Are you suffering from high DHEA-s?
If so maybe you are experiencing symptoms such as fatigue, weight gain, or signs of hirsutism.
All of these symptoms and more may be caused by high levels of DHEA, but the question is what causes high DHEA to begin with?
Once you understand WHY your DHEA levels are high then you can begin to talk about how to lower them and treat the problem.
This guide will walk you through the primary causes of high DHEA levels and, more importantly, what to do about it:
What is DHEA?
DHEA stands for dehydroepiandrosterone which is a fancy name given to the most abundant circulating steroid hormone in the human body.
DHEA, and its sulfated form DHEA-S, is responsible for several different actions inside the cell and its unique ability to act as a hormone precursor for both estrogen and testosterone.
DHEA is very well known for its ability to convert into estrogen or testosterone (depending on the circumstances), but it also has direct cellular action by itself.
DHEA helps regulate immune function and acts on cells through an androgen receptor (1) (which is why low levels may lead to reduced libido and why high levels may cause symptoms of excess androgens).
Understanding how DHEA works helps us understand why it’s important to have enough of it in the body (not too much or too little).
DHEA is very much a Goldilocks type of steroid and androgen in the body.
What do I mean?
Studies have indicated that there is an increase in mortality (2) (increase in death) in patients who have too little or too much DHEA.

We can, therefore, interpret this to mean we want just the right amount of DHEA for optimal cