Hashimoto’s is the number 1 cause of hypothyroidism in the US and developed countries.
And while that statistic is interesting, there’s something much more interesting about Hashimoto’s…
The fact that many people who have Hashimoto’s have no idea that they do.
And it’s not because Hashimoto’s is a hard condition to diagnose.
Quite the opposite actually.
Because Hashimoto’s is an autoimmune disease, you can test for thyroid antibodies in the bloodstream.
The two thyroid antibodies associated with this condition include thyroglobulin antibody and thyroid-peroxidase antibody.
For most people, it’s as easy as checking your bloodstream for these two antibodies.
If they come back positive AND you have thyroid problems you are officially diagnosed with Hashimoto’s.
Sounds pretty easy, right?
Well, yes and no.
Despite how easy it is to diagnose Hashimoto’s, many doctors fail to order the antibody tests which leaves many patients diagnosed with a thyroid problem of unknown origin/cause.
But things can get a little more complicated than this.
It turns out that as many as 5-10% of people with Hashimoto’s have NEGATIVE thyroid antibodies in their bloodstream.
And yet, these people still have all of the signs and symptoms, including thyroid gland inflammation, of Hashimoto’s.
What gives?
There are at least 2 medical conditions in which you can have NEGATIVE thyroid antibodies but still have Hashimoto’s.
And it’s very important for you to understand if you have either of these conditions because if you don’t, you may never get the correct diagnosis.
Before you walk away thinking that it doesn’t matter whether you know if you have Hashimoto’s, let me address that as well.
There is a big difference in treatment between those with Hashimoto’s and those with regular run-of-the-mill hypothyroidism.
Knowing you have Hashimoto’s means that you can tailor your treatments to more than just thyroid function.
You can focus on treatments that ALSO impact your immune system.
Doing this will help you reduce the inflammation and damage to your thyroid gland and may help you prevent or reverse future damage.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Conditions that result in Negative Thyroid Antibodies
As I mentioned previously, there are at least 2 different medical conditions in which you can have Hashimoto’s thyroiditis without the presence of thyroid autoantibodies.
While it is uncommon to have Hashimoto’s and not have thyroid antibodies, these conditions are still fairly common.
It’s also unlikely that your doctor will even be thinking of these conditions and may not even be aware that they exist at all.
This means it will be up to you, as a thyroid patient, to have some basic knowledge that they exist.
You may need to advocate for some additional testing (which we will talk about below) if you strongly believe that you have Hashimoto’s in the face of negative antibodies.
With this in mind, let’s talk about the conditions associated with Hashimoto’s and negative thyroid antibodies…
#1. Seronegative Hashimoto’s Thyroiditis
The first condition is known as seronegative Hashimoto’s.
The word ‘sero’ refers to the serum, the word ‘negative’ refers to the absence of something, and ‘Hashimoto’s refers simply to the medical condition.
So we can break down the word to mean the absence of Hashimoto’s in the bloodstream (serum is another word used to describe testing in the blood).
And that’s exactly what this condition is.
People with seronegative Hashimoto’s do NOT have antibodies to thyroglobulin or thyroid-peroxidase (the typical antibodies associated with Hashimoto’s) and yet they still have Hashimoto’s.
How can this be?
Well, it’s not exactly clear but the hallmark of Hashimoto’s is inflammation and immune cell-mediated damage of the thyroid gland tissue.
And people who have seronegative Hashimoto’s do NOT have thyroid antibodies but they DO have this thyroid gland damage (which you can test for).
So clearly they have Hashimoto’s.
But, again, this is not a common occurrence among patients with Hashimoto’s.
Roughly 90% of all patients who have Hashimoto’s will have positive thyroid antibodies in their bloodstream.

This leaves the other 5-10% (depending on which study you look at) with negative antibodies but with the signs and symptoms of the disease.
5-10% is not insignificant, though, and it leaves roughly a 1 in 10 or a 1 in 20 chance that you may fall into this category.
People who have seronegative Hashimoto’s thyroiditis are often missed by both conventional doctors and even more experienced thyroid doctors/endocrinologists.
The only way to diagnose seronegative Hashimoto’s is by directly evaluating the thyroid gland with an ultrasound and doctors are not likely to order such a test unless they see thyroid gland enlargement.
Standard thyroid lab tests will not show the presence of this condition either.
