The answer is yes!
But what I find in most patients is that the underlying cause of high blood sugar is typically not the thyroid.
Even though thyroid function can play a role, it’s usually other underlying conditions such as how much stress you are under, how much thyroid medication you are taking, what types of foods you are eating, how much inflammation is in your body, and more, contributing the most.
The good news is that managing your blood sugar if you have hypothyroidism is possible.
The bad news is that it may take a little more work compared to someone that doesn’t have thyroid problems which is exactly what we are going to be discussing today.
In this article, you will learn:
- The connection between insulin resistance and hypothyroidism
- The connection between blood sugar and insulin levels
- How insulin impacts your weight
- How to treat insulin resistance if you have hypothyroidism
- And much more
Let’s jump in…
High Blood Sugar Stems from Insulin Resistance (& Sugar Consumption)
Treating high blood sugar is incredibly important from an overall health perspective but also from a weight loss perspective.
Why?
Because the fact that you have high blood sugar is usually a sign of something known as insulin resistance.
You’ve probably heard of insulin in the past but perhaps you didn’t really understand its significance.
So what exactly is insulin?
Insulin is a hormone secreted by your pancreas typically in response to food (1) but stress can also stimulate it.

Your body produces insulin after you eat a carbohydrate-rich meal because it wants to utilize the energy you just consumed.
Insulin acts to take that sugar and push it into your cells thereby storing it for later.
And this is a good thing, usually.
Insulin is just a hormone doing its job but, under the right circumstances, can become dysregulated (2) that’s when it becomes an issue.
This is why understanding the distinction between the hormone insulin and insulin resistance is important.
Insulin resistance is a state of cellular resistance to insulin that occurs in response to repetitive and repeated carbohydrate (sugar) intake.
And that’s when things start to become a problem.
As your body becomes resistant to insulin, your blood sugar will rise (3) because your body has a harder time putting inside of your cells.
This leaves extra sugar floating around in your bloodstream instead of inside your cells where your body wants to put it.
This blood sugar starts to bind to things in your body including your red blood cells (this is where the hemoglobin A1C test comes in) and can even damage organs and tissues (such as your kidneys and eyes).
Insulin resistance is actually quite common, especially among hypothyroid patients.
The incidence of insulin resistance is estimated to be around 50% (4) of the adult population in the United States.
Among hypothyroid patients, this percentage is likely far higher given the connection between your thyroid and insulin levels.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Hypothyroidism and Blood Sugar
It turns out that your thyroid is actually a potent modulator of both insulin and glucose (sugar) metabolism (5).
What does that mean?
It means that if there is something wrong with your thyroid function then it will almost always affect your blood sugar (6) in some way.
This effect occurs independently of other factors which may trigger insulin resistance (such as stress or sugar consumption).
What this means is that patients with thyroid disease, of any type, are at higher risk of developing insulin resistance because of their thyroid condition.
And I find this to be true.
It’s rare that I see someone with hypothyroidism who doesn’t also have insulin resistance (this also applies to hyperthyroid patients (7), by the way).
It is likely the case that at least some amount of insulin resistance was present before the diagnosis of hypothyroidism in most people but that insulin resistance was then made worse by the added thyroid problem.
Thyroid hormone, under normal conditions, is supposed to act to help your body get rid of excess sugar inside of your cells.
In this way, it opposes the action of insulin.
The interplay of thyroid hormone and insulin/blood sugar is actually more complex than that (8), but this serves to drive home the point.
If there is an issue in thyroid status (meaning that your thyroid levels are abnormal) then it will always affect your blood sugar and insulin receptor sensitivity to some degree.
It’s best to think of the connection between thyroid function and blood sugar as a balance.
If thyroid hormone is too low then it will result in high blood sugar and insulin resistance.
On the flip side, if thyroid hormone is too high then it will also result in insulin resistance and high blood sugar.
You want your thyroid status to be just right in order to balance blood sugar.
This also means that patients with hypothyroidism or low thyroid function are at a distinct disadvantage when compared to other healthy people when trying to treat insulin resistance.
Why?
Because the current treatment paradigm for hypothyroidism may leave up to 20% of thyroid patients ‘undertreated’.
You will know if you fit into this category because you are likely already taking thyroid medication but still experiencing low thyroid symptoms.
