Hashimoto’s symptoms can vary drastically from person to person.
Couple that with the fact that the symptoms of Hashimoto’s disease change through time and can “flare” due to certain triggers making the disease even more difficult to diagnose and manage.
It turns out that your symptoms may be telling you something about your body and can help you determine the source and cause of your Hashimoto’s disease.
Managing and treating the autoimmunity and inflammatory aspect of Hashimoto’s is critical for reducing these symptoms.
Let’s dive in:
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Progression of Symptoms in Hashimoto’s Patients
Hashimoto’s and autoimmune thyroiditis should be differentiated from other causes of hypothyroidism.
Why?
Because autoimmune thyroiditis should be treated differently.
While it’s true that some patients with Hashimoto’s and autoimmune thyroiditis may need thyroid hormone replacement, this statement is not true for ALL patients with this disease.
Instead of focusing on the thyroid hormones and values, your focus should instead be on the autoimmunity and inflammatory component.
Autoimmunity indicates a deeper problem in the body.
The inability to recognize self from non-self, and an imbalance in the immune system.
This component is usually triggered by various factors (usually a combination of factors that we will discuss later) that results in the dysregulation of this system.

Physiologically this causes a variety of symptoms ranging from general and diffuse non-specific symptoms to alternating symptoms of both hypothyroidism and hyperthyroidism.
These issues result in a disease that can be both difficult to diagnose and manage (unless your provider knows to be looking for it).
In fact, many patients with hypothyroidism likely have some component of autoimmune thyroiditis – they just have never been diagnosed.
- Bottom line: The symptoms of Hashimoto’s and autoimmune thyroiditis differ from hypothyroidism due to both the inflammatory and autoimmune components of this disease. These two factors change how Hashimoto’s should be managed.
Fluctuations in TSH and T4 Over Time
Many of the symptoms of Hashimoto’s can be traced back to 2 main areas:
- Changes and fluctuations in thyroid hormone
- Fluctuations in inflammatory markers
We will talk about both and how they can impact your symptoms:
You can see an example below of how both TSH and FT4 can fluctuate throughout time:
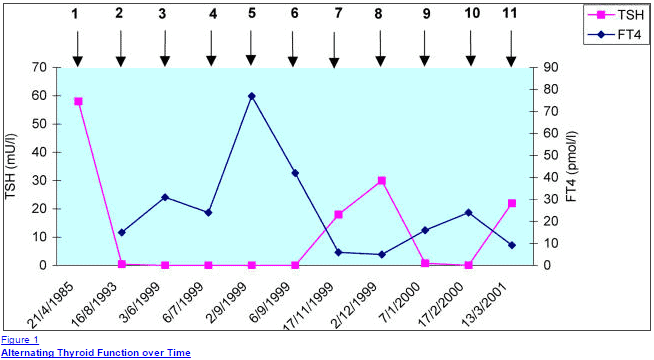
The blue line represents FT4 which you can see varies as much as 6 times between laboratory results.
The FT4 level tends to be inversely proportional to the TSH (meaning as FT4 level increases the TSH level decreases).
The TSH in the pink line varies from episodes of hypothyroidism (high levels of TSH) to nearly suppressed levels (episodes of hyperthyroidism) throughout time.
This variance in thyroid hormone levels can often trick both patients and providers which results in constant changes to thyroid hormone and various symptoms in the patient.
When in reality the focus should be on the autoimmune and inflammatory components and NOT the thyroid hormone themselves.
It’s easy to see how thyroid hormone levels directly impact your symptoms so we will move to the second factor which is changes in your inflammatory markers.
Inflammatory changes cause a variety of symptoms related to your thyroid and related to other hormone systems in the body.
Inflammation by itself can cause a reduction in T4 to T3 conversion (1) (leading to worsening symptoms of hypothyroidism).
Inflammation can also potentiate insulin resistance (2) and make adrenal function worse.
These changes may lead to symptoms such as weight gain (3), fatigue, and neurological symptoms that may complicate or worsen existing hypothyroid/hyperthyroid-like symptoms.
Your inflammatory status can be measured and tracked by checking non-specific markers in the blood including:
- Erythrocyte sedimentation rate (ESR)
- C reactive protein (CRP)
- Ferritin
- Thyroid antibodies and other antibody levels
The elevation of these markers (while not specific) indicates dysfunction in the body and may make the symptoms of Hashimoto’s worse.
Now let’s discuss how these two component changes and alter the progression of the symptoms of Hashimoto’s over time…
- Bottom line: The combination of inflammation and autoimmunity cause variations in thyroid function and other hormone function in the body. This is part of the reason that this disease causes symptoms to change over time.
Generalized and non-specific symptoms -> Symptoms start here
The symptoms of Hashimoto’s usually start out as minor diffuse fatigue.
Because of these symptoms, it can be difficult to pinpoint where your symptoms are coming from.