While it is very difficult to diagnose, the silver lining is in the fact that it is often less severe compared to antibody-positive Hashimoto’s (1).
It is felt that those with seronegative Hashimoto’s have a less severe disease compared to those with positive antibodies.
But it’s still worth pointing out that therapies that impact immune function (including supplements, diet, stress reduction, detoxication, and so on) will still help those with seronegative Hashimoto’s.
In fact, the treatment between those with seronegative Hashimoto’s and those with antibody-positive Hashimoto’s is not any different.
#2. End-Stage Hashimoto’s Thyroiditis
There is at least one more condition that can make diagnosing Hashimoto’s difficult and that is end-stage Hashimoto’s.
People who have end-stage Hashimoto’s frequently do NOT have any antibodies present in their bloodstream, but clearly have Hashimoto’s.
But this group of people should be differentiated from those with seronegative Hashimoto’s.
Let me explain:
The standard course of Hashimoto’s (for 90% of people) is that thyroid antibodies slowly rise, reach a peak, and then eventually decline over time (2).
See this image below:
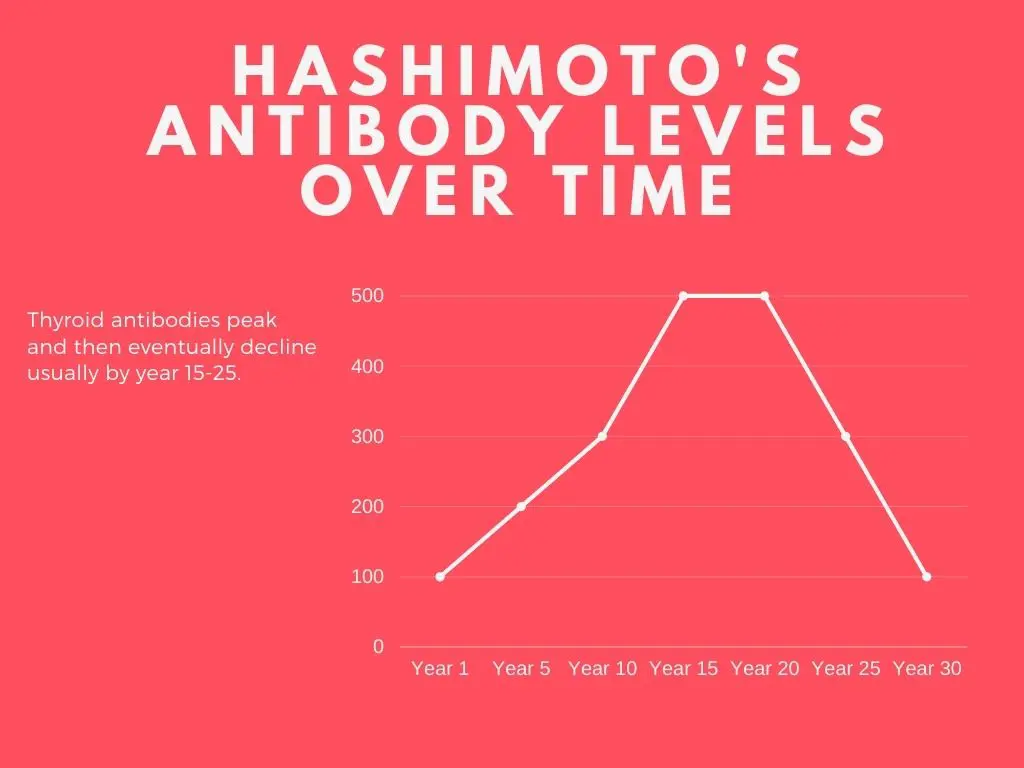
This is obviously just an illustration, but it shows what I am trying to explain.
The reason that antibody levels fall over time is due to the eventual destruction of the thyroid gland.
Your body produces thyroid antibodies designed to kill thyroid gland tissue.
Once the tissue is dead, the body no longer sees your thyroid as a threat and your antibody levels will fall.
But did your Hashimoto’s go away? Not really, it’s still there, you just don’t see the antibodies anymore.
People generally don’t miss this condition, though, because they have typically been diagnosed many years ago.
You don’t reach this end-stage until you’ve had Hashimoto’s for at least a couple of decades (usually 20+ years).
But it is still a condition in which you can have Hashimoto’s and NOT have positive antibodies so we are including it here.