You can also fit into this category if you have a normal TSH but low circulating free thyroid hormones such as free T4 and free T3.
In either case, the result is the same, you do not have sufficient thyroid hormone in your body to balance the effect of insulin.
This means that treating insulin resistance and losing weight will always be more difficult for thyroid patients unless their thyroid medication dose is optimized.
You can also obtain thyroid optimization through the use of natural thyroid remedies so don’t think you necessarily have to use medication to get there.
Regardless of the situation, though, your goal should be to obtain 100% thyroid optimization to make treating insulin resistance easier.
Does Thyroid Medication Worsen or Treat Insulin Resistance?
It is well known that there is a connection between the thyroid and blood sugar which is why thyroid patients often ask how thyroid medication fits into this equation.
After all, thyroid medication contains active thyroid hormone and, therefore, will impact blood sugar levels when taken.
How your thyroid medication impacts blood sugar depends on many factors, though, and is not as straightforward as you might think.
First of all, how much thyroid medication you are taking is very important.
What do I mean?
How well are you being dosed?
Is your dose allowing you to obtain 100% normal thyroid function? Are you taking too much thyroid hormone? Or are you taking too little thyroid hormone?
When doctors prescribe thyroid medication they try to get you as close to normal as possible but this rarely happens.
Instead, it’s not uncommon for thyroid patients to experience bouts of high thyroid function and low thyroid function as they try to adjust their dose.
These ups and downs in thyroid dosing obviously will impact insulin and blood sugar levels.
Because of this, it’s possible for thyroid medication to make insulin resistance (and blood sugar) worse but it’s also possible for thyroid medication to improve your blood sugar.
It all depends on your dose.

If you take too much thyroid medication, in any form, and you become hyperthyroid, then you may raise your blood sugar and make insulin resistance worse.
As insulin resistance worsens, you may also find that you gain weight!
This doesn’t always make sense to thyroid patients because they often want to increase their dose because they want to try to lose more weight.
But it doesn’t always work out that way.
Sometimes taking too much thyroid hormone can lead to weight gain. It’s rare but it does occur.
On the flip side, not taking enough thyroid hormone can also lead to insulin resistance and weight gain.
Being underdosed is typically more common than being overdosed though but it is not uncommon for some patients to be both underdosed and overdosed at various times during their treatment.
Being underdosed generally leads to persistently high blood sugar (and insulin resistance (9)) and the inability to lose weight.
When it comes to being underdosed, the right type of thyroid medication can often make all of the difference.
Often this means using a combination of both T4 and T3 thyroid medications instead of just isolated T4 like levothyroxine.
Medications such as Cytomel and Armour thyroid, for instance, contain the more active thyroid hormone T3.
Using these medications provide more oomph to your thyroid medication dose and may make all of the difference in both how you feel and how well your thyroid is managed.
Cortisol, Blood Sugar & Thyroid Function
The connection between your thyroid and blood sugar goes even deeper than what we’ve discussed so far.
Going deeper, we also see a connection between thyroid function, stress, and blood sugar.
Before we talk about this, let’s do a quick recap of what we’ve already discussed:
So far we know that both hypothyroid and hyperthyroid states can lead to high blood sugar.
We also know that medications that impact thyroid hormone levels can also impact blood sugar.
Thyroid medications such as levothyroxine or Cytomel must be dosed correctly if you want to have normal blood sugar.
Antithyroid medications like methimazole can also result in insulin resistance and high blood sugar due to their impact on thyroid function.
Any medication which impacts your thyroid will have an impact on your blood sugar. Period.
The degree of that impact will depend on the dose and therapeutic strength of the medication you are taking.
But there’s another factor that can impact blood sugar in hypothyroid patients as well.
And that is cortisol.
We know that there is a strong connection between thyroid function and cortisol levels.
Physiologic studies have shown that as cortisol rises it also tends to bring up TSH levels (10).
