Have you been told, or are you suspicious, that you have a high TSH?
If so there are many things you want to consider before pursuing treatment.
While your TSH is important for assessing thyroid function it’s certainly not the only test, or the best way, to identify thyroid disease.
We are going to take an updated, scientific dive into TSH including what a high TSH means, what kind of symptoms are associated with this condition, and the top 5 causes…
What does your TSH Really Mean?
Many physicians consider TSH to be the most accurate marker of thyroid status in your body.
With that in mind, it makes sense to talk about what it actually does in your body.
TSH stands for thyroid-stimulating hormone and it is a hormone secreted by your pituitary gland.
Thyroid physiology is quite complex (1) but we can break it down into an easy-to-understand sequence:
Your hypothalamus (part of your brain) pumps out a hormone called TRH (thyrotropin-releasing hormone).

TRH then acts on your pituitary gland (another portion of your brain) to stimulate the release of TSH (thyroid-stimulating hormone).
TSH then enters your bloodstream and lands on receptors directly on your thyroid gland which then causes the release of thyroid hormones – T3 and T4.
T3 and T4 then enter the bloodstream and target specific cells in the body (almost every cell has a thyroid receptor) to alter genetic transcription, increase energy production, and so forth.
This complex system is regulated at several steps and one step that we use to assess the stability of this entire system is the serum concentration of TSH.
This isn’t the best marker of thyroid function by itself (2), but it can give you a quick idea of what is happening in the body.
So what does a high TSH actually mean?
An elevation in TSH is an indicator that the system is not working properly, and in this case, it means that thyroid function in the serum (T3 and T4) is low.
Low levels of T3 and T4 circulate back up to the pituitary gland which tells the body that not enough thyroid hormone is being produced.
Your pituitary gland compensates by increasing TSH levels in the serum because it is trying to tell your thyroid gland to produce more thyroid hormone.
Hopefully, this is making sense.
It can be confusing because a high TSH level actually means that there is not ENOUGH thyroid hormone in the blood and this condition is known as hypothyroidism.
Hypothyroidism = low thyroid function = sluggish thyroid = low T3 and T4 levels of thyroid hormone in the blood = high TSH (all of these terms are ways to describe the same condition).
The exact opposite is true when the TSH is low.
A low TSH is an indicator that your body has enough T3 and T4 in the body and so your pituitary responds by reducing the production of TSH from the pituitary gland.
Hyperthyroidism = excessive thyroid production = high T3 and/or T4 levels of thyroid hormone in the blood = low TSH.
This isn’t the complete picture because certain medications can actually reduce TSH but still leave T3 and T4 levels low in the body, but it gives you a general idea of what is actually happening in the body and what your TSH actually stands for.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
So How do Doctors Use TSH?
TSH is primarily used as a marker of thyroid hormone status in the entire body.
Checking your TSH can be used as a quick measure to determine if your thyroid is functioning properly or not.
A high TSH (defined below) tells your Doctor that your thyroid is not working properly which means that you may need the use of thyroid hormone medications to increase and normalize thyroid function.
After starting thyroid medication (if necessary) the TSH can be used to “track” your progress.
As you take thyroid medication your TSH should be reduced back to the “normal” range.
As this occurs you are said to once again become “euthyroid”.
This is how everything is supposed to work, but is it really that easy?
This is where Doctors and patients tend to disagree (3).
Even though you can “normalize” the TSH with thyroid medications, many of the symptoms of hypothyroidism may actually still persist.
This, along with many studies, may indicate that TSH may not be the best marker for thyroid function in the body (4).
We will discuss more of that below, but for now, let’s discuss what kind of symptoms you may experience if your TSH is elevated.
High TSH Symptoms
As your TSH increases it is a sign that circulating levels of thyroid hormones are dropping.
Therefore, the symptoms associated with high TSH levels present as the symptoms of hypothyroidism.
Symptoms do not stem from the TSH itself but from the lack of circulating T3 and T4 and their influence on your cells.
In addition, symptom severity is dependent, at least somewhat, on the degree of elevation of TSH.
Higher levels of TSH, those greater than
The degree of elevation of your TSH will also help determine the severity of your symptoms.
People who have a TSH of 5.0 will likely experience symptoms that aren’t quite as severe as someone who has a TSH of 7.0 or higher.
You can find a list of the symptoms that one might experience with a high TSH below:
- Weight gain or difficulty losing weight (the degree of weight gain and inability to lose weight depends on the severity of thyroid lab studies)
- Fatigue or decreased energy
- Insomnia or inability to sleep
- Changes to the menstrual cycle or changes to sex hormones (reduced testosterone in both men and women and changes to progesterone/estradiol in women)
- Drop in body temperature – cold hands/feet
- Slower than normal metabolism
- Changes to skin that include dry or cracking of the skin
- Changes to hair, skin, and nail quality and texture – brittle hair, dry hair, hair loss, etc.
- Slowing down of the intestines which manifests as constipation or acid reflux
- Mental changes to include depression, anxiety, poor concentration or poor memory
- Swelling of the face or extremities (puffy eyes)
Why are these symptoms important?
Symptoms reduction, along with TSH, can also be used as a marker to determine if your therapy or treatment is working.
If you take medication to lower your TSH and your TSH lowers but your symptoms remain, then there may be another issue you are missing.
You can find a more complete list of thyroid symptoms that women may experience in this post and a complete list of thyroid symptoms that men experience in this post.
Definition of a “High” TSH (Reference Ranges)
So what defines a “high” TSH?
By definition, the standard reference range for TSH is anywhere between 0.30 to 5.0 uIU/mL.
If your TSH is higher than 5.0 then the lab will flag you as “high” and you may experience the symptoms listed above.
You can see a clear example of this below:

