregnant.
Now, this isn’t normally an issue for women with a healthy thyroid gland, but what about women who are taking thyroid hormone?
What you may not realize is that when you are taking thyroid hormone you are effectively shutting down the natural ability of your thyroid gland to produce thyroid hormone.
So you are dependent upon the DOSE of thyroid hormone that you are currently taking.
This means that if you are taking thyroid hormone and you become pregnant you will need to have your thyroid dose adjusted.
And for most women, this means INCREASING your dose (not decreasing).
This change in dosing should occur as soon as possible as well.
The increase in demand for thyroid hormone comes because your baby has a demand for thyroid hormone.
So the amount that you normally take is only sufficient for your body, and it doesn’t take into account the need of your baby.

But how much more thyroid hormone will you need when you become pregnant?
The answer is that it depends on the person, but studies show that on average your dose may need to be increased anywhere by 40% to 100% (4).
So this means that if you are taking 50mcg of T4 (Synthroid or levothyroxine) you may need to increase your dose up to 75mcg (50% increase) to 100mcg (100% increase).
And, again, this increase in your dose is absolutely necessary because your thyroid may not be able to naturally increase the amount of hormone necessary for your child.
This also means that increasing your dose as soon as possible is of utmost importance (preferably during the first trimester after initial labs have been drawn).
Pregnancy Increases Iodine Demand (Which means you need more Iodine)
Remember when we were talking about thyroid disease potentially revealing existing thyroid issues?
Well, part of this issue may come from iodine usage and demand during pregnancy.
To help illustrate this point we can look at basic studies which outline the demands of iodine uptake and usage for normal men and women.
We know that men and women need around ~150mcg of iodine per day to keep up with the demand for thyroid hormone production in the body (5).
Most of this iodine must come from your diet such as iodinated salt or from sea vegetables.
But we also know that pregnant women, and lactating women, need up to 290mcg of Iodine per day (6).
We also know that the average consumption of iodine per day is around 130mcg (7).
Do you see the problem?
On average we are consuming barely enough to meet the demands of normal day to day thyroid needs, but when you throw it pregnancy and lactation the consumption of iodine may be insufficient.
Because of this, most prenatals do contain extra iodine, such as this one.
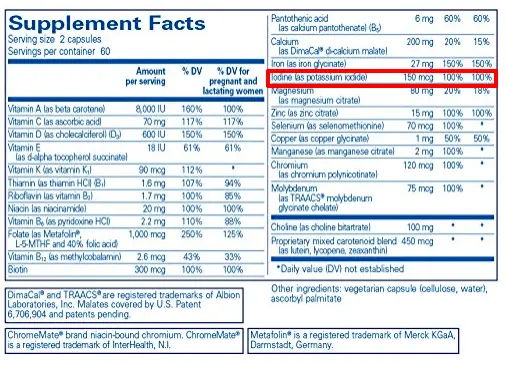
But the amount of iodine in most prenatals is usually around 100-150mcg per day.
If you are consuming the regular amount of 150mcg from food sources then the added 150mcg of Iodine from your prenatal is probably sufficient.
The key here is to be mindful that more factors are involved in thyroid function during pregnancy so be aware of the foods that you consume and make sure to check for iodine in your prenatal vitamin.
If you have a history of thyroid disease or suspect that you have an increased risk for developing thyroid disease during pregnancy, it may be wise to avoid goitrogenic foods (8) (those foods that reduce thyroid function) and increase your consumption of sea-vegetables (natural iodine foods).
It’s also important to continue this supplementation of Iodine through lactation if you are breastfeeding.
This mismatch of Iodine intake and demand may be enough to manifest slight hypothyroid symptoms in your body (please see the symptom list above).
Thyroid Antibodies and Pregnancy – Is it Hashimoto’s or something else?
It’s important to remember that pregnancy is a condition which is quite taxing on your immune system.
Your body must recognize the difference between its own tissues and the tissues of your baby.
Your immune systems primary goal is to eliminate and kill invaders, but even though we know that the fetus is “foreign” it’s not something we want your body to attack!
These are the exact same antibodies that we see in autoimmune thyroiditis or Hashimoto’s thyroiditis, but is your body actually attacking your thyroid?
The exact situation is unclear but it looks like the presence of thyroid antibodies in your serum does not necessarily mean that you have Hashimoto’s (if it comes DURING pregnancy).
In most situations, these antibodies will fall after delivery, but that doesn’t mean you are out of the clear just yet.
The presence of antibodies in the serum during pregnancy does increase your risk of developing both maternal complications and thyroid disease later in your life.
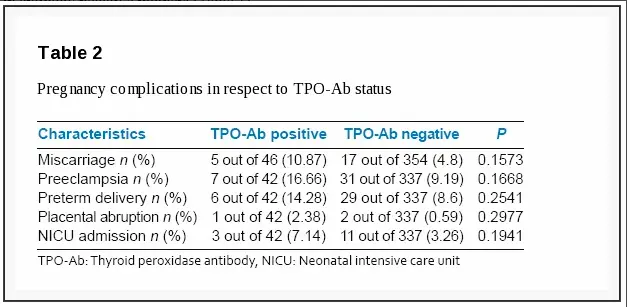
But this begs the question:
Should assessing for thyroid antibodies be part of routine screening for pregnant women?