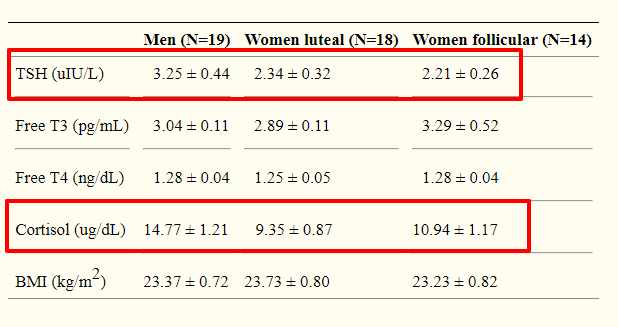
For those who may not understand the TSH lab test, a rising TSH is an indication of low thyroid function or hypothyroidism.
In other words, high cortisol causes low thyroid function.
So now we have a system that looks like this:
Stress causes decreased thyroid function which causes increased insulin resistance which causes increased blood sugar which causes weight gain and weight loss resistance.
And it doesn’t stop there.
We also know that stress by itself causes the release of blood sugar and excess stress can lead to insulin resistance on its own (11).
Because of this, it’s probably more important for you to manage stress than it is to focus on your thyroid if you have a thyroid problem.
Focusing on your stress and cortisol levels will impact both thyroid function and blood sugar and give you more bang for your buck.
Excessive stress tends to lead to issues with cortisol levels (which can be tested for, by the way) and typically manifests as increased belly fat.
In contrast, the weight gain for decreased thyroid function tends to be uniform over the entire body.
The distribution of weight gain in your body can sometimes provide valuable information about the status of your hormones.
The bottom line?
Because of the connection between cortisol, thyroid, and insulin resistance, you should always make sure to test your cortisol if you have any sort of thyroid problem.
Addressing stress and cortisol will allow you to influence your weight, thyroid, and blood sugar levels simultaneously.
The Impact of your Diet on Blood Sugar
Another area that is worth going into more detail is diet and its impact on blood sugar.
I touched on this in the very beginning but we will revisit it here.
When most people think about high blood sugar they often think immediately of the food that they put in their mouth (12).
It just makes sense that if you eat a lot of sugar, you will see that consumption of sugar is reflected in your blood and body.
Imagine consuming a 44-ounce big gulp of Coke or Pepsi loaded with high fructose corn syrup.
All of that sugar is going to be rapidly absorbed into your body and trigger the release of insulin, as we’ve discussed previously.
This example makes a lot of sense because we are talking about rapidly absorbed sugars in liquids.
But there are other foods that are high in sugar that can stimulate the same response.
Starchy foods, potatoes, fruits, etc. can all be absorbed and stimulate the insulin response as well.
The main difference between these foods and the big gulp example is the rate of absorption and how this rate impacts the rise of insulin levels from the pancreas (13).
Because of this, healthy whole foods are nowhere near as stimulatory to insulin as foods with added sugars such as those in the big gulp example.
Having said that, it is still possible to consume too much of a good thing even whole foods.
Excessive consumption of whole foods high in sugar, especially when combined with high fats, can exacerbate and contribute to insulin resistance.
I’ve found that it’s generally safe for most people to consume whole foods which are high in ‘sugar’ if they aren’t also consuming them with fatty foods (even healthy fats (14)).
Proteins have also been shown to stimulate the insulin response.
The only macromolecule which has the smallest impact on insulin by itself is fat.
Because of this, many doctors and providers have started recommending diets that are very high in fat as a treatment for high blood sugar and insulin resistance.
In fact, you’ve probably tried these diets before if you’ve been on the ketogenic diet or the carnivore diet which happen to be popular at the time of this writing.
Even though this approach makes logical sense, there’s one big problem:
It doesn’t always work!
There are plenty of people who go on ketogenic diets and high fat & low carbohydrate diets and yet they still struggle with high blood sugar and weight gain.
This just highlights the fact that we need to better understand the relationship between blood sugar and insulin.
The ketogenic diet, for instance, may have a suppressive effect on thyroid function which may counteract the benefits of this type of diet in some people.
My opinion is that there are other factors outside of just your diet that contribute to weight gain and insulin resistance such as subclinical thyroid dysfunction and cortisol dysregulation (as we’ve discussed above).
Treating Insulin Resistance if you have Hypothyroidism
So, what are you supposed to do if you have high blood sugar and hypothyroidism and you want to treat it?
What if you want to treat insulin resistance to help you lose weight?