The reference range in this example is 0.3 to 5.00 uIU/ml and the result is 7.024.
Having said all of this, there’s actually a good case to make that you can still have a “high” TSH but still be inside of the reference range.
So how do we get there?
Well, newer studies (5) have shed light on the fact that some of the original tests that helped determine our “standard normal” TSH values may not have been full of “healthy” people.
When you are being compared to some standard you want to make sure that the standard you are being compared to is actually healthy!
It doesn’t make sense to compare your TSH as a 25-year-old to that of an 86-year-old (6).
Using this logic some newer studies have suggested that a more “normal” TSH reference range is somewhere between 1.0 and 2.5 uIU/ml and anything higher than 2.5 is considered “high” (7).
With this logic you can have a “high” TSH anywhere between 2.5 and 5.5, even though it technically falls within the “normal” range:
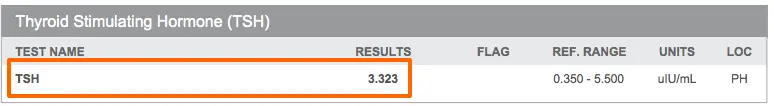
In addition, other studies have suggested we use the African American population as the standard for TSH testing because they have one of the lowest rates of autoimmune disease compared to other populations and their TSH is somewhere around 1.0.
It’s important to realize that many physicians are not aware of these studies or these concepts so they may use the “standard” laboratory reference range instead of these newer guidelines.

5 Causes of High TSH
Having a high TSH is never normal.
An elevated TSH (as defined by the reference ranges listed above) is an indication that your body is working overtime to try and increase the amount of thyroid hormone that it can produce.
In most cases, your TSH is simply a warning sign that indicates your body is under stress and increased pressure.
While knowing that your TSH is elevated is important, your TSH itself does not tell you WHY it is increased.
That’s why it’s important to understand the potential causes because each of these causes has a different treatment.
#1. Hashimoto’s Thyroiditis
Probably the most common cause of slightly elevated and high TSH levels is an autoimmune disease known as Hashimoto’s Thyroiditis.
It is estimated that anywhere between 50% and 90% of all cases of hypothyroidism may be caused by this condition in the United States.
Hashimoto’s thyroiditis is a condition where your body begins to attack its own thyroid gland, through an autoimmune process, which results in long-term and potentially permanent damage to your thyroid gland over time (8).
As your thyroid gland becomes damaged the amount of thyroid hormone it produces will be reduced over time.

As this happens your pituitary compensates by increasing TSH levels slowly over time.
In a sense, it’s like trying to squeeze water out of a rock.
How can your thyroid gland produce thyroid hormone if it is permanently damaged?
It can’t.
The good news is that diagnosing Hashimoto’s thyroiditis is not very difficult and can be assessed by checking for thyroid antibodies in the serum.
The presence of clinical thyroid damage (symptoms) combined with elevated antibodies is sufficient to diagnose the disease.
Your Doctor should know to check for the following antibodies:
- Thyroid Peroxidase antibodies (9)
- Thyroglobulin antibodies
If they are contributing to your TSH then your labs may look something like the example listed below:

Identifying that you have Hashimoto’s is important because it means you may be able to influence the course of the disease and reduce the autoimmune damage if you take steps as soon as possible.
Note, though, that in some cases by the time the diagnosis is made it may be too late – there may already be permanent damage to your thyroid gland, especially if the autoimmune process has been going on for decades.
You can learn more about treating, identifying, and managing Hashimoto’s in this post.
#2. Iodine Deficiency
While overt iodine deficiency is no longer a huge issue in the United States, many people may still have what I refer to as “sub-optimal” iodine levels.
The main method by which we get iodine is through our diets, but unfortunately, many factors may be influencing how much we actually get.
For starters, many people simply aren’t consuming enough iodine because they don’t consume sea vegetables regularly.
This is worsened by the fact that the iodine concentration in the soil is dropping as well, so foods that would normally contain iodine may vary in their concentration.
In addition, other factors such as the lack of utilization (from goitrogens) in certain foods may limit the activity of iodine that you do consume.
Taking this one step further…
Studies have shown that the average person should be consuming 150 ug of iodine per day (up to 250-290 if you are lactating or pregnant) (10), while other studies show that the average consumption varies between 120-130 ug per day (11).

You can compare this to the 1970s when the average consumption of iodine was up to 294 ug/day.

Putting all this together you can make a case that many people simply may not be getting sufficient iodine even though we live in an iodine “replete” environment.
How does this impact TSH?
Iodine is required for the production of thyroid hormone in your body (12).
Therefore, low iodine will result in low circulating thyroid hormone in the serum.
This will trigger a feedback loop which will result in an increase in TSH from your pituitary.
Low iodine = high TSH.
The good news is that replacing iodine through dietary means will rapidly result in an improvement in your thyroid function.
You can learn more about using iodine safely and correctly in this detailed guide.
#3. Obesity & Metabolic Damage
Most people assume that hypothyroidism (low thyroid function) causes obesity, but what they don’t realize is that obesity can actually decrease thyroid function as well.
The cause vs effect has not been settled but we will most likely find that while hypothyroidism can cause obesity, obesity can also reduce thyroid function and increase TSH.
Why does this matter?
For starters, it means that if obesity is the cause of low thyroid function (and therefore an elevated TSH) it means that if you lose weight you will improve your thyroid status.
And this is what studies have shown.
As you lose weight TSH tends to drop and FT3 and FT4 levels tend to normalize (13).
Another important implication of the obesity-thyroid connection is that due to the widespread increase in obesity we may need to alter TSH reference ranges (14).
Our current understanding of obesity and thyroid function is that obesity is the RESULT of hypothyroidism.
But if obesity causes hypothyroidism then that means we need to create a “normal” TSH based on the reference ranges of people that have normal body weight and who do NOT have Hashimoto’s thyroiditis.
This may impact our definition of the “ideal” or “normal” TSH.
Moral of the story?
Obesity, weight gain, and metabolic damage may all potentially increase your TSH and lead to hypothyroidism.
#4. Stress & Increased Cortisol
Another important cause of high TSH is stress and increased cortisol.
Cortisol is considered our stress hormone which is released to help our body “tolerate” excessively stressful situations.
Stressful situations range from lack of sleep to social pressure from jobs and back to the food we put in our bodies.
The idea here is that all of these factors influence this stress hormone and may result in chronic elevations in serum cortisol.
High cortisol is positively correlated with TSH levels in the serum (15).
This means that as cortisol increases so too does TSH.
What isn’t clear is whether or not this relationship is physiologic or pathologic.
In my experience, I tend to lean more toward the pathologic side as patients with both high TSH and high cortisol exhibit higher rates of depression, anxiety, and poor cognitive function.
These symptoms lead me to believe that stress, excessive stress which is chronic in nature, most likely results in an increased TSH which reduces thyroid function in the body.
The treatment for this condition is to focus on limiting the impact that stress has on your physiology by taking targeted supplements and practicing specific therapies.
You can learn more about addressing cortisol to improve thyroid function here.
#5. Thyroidectomy (Partial or Complete) & RAI
Next up is really any condition that results in damage or removal of your thyroid gland.
It makes sense that if you damage your thyroid gland or completely remove it that you won’t be producing as much thyroid hormone as you were before.
Most people who undergo complete thyroidectomy (meaning complete removal of their thyroid gland) are given thyroid medication right away.
The same is not necessarily true for those who have only had a portion or partial thyroidectomy (partial removal of their thyroid gland).
Patients who undergo RAI or radioactive iodine ablation therapy may also still have some thyroid gland function, but this function may not be sufficient to provide adequate thyroid hormone to the entire body.
In both cases, these patients may still have somewhat “normal” thyroid lab studies but tend to present with MANY of the symptoms of hypothyroidism.
The bottom line?
Damage to your thyroid gland or removal of your thyroid gland (16) (even part of it) may result in an increase in TSH levels.
