Radioactive iodine is a procedure that results in the intentional destruction of your thyroid gland.
This procedure is often used to treat serious medical conditions such as hyperthyroidism and thyroid cancer.
But is this procedure without side effects?
Learn more about radioactive iodine including what it is used for, the side effects to watch out for, why it increases your risk of weight gain, and more in this guide:
Radioactive Iodine Basics & Is RAI Safe?
What exactly is radioactive iodine?
Radioactive iodine (often abbreviated RAI) is a therapy used to treat hyperthyroidism and thyroid cancer.
In this procedure, you are intentionally given Iodide, I-131, which emits radiation.
Your body then takes up this radioactive iodine into your thyroid gland where the radiation proceeds to destroy thyroid gland tissue.
RAI works because it takes advantage of certain aspects of normal physiology.
You probably already know that iodine (not the radiated version) is required for optimal thyroid hormone production.
Each thyroid hormone has a specific amount of iodide in it (2, 3, or 4 moieties depending on the type of thyroid hormone).
In addition, your thyroid gland stores up to 15-20 grams of iodine as a reservoir for thyroid hormone production (1) (stores that it can draw upon when necessary).
RAI takes advantage of this storage capacity of your thyroid gland.
So when you take RAI your thyroid will take up and store the radiated iodine which will cause local damage as it emits radiation and disrupts cellular function.
But why on earth would you WANT to destroy thyroid gland tissue? Surely there must be a better way.
RAI is often used to treat medical conditions which result in HYPERTHYROIDISM or the production of too much thyroid hormone from the thyroid gland.
Conditions such as Graves’ disease or Toxic multinodular goiter may result in excessive production of thyroid hormone.
This production can be stopped or blunted by either taking medication (anti-thyroid medication), removing the thyroid gland (thyroidectomy), or by completely destroying it with radioactive iodine.
In this way, RAI is a potent therapy that results in intentional damage to thyroid gland tissue.
As you might suspect, destroying your gland with radioactive iodine is associated with some side effects and is not without risk (but more on that later).
It may sound like a barbaric treatment, but it has been around since the 1940s and is often used to treat hyperthyroidism and thyroid cancer.

It is considered a “definitive” treatment for hyperthyroidism, much like thyroidectomy.
Is RAI safe to get?
For the most part, if done correctly and if proper precautions are taken after the procedure, yes it is safe.
There are some groups of people who should NOT use RAI, however, and this group includes pregnant women, women who are breastfeeding, and patients who are unstable or in a thyroid storm.
Now that you have a basic understanding of what RAI is and how it works, we can talk about how it is used for individual conditions.
DOWNLOAD FREE RESOURCES
Foods to Avoid if you Have Thyroid Problems:
I’ve found that these 10 foods cause the most problems for thyroid patients. Learn which foods you should avoid if you have thyroid disease of any type.
The Complete List of Thyroid Lab tests:
The list includes optimal ranges, normal ranges, and the complete list of tests you need to diagnose and manage thyroid disease correctly!
Treating Hyperthyroidism with RAI
Perhaps one of the most common uses of RAI is as a therapy to treat hyperthyroidism.
As we discussed, RAI results in complete and irreversible damage to the thyroid gland.
Because of this, you should consider all available options and therapies available to you before you undergo this procedure.
In the case of hyperthyroidism (caused by Graves’ disease, toxic multinodular goiter, or any other cause), RAI is considered to be a “definitive” therapy.
It’s definitive because after the procedure your thyroid gland will no longer function optimally and your hyperthyroidism will have been treated.
You can compare this to temporary hyperthyroid treatments such as thyroid-blocking medication.
Thyroid-blocking medication is NOT definitive because once you stop taking the medication your condition will most likely come back.
Is RAI effective at treating hyperthyroidism?
The answer is yes.
Up to 60-80% of patients with hyperthyroidism have Graves’ disease which is an autoimmune disease.
Patients with this condition often experience excessive doses of thyroid hormone as antibodies stimulate the thyroid gland.
Because of this, it is considered a safe alternative to complete thyroid removal (thyroidectomy) for hyperthyroidism.
It’s important to realize that RAI is not the only option available for the treatment of hyperthyroidism.
Before you undergo RAI make sure that you have evaluated all options available to you.
There are 3 primary ways to treat hyperthyroidism:
#1. Thyroid-blocking medications(usually temporary)
#2. RAI(more definitive than medication)
#3. Thyroidectomy(more definitive than medication)
You can learn more about these therapies in the links provided above.
Treating Thyroid Cancer with RAI
In addition to being used to treat hyperthyroidism RAI can also be used to treat thyroid cancer.
But it is often used in a different way which is worth discussing.
Thyroid cancer represents a different medical condition, when compared to hyperthyroidism, and requires slightly different treatment.
The baseline treatment recommended for thyroid cancer is thyroidectomy or complete thyroid removal.
This procedure allows for nearly the complete removal of the thyroid gland and usually 99+% of thyroid cancer cells.
But what you may not realize is that it is nearly impossible to remove 100% of the thyroid gland tissue even with thyroidectomy.
This leaves a small percentage of thyroid gland tissue in the body.
This remaining thyroid gland tissue slightly increases the risk of recurrence of thyroid cancer (3).
In addition, it is possible that thyroid cancer cells may exist outside of the thyroid gland during the operation (from metastatic disease).
Because of these two main reasons, RAI is often used as an additional therapy combined with thyroidectomy to completely eliminate thyroid gland tissue in the body (4).
This combination of therapy reduces the risk of thyroid cancer recurrence and increases the likelihood that you will kill any thyroid gland tissue or cancer cells that may be outside of the thyroid gland.
Is there a problem with this approach?
Remember that every procedure comes with risks and potential side effects.
These side effects must be weighed against the potential positive outcome of the therapy.
Because of this, not EVERY patient with thyroid cancer will undergo both procedures.
In fact, current recommendations state that the addition of RAI to thyroidectomy can be determined by the physician and based on the patient.
Before you get RAI in addition to thyroidectomy, these two factors should be considered:
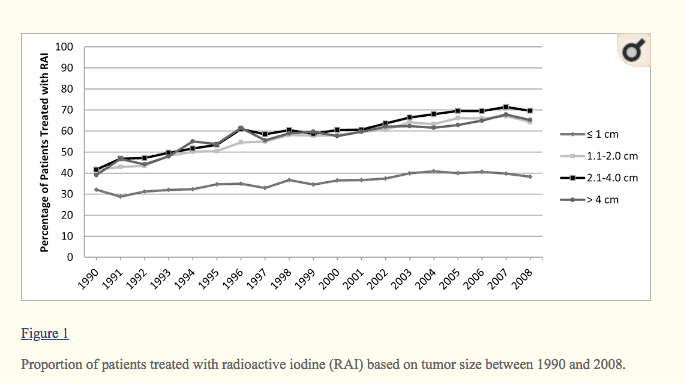
#1. Thyroid cancer has a low risk of recurrence after thyroidectomy.
Even without RAI, the risk of thyroid cancer recurrence is very low (5), so adding on the RAI may not further reduce that risk in every patient.
#2. There are always health risks associated with RAI.
RAI is a procedure in which radioactive iodine is given with the intent to destroy thyroid gland tissue.
There are side effects associated with this procedure (discussed below).
Around 50% of patients with thyroid cancer get both thyroidectomy and RAI (6).
This leaves another 50% who only get thyroidectomy.
Each individual patient with thyroid cancer should weigh the risks vs the benefits before adding RAI to their treatment plan.
Your Doctor should be able to help you determine if, in your case, RAI makes sense.
Side Effects of RAI & What to Expect After Therapy
While RAI is considered a “safe” procedure, it is not without risks (7).
Remember:
When you take RAI you are intentionally placing radioactive substances inside your body.
Yes, it is true that this radioactivity is mostly confined to your thyroid gland, but there is still a small risk that you can pass some of this radiation onto others.
Because of this, certain precautions must be taken to avoid this transfer to others.
But beyond the side effects, what should you expect after treatment?

Remember that the goal of RAI is to completely destroy your thyroid gland.
This destruction of thyroid gland tissue will permanently alter thyroid hormone status in your body.
After the procedure, you will be reliant upon thyroid medication for the rest of your life.
You are effectively turning yourself into a hypothyroid patient, which can be confusing for many patients, especially those who are undergoing RAI for the treatment of hyperthyroidism.
Many of the side effects associated with RAI have to do with the hypothyroid state which occurs AFTER the procedure and no side effects are directly associated with the procedure itself.
Weight Gain After RAI
It is well known that RAI poses a potentially serious threat to your current weight (8).