There are several strategies that you can take and I’ve listed several below:
- Optimize your thyroid medication – What I mean here is that you need to make sure that your thyroid medication is optimized for your body. For most of you, that means you will probably need to take more medication than you are taking right now. For some that may mean lowering your dose. When optimizing your medication for blood sugar, you’ll want to focus less on the TSH and more on your free thyroid hormones (free T3 and free t4). As you optimize both of these numbers you will probably find that your blood sugar will drop naturally (as well as your weight). Avoid increasing these numbers outside of the reference range while trying to optimize them in the top percentile of the “normal” range. You can learn more about this concept here.
- Take insulin-sensitizing supplements – There are several supplements (which are available over the counter) that you can take in conjunction with all of the therapies I’ve listed here, that can help improve your blood sugar. Some of my favorites include Berberine, fish oil, Alpha lipoic acid, glucomannan, and chromium. These supplements all have scientific studies which show that they are effective at reducing both blood sugar and insulin resistance. And the best part is that they can be taken or used in conjunction with medications and other lifestyle modifications.
- Take insulin-sensitizing medications – If you really want to kick things up a notch you can also try the use of insulin-sensitizing medications. These medications are particularly useful if you are struggling with weight loss resistance which you believe is secondary to insulin resistance/high blood sugar. These medications can be used temporarily (to reverse the condition) and don’t necessarily have to be taken long-term for you to realize their benefits. Medications that fit into this category include Victoza, Saxenda, SGLT-2 inhibitors, and metformin. There are others, but these should serve as a good starting point. Victoza and Saxenda are quite expensive if insurance doesn’t cover them while metformin is incredibly cheap at around $4.00 per month. The downside to using Metformin is that it’s not quite as effective as the others, but it’s a great medication to use in many people. Metformin (and the others) can also be used in conjunction with supplements with may enhance their potency and effects!
- Exercise correctly – We didn’t talk much about exercise in this post, but it’s certainly an important aspect if you are trying to lower your blood sugar. Exercises that put a temporary high strain on the body over a short period of time tend to be best at improving insulin sensitivity. Exercises that fit into the high-intensity interval training spectrum are often ideal. The good news is that you don’t need to spend hours on a treadmill but the bad news is you will need to push yourself to get results.
- Clean up your diet – Another thing you’ll want to do no matter which therapies you use is adjust your diet. Taking all the supplements, medications, and thyroid hormones in the world will not be enough to counteract the negative effects of a bad diet. Most people know what ‘healthy’ foods are, they just have a hard time sticking to them. For those who aren’t sure where to start, look at diets that are high in real, whole foods. From there you can then start to tweak macromolecules such as protein, carbohydrates, and fats as needed.
- Consider other medications such as LDN – Lastly, some other medications can also be used to help sensitive your body to insulin. Medications like LDN (low dose naltrexone) can also potentially help autoimmune disease states such as Hashimoto’s thyroiditis (a major cause of hypothyroidism). These medications are often prescribed off-label though, so you may need a willing physician to help you out.
As you consider these therapies keep in mind that the more therapies you add on top of each other the more likely you are to see your desired results.
That means you’ll want to simultaneously change your diet, take the right supplements, adjust your thyroid medication, exercise with enough intensity, and consider the use of medications for the best results.
Final Thoughts
While it is true that hypothyroidism can lead to high blood sugar, the connection between the two is not just that simple.
There is a range of competing factors that can also contribute to high blood sugar in hypothyroid patients which should be evaluated and addressed.
The good news is that you can lower your blood sugar by taking several steps such as adjusting your thyroid medication, taking supplements, and improving your lifestyle.
Lastly, never forget the connection between stress, your thyroid, and your blood sugar.
Many people out there right now are probably suffering from a combination of all 3 while not even realizing it.
If you haven’t already, I would encourage you to look at adrenal adaptogens as a treatment for stress management.
These adaptogens have the potential to improve your energy levels, improve thyroid function, and help improve other hormone systems in your body.
I have yet to meet a thyroid patient that didn’t need them!
Now I want to hear from you:
Do you have hypothyroidism?
Do you also have high blood sugar?
What have you done to try and treat this problem? Did it work?
Do you feel that stress is contributing to your situation?
Are you planning on trying any of the treatments listed above?
Leave your comments or questions below!