There is a good case to be made and it is something that I often do and recommend.
In my experience, I find having this information to be very helpful, especially in monitoring the pregnancy and in monitoring thyroid function after birth.
It’s helpful information to have, especially if the pregnant woman starts to develop postpartum depression or excessive hair loss after her pregnancy.
But your physician may feel differently.
With up to 11% of pregnant women having positive antibodies in their serum during pregnancy, it may be worthwhile assessing for this simple lab test.
The most important thing to realize is that while a huge percentage of women may have positivity to these antibodies it does NOT mean that their thyroid function is compromised.
In fact, the vast majority of women who fall into this category are considered to be “euthyroid” which is to say they have normal thyroid function.
On the other hand, it is also possible that some women may go into pregnancy with undiagnosed Hashimoto’s thyroiditis and may, therefore, fall into a different category.
So how do you differentiate these patients?
Often those women with Hashimoto’s will have hypothyroid-like symptoms BEFORE pregnancy and these symptoms may be worsened after they become pregnant.
If you are one of those women who have positive thyroid antibodies during pregnancy just realize that you have about a 20-40% chance of developing permanent hypothyroidism at some point later in your life (10).
Testing for Thyroid Disease During Pregnancy
If you suspect you have thyroid disease and you have the symptoms of thyroid disease then what is your next step?
Your next step should be to evaluate thyroid function in the serum with basic thyroid lab testing.
But this may be easier said than done.
The problem is that pregnancy results in the release of several hormones which all impact thyroid function (these include human chorionic gonadotrophin and chorionic thyrotrophin (11)) which may make the “standard” interpretation of TSH less valuable.
Because the TSH may be less helpful in pregnancy you will also need to assess for the free thyroid hormones (Free T3 and Free T4) (12).
So, if you are pregnant, what is considered the “complete” thyroid panel?
The following tests will give you the most information regarding your thyroid:
- TSH (Thyroid stimulating hormone) – Your TSH will help you understand the pituitary function and its response to thyroid hormone in circulation.
- Free T3 – Free T3 represents the active thyroid hormone and is the most biologically active thyroid hormone.
- Free T4 – Free T4 is another biologically active thyroid hormone but less active than T3. It’s helpful to understand this value because it will help determine how much thyroid hormone is in “reserve”.
- Thyroid antibodies (Both Thyroglobulin Antibody and Anti Peroxidase Antibody) – These thyroid antibodies may be a sign of Hashimoto’s or they may give you insight into your future risk of developing thyroid disease after pregnancy.
Thyroid testing, if thyroid disease is suspected, should be assessed as early as possible in your pregnancy (preferably with other routine tests).
If an abnormality is suspected based on lab testing then supplementation with thyroid hormone should be the next step.
The reason for this aggressive treatment is because the fetus is dependent upon maternal (the mothers) thyroid hormone supply for the entire first semester and up to mid-gestation.
There may be some instances where you want to try all natural approaches to therapies, but this is not one of them.
The lack of thyroid hormone to the fetus may result in miscarriage or development issues.
Your Thyroid and Infertility
What if you are having a hard time getting pregnant or if you are suffering from miscarriages?
Thyroid disease may be the cause.
Even though hypothyroidism occurs in only a few percentages of the population, thyroid disease is found in up to 20-30% of women suffering from infertility.
The good news?
The hard part isn’t necessarily treatment but identifying the disease in the first place.
Your thyroid helps regulate progesterone levels and progesterone is required for sustaining pregnancy in early pregnancy (15).
Low thyroid function also causes menstrual irregularity which may lead to inconsistent cycles or anovulatory cycles (cycles where you don’t ovulate).
These issues can all be caused by minor changes to thyroid function which may not be picked up by standard lab tests.
Because of this, some maternal-fetal medicine practitioners maintain very strict guidelines regarding the “normal” range of those who are having issues with fertility.
If you are having issues with either getting pregnant or maintaining your pregnancy then you should closely evaluate a standard thyroid lab testing panel with optimal ranges in mind.
You can read more about how this idea here.
Final Thoughts
The bottom line?
As a pregnant woman (or someone trying to conceive) make sure that you understand the basics of thyroid hormone and how it may influence your pregnancy.
Testing and understanding thyroid issues are especially important if you have a family history of thyroid disease or if you suspect you may have thyroid disease going into pregnancy.
The best way to avoid complications secondary to thyroid dysfunction is to go into pregnancy with your thyroid optimized.
Taking this approach will limit complications and ensure that you do not experience exaggerated symptoms during your pregnancy.
Now I want to hear from you:
Are you currently pregnant?
Do you have or suspect thyroid issues?
Is your physician willing to work with you?
Why or why not?
Leave your comments below!