You may present with a mild weight gain of 5-10 pounds, or maybe just some mild fatigue.
The issue is that most patients know that something is “off” in their body, but when they go to their physician they usually undergo “standard” lab tests that don’t identify the problem.
Or worse, the provider will identify the presence of antibodies like anti-TPO thyroid antibodies but take the “wait and see” approach to management.
The symptoms generally start out somewhat mild due to the low-grade inflammation and autoimmunity that is present.

At this point there isn’t usually significant damage to the thyroid gland, so most damage at this point is reversible if treated correctly.
It also means that undergoing treatment at this point is critical.
Because any treatment you can do to help lower the inflammation and autoimmunity will go a long way to helping reduce long-term thyroid damage and reliance upon thyroid hormone later in life.
How Hashimoto’s symptoms start:
- General fatigue or sensation of being “run-down”
- Mild weight gain(usually 5-10 pounds)
- Flat affect or depressed mood, not feeling like yourself
- Mild difficulty with concentration or inability to focus
- Dry skin, cracked lips, dry & brittle hair, non-specific rashes or patches on the skin
- Mild constipation
- Mild fluid retention(especially in the face and lower extremities)
- Voice hoarseness or sensation of a “swollen throat”
- Reduction in sweating or inability to sweat
- Mild joint pain or muscle aches
- Mild to moderate changes to the menstrual cycle including irregular cycle and/or reduced/increased flow
If you are experiencing any of the symptoms listed below make sure to get your antibody levels checked, and not only that but continue to follow them as you undergo treatment.
This will help to determine if you are on the right track.
This is only the start of the symptoms of Hashimoto’s however, and symptoms may fluctuate between hyperthyroidism and hypothyroidism which I will go over below.
- Bottom line: The initial symptoms of Hashimoto’s tend to be vague and diffuse making the diagnosis difficult. Treatment at this early stage is critical, however, because you can prevent long-term reliance upon thyroid hormone later in life if you can stop the damage early.
Progression through hyperthyroidism and hypothyroidism
Many patients, unfortunately, can go years (or decades) without a diagnosis of Hashimoto’s or autoimmune thyroiditis.
During this time some patients will experience swings or episodes of hyperthyroidism followed by episodes of hypothyroidism.
This can occur as a result of the damage done to the thyroid gland by thyroid antibodies.
As antibodies attach to the thyroid gland your body will react in turn with an inflammatory response that may damage or injure the thyroid gland.
The thyroid as a gland has the job to release hormones under a stimulus. And this stimulus can be triggered by the damage and cause a “flush” of thyroid hormones to be released from the body.
This flush can temporarily trigger symptoms of hyperthyroidism which can make symptoms worse (especially if the patient is already on thyroid medication).
Symptoms that mimic episodes of hyperthyroidism or a “flush” of thyroid hormones in the bloodstream/body:
- Hot flashes or episodes of heat intolerance
- Mood changes, typically on the anxiety spectrum
- Jittery sensation or sensation of “too much energy”
- Fatigue or episodes of energy swings(up and down)
- Difficulty sleeping or episodes of insomnia
- Facial flushing or sensation of warm extremities
- Heart palpitations or sensation of a racing pulse(usually episodic and at night but can occur at any time throughout the day)
- Weight loss/weight gain accompanied by changes in appetite
These symptoms do not occur in every patient, however.
Some patients just have a chronic and continuing decline in thyroid hormone throughout time, but some experience these episodes of “ups” and “downs”.
It’s important to realize that the presence of these symptoms may also indicate antibodies that directly stimulate the release of thyroid hormone from the body (it isn’t always caused just by the inflammatory component).
- Bottom line: The inflammatory component of Hashimoto’s may trigger a “flush” or release of thyroid hormones into the bloodstream which may manifest as hyperthyroid-like symptoms. During these episodes, your free thyroid hormones will be elevated and your TSH will drop.
Overt Hypothyroidism
Over time, if not treated, most patients will eventually develop symptoms of hypothyroidism.
As antibodies remain elevated (and untreated) in the blood for long periods of time, thyroid glandular damage (4) will accumulate.
Once this point reaches critical mass you will eventually lose endogenous production of thyroid hormone.
This is usually the point where your symptoms progress and continue to worsen all of a sudden over a 1-2 year period.
Once patients get to this stage they may ultimately require lifelong use of thyroid hormone replacement due to this glandular damage.
The symptoms experienced at this stage generally mimic hypothyroidism but many patients still have lingering “general and diffuse” symptoms from the autoimmune component.