The treatment for patients in cases such as these is the replacement of thyroid hormone with thyroid hormone medication.
Treatment Options
If you have a high or high-normal TSH then your next step should be to focus on ways to bring it down.
This can be accomplished by focusing on several areas:
#1. Using thyroid hormone replacement medication.
Using thyroid hormones will help to reduce your TSH due to the feedback loops that exist in your body.
Remember:
As you put thyroid hormone into your body, your brain will “sense” this thyroid hormone and respond by normalizing your TSH.
This will result in a reduction in your TSH, provided that the dose of thyroid medication that you are taking is sufficient for your needs.
This is exactly how many Doctors use the TSH to help guide their treatment.
The idea is to bring down your TSH to a “normal” level based on your lab results and to stop the titration of medication once you get there.
This sounds fairly easy, but it doesn’t quite work this way in all patients.
Some people will feel great as they take thyroid medication such as Levothyroxine to help lower their TSH.
In other people, it may not be quite that simple.
Up to 15% of people may suffer from genetic changes in their body which limit their ability to utilize or “convert” thyroid medication appropriately.
If you have this genetic defect (which is a problem with a deiodinase enzyme) then you may not respond very well to standard thyroid medication.
This problem can be overcome through the use of different types of thyroid medications.
Even though thyroid medication may be helpful to lower TSH it may not be required in each person.
#2. Addressing the primary cause of your high TSH.
Another area of focus should be on the CAUSE of your high TSH.
As I discussed with you previously, not all causes of high TSH are permanent.
In fact, some causes, such as iodine deficiency, can completely be reversed if you treat them appropriately.
In the case of iodine deficiency, this problem can be easily treated with iodine supplementation.
In the case of stress, you may be able to improve your TSH by completely removing the stress in your body or by attempting to lower your cortisol.
Other conditions, such as Hashimoto’s thyroiditis, may be more difficult to treat because they indicate a deeper problem.
Hashimoto’s is a result of autoimmune dysfunction and is not readily reversible (at least not in the majority of cases).
#3. The use of targeted supplementation.
We’ve already established that nutrient deficiencies, such as iodine deficiency, may play a role in altering thyroid function (17).
This idea extends to more than just iodine.
Other nutrients, such as Zinc and Selenium (18), also play an important role in regulating thyroid function in your body.
One study showed that using the combination of zinc and selenium helped to reduce TSH and increase free T3 and free T4 levels in overweight female obese hypothyroid patients.
What’s really interesting is that these patients didn’t experience any increase in serum zinc or selenium levels.
The use of supplements that contain both Zinc and Selenium has been shown to improve thyroid function in those who have deficiencies.
The good news is that this is a potentially reversible cause of high TSH, the bad news is that it will probably only work if you are deficient.
But, as a potential therapy with very little downside, it’s always worth evaluating for these simple deficiencies.
Using a supplement such as this one may be beneficial and has worked well for other hypothyroid patients.
Is it Possible to Have a High TSH and Normal T3 & T4?
Yes!
In some cases, the serum T3 and T4 levels can be relatively preserved despite elevation in TSH levels.
Some people assume this is a reactive response but you must realize that serum concentrations of thyroid hormone do not necessarily reflect tissue levels of thyroid hormone.
What’s important is not the serum concentration but the amount of thyroid hormone that enters the cells and activates genetic transcription.
TSH reflects the tissue concentration of the pituitary gland, but it does not reflect the concentration of say your liver.
We can use SHBG as an indirect marker for assessing the concentration of thyroid function in the liver (19) and this can actually be used as a somewhat sensitive marker for tissue levels elsewhere in the body.
You can learn more about using the SHBG for this purpose in this guide.
Just realize for now that in order to get a “complete” picture of thyroid function in the body, you should evaluate TSH in the presence of other thyroid lab studies such as free T3, total T3, free T4, sex hormone-binding globulin, and of course thyroid antibodies.
Conclusion
A high TSH level may indicate that you have sub-optimal levels of circulating thyroid hormone in your body.
This condition is known as hypothyroidism and presents with MANY diverse symptoms.
If you find that you have a high TSH then your next step should be to look into the potential causes of the disease and treat that issue, if possible.
Treating can then be focused on several areas:
#1. Thyroid medication.
#2. The underlying cause.
#3. The use of Supplements.
This approach will ensure that you cover all of your bases and will provide you with the most relief.
You will also want to consider if thyroid medication is right for you or if taking a more conservative approach may be the best fit.
Once you start thyroid medication you may be taking it for life so you may not want to jump into it.
Lastly, when evaluating your TSH make sure that you are looking at your value with the “optimal” level in mind and not just the standard reference range.
Looking at your TSH in this way will help you get back to your 100%.
Now I want to hear from you:
Is your TSH high?
If so, have you been able to find appropriate treatment?
If not, why not?
Leave your comments below!