How to Tell if You Have Hashimoto’s (Even if Antibodies are Negative)
I know what you are probably thinking…
“How can I test for Hashimoto’s if it won’t show up in my bloodstream?”
That’s exactly what we are going to talk about now.
There are several ways that you can identify if you have Hashimoto’s without checking for thyroid antibodies.
Looking for thyroid antibodies is obviously the easiest method, but you can’t count on it if you are one of the lucky (or unlucky, depending on how you look at it) few who have seronegative Hashimoto’s thyroiditis.
- Thyroid Ultrasound – The first and easiest way to identify Hashimoto’s is with a thyroid ultrasound. The thyroid gland is very superficial which means you can look at its shape, size, and other features using ultrasound. If Hashimoto’s is present, you will see signs of thyroid gland inflammation as well as changes to the normal volume of the thyroid gland. This usually is described as hypoechoic or dark patterns seen inside of the thyroid gland, a diffusely enlarged thyroid gland with heterogeneous echotexture, a doppler study with normal or decreased flow, and reactive cervical nodules (you might see this language on your ultrasound report (3)). In addition, you might see that your thyroid gland is enlarged (bigger than it should be) or smaller than it should be. Both can occur in Hashimoto’s and should not be seen in regular hypothyroidism. Getting a thyroid ultrasound is a very simple, non-invasive way to test for Hashimoto’s and it should be your first step if you believe you have seronegative Hashimoto’s.
- Complete thyroid lab tests – You can also look at your thyroid lab tests, and you should be getting these. And I’m not just referring to your thyroid antibodies. You can use your other thyroid lab tests (such as TSH, free T3, and free T4) to identify EARLY thyroid problems. If you find, for instance, that your TSH is normal and your thyroid antibodies are negative, but your free T4 and free T4 are low, then you might want to consider getting the thyroid ultrasound done. In this way, you can use your thyroid lab tests to help identify EARLY Hashimoto’s so you can get ahead on your treatment. The reason this is so important is that most people are not diagnosed with Hashimoto’s until they’ve had it for several years. If you check a full thyroid lab panel you may be able to diagnose your disease much earlier!
- Checking for inflammatory markers in the bloodstream – The next thing you will want to consider ordering are tests that assess for inflammation in your body. And specifically, I am talking about ESR and CRP. ESR stands for erythrocyte sedimentation rate and CRP stands for c-reactive protein. If either is positive then it’s a sign that you have inflammation in your body. This is important because regular causes of hypothyroidism are NOT associated with inflammation in the body. And remember, Hashimoto’s is first and foremost an immune disease which means that it IS associated with inflammation. If you find that you have high levels of inflammation in your body (because your CRP or ESR are elevated) AND you have thyroid problems (with negative antibodies) then it would be a good next step to get that ultrasound I talked about previously!
- Biopsy of the Thyroid Gland – Lastly, and I don’t recommend getting this done, you could always get a biopsy of the thyroid gland (4). Getting a biopsy is the gold standard for diagnosing Hashimoto’s, but it comes with a cost. When you stick a needle into your thyroid gland and pull out tissue, that tissue is gone forever. You don’t really want to cause permanent damage to your thyroid gland when you can get all of the information you need through other methods. I’ve included this option here though because sometimes it’s necessary to get a biopsy, in which case you might as well test for it, and for completeness’ sake. This should be your last option, though, for diagnostic purposes.
Wrapping it Up
Hashimoto’s thyroiditis is the #1 cause of hypothyroidism in the developed world.
As such, it’s incredibly important for patients who have this disease to get diagnosed with it as soon as possible.
There are some conditions that make diagnosing Hashimoto’s difficult because they are associated with negative thyroid antibodies.
These conditions include seronegative Hashimoto’s and end-stage Hashimoto’s.
You can diagnose these conditions by getting certain tests including a thyroid ultrasound.
For this reason, a thyroid ultrasound is a very helpful tool in patients who have thyroid disease!
Now I want to hear from you:
Do you have Hashimoto’s?
Do you have elevated antibodies?
Is your case of Hashimoto’s not as clear-cut as you want it to be?
Do you suspect or think that you have seronegative Hashimoto’s?
Leave your questions or comments below!
Scientific References
#1. https://pubmed.ncbi.nlm.nih.gov/24743395/
#2. https://pubmed.ncbi.nlm.nih.gov/18631004/
#3. https://radiopaedia.org/articles/hashimoto-thyroiditis
#4. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3821498/