Hypothyroid symptoms due to glandular damage in Hashimoto’s patients:
- Extreme fatigue and/or exhaustion
- Moderate weight gain (20-30+ pounds usually gained over a 6-12 month period)
- Hair loss, hair thinning, and/or hair breakage
- Changes to mood, usually on the depression spectrum
- Menstrual irregularities and other conditions like PMS/PMDD
- Chronic and debilitating muscular and/or joint pain
- Chronic and daily constipation, development of other GI issues like gas/bloating, acid reflux, low stomach acid, and SIBO/SIFO
- + any other generalized symptoms above
- Bottom line: Once the damage has accumulated the thyroid may become permanently damaged leading to reliance upon thyroid hormone replacement. These symptoms generally match symptoms of hypothyroidism from other causes.
Symptoms of Hashimoto’s Flare-up
At some point in time, you may also experience what I refer to as a Hashimoto’s “flare-up”.
These flare-ups usually result from some sort of “trigger”.
We’ve already discussed how the immune system and inflammatory cascade in your body are dysregulated when you have Hashimoto’s or autoimmune thyroiditis in the previous section but what we didn’t talk about is how sensitive the immune system really is.
Due to these problems, your immune system is hyperexcitable.
Meaning that small changes may result in a cascade effect causing multiple downstream effects.
This cascade is usually responsible for the symptoms of a “flare-up”.
Symptoms of a Hashimoto’s flare-up include:
- Abrupt worsening of fatigue
- Usually weight gain from an unclear source without changing your diet or food intake(rarely some patients do experience some weight loss)
- A general feeling of weakness or malaise
- Abrupt worsening of joint pain/muscular pain
- Racing heart, jittery sensation, or feeling an uncomfortable “rush”
- Abrupt onset of brain fog, difficulty concentrating, or inability to focus on difficult tasks
- Changes to GI function
- Some patients may experience acute symptoms of Hyperthyroidism(see list above)
- Some patients may experience acute symptoms of Hypothyroidism(see list above)
While flare-ups may differ dramatically from person to person, it’s important not to focus on the symptoms necessarily but instead on what they mean for your body.
During a “flareup” both your immune system and inflammatory system have been triggered and you may be damaging your thyroid.
It’s important to find the eliminate the cause of whatever triggered this event.
Manage flare-ups by managing inflammation and finding the source
Since finding the source of the flare-up is so critical I’ve included several possible factors that can all influence Hashimoto’s symptoms and trigger a “flare-up”.
List of Hashimoto’s flare-up sources:
- Extreme physiological or emotional stress (5) (death of a loved one, divorce, problems at home/school/work, etc.)
- Physical trauma such as car accidents or even repetitive physical trauma from extreme exercise/sports
- Chronic nutrient deficiencies (6)
- Viral infections (7) (CMV, EBV, etc.)
- Other hormone imbalances that may alter immune system function
- Exposure to endocrine-disrupting chemicals (8) (see list below)
- Exposure to heavy metals (9) (the removal of dental amalgams has been shown to reduce thyroid antibodies in some patients)
- Increased intestinal permeability (10) due to overgrowth syndromes or intestinal dysbiosis
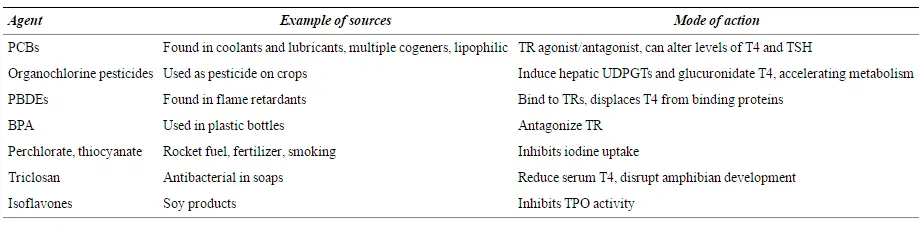

You will notice that many of these sources of flare-ups can also be potential triggers of the autoimmune disease itself.
This makes sense because you can trigger Hashimoto’s with emotional stress and then make the disease worse by introducing another trigger/flare-up source.
For these reasons I always recommend that patients take a comprehensive approach to managing their Hashimoto’s to eliminate the increased risk of making their disease worse.
If you focus on and treat multiple problems at once then your results will be better and you will have less risk for a flare-up.
You can find information on how to reduce your antibody levels here, and you can find more information on how to manage other triggers of Hashimoto’s in this post.
Recap & Final Thoughts
Hashimoto’s disease should be differentiated from other causes of hypothyroidism because of the inflammatory and autoimmune component that accompanies it.
Addressing both of these components is required for optimal treatment.
On the other hand, the symptoms of Hashimoto’s tend to differ drastically from other causes of hypothyroidism from these components as well.
This results in various symptoms ranging from diffuse and generalized symptoms to “flushes” of thyroid hormone causing hyperthyroidism and ultimately hypothyroidism if the disease progresses enough.
Some patients will also experience flares throughout the course of their disease which can be managed by eliminating the source.
Now it’s your turn:
Do you have Hashimoto’s or autoimmune thyroiditis?
Do your symptoms follow the “textbook”?
Have you experienced a flare before? If so what were your symptoms?
Leave your comments below!