It has been reported (and shown) that the risk of becoming overweight and obese increases dramatically after radioactive iodine ablation therapy.
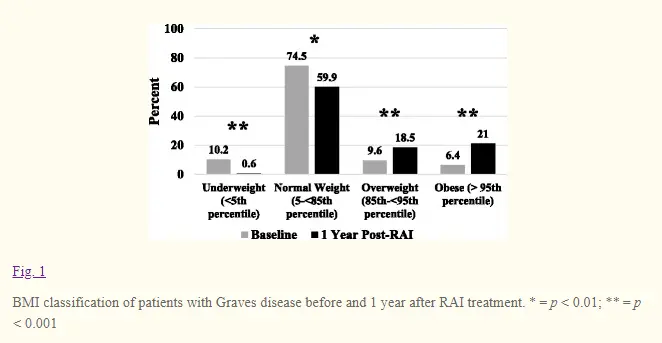
This risk increases anywhere from two-fold to three-fold compared to normal healthy euthyroid controls (those without thyroid damage).
It was previously thought that this weight gain was likely due to changes in metabolism and food intake after hyperthyroidism treatment, but the same effect is seen in those with normal thyroid status who undergo RAI (such as those with thyroid cancer).
Other theories suggest that the weight gain is the result of a hypothyroid state which may occur immediately after the procedure and before thyroid hormone levels are optimized with medication.
The exact cause of the weight gain is not well understood, but in my opinion, it is most likely related dosing of thyroid medication after the procedure.
Your thyroid is responsible for about 50-60% of your baseline metabolism (9).
Small changes to thyroid hormone may disrupt the normal regulation of your metabolism and may lead to weight gain.
It seems unlikely that physicians can perfectly balance how much thyroid hormone you need after your procedure with 1 pill taken once per day.
This weight gain is also seen post-thyroidectomy and with anti-thyroid medications, indicating that the weight gain is likely secondary to thyroid hormone levels and thyroid dosing.
You can learn more about this idea in this post.
It is important to know that not all patients who undergo RAI will experience dramatic weight gain.
Patients who go into the procedure overweight or obese are much more likely to experience weight gain after the procedure.
Side Effects Special to Men
RAI may pose a threat to fertility, especially in men.
This side effect is not necessarily a contra-indication to the procedure because banking your sperm prior to the procedure can bypass these negative effects.
Long-term infertility is typically not a problem unless multiple rounds of RAI are necessary (such as for metastatic cancer).
Before undergoing RAI make sure you consider this side effect and take the necessary precautions, such as banking sperm, if necessary.
Side Effects Special to Women
Specific to women, RAI does pose a serious risk to fetal development in pregnant women.
RAI is readily transferred across the placenta, which means it may seek out and destroy the thyroid gland of the developing baby.
Thyroid function is required for brain development and thyroid damage may result in mental retardation in the developing fetus.
RAI should also be avoided in women who are breastfeeding.
Reducing RAI Risk for Others + Precautions
Because RAI utilizes radioactivity, certain precautions must be taken after the procedure.
These precautions help to reduce exposure to radioactivity to loved ones or people who you live with.
Because of this risk physicians often make recommendations regarding avoiding sexual intercourse, avoiding contact with children, breastfeeding, avoiding sleeping next to people, and avoiding conception for days to months after the procedure.
Certain activities, such as sleeping next to someone, returning to work, preparing food for others, presence in public locations, traveling (air travel and car travel), sharing utensils with others, and sitting on a shared toilet only need to be avoided for up to 5-7 days.
While others, such as attempting conception, should be avoided for at least 6 months.
These precautions and recommendations from your physician may vary.
Current guidelines regarding safety post-RAI can be found here (11).
Conclusion
RAI is a relatively safe and very effective treatment for hyperthyroidism and thyroid cancer.
Like any procedure, make sure you weigh the potential benefits vs the risks because this procedure is not without side effects.
RAI results in permanent damage to your thyroid gland which will leave you reliant upon thyroid medication for the rest of your life.
This supplementation with thyroid hormone, if not done correctly, may increase your risk of weight gain, cardiovascular disease, and other side effects (12).
RAI should always be avoided if you are pregnant or breastfeeding, but other than that it doesn’t have many absolute contra-indications.
Now I want to hear from you:
Have you had RAI done?
Are you experiencing any negative side effects from the procedure?
Are you currently considering undergoing this procedure?
What are you worried about?
Leave your comments below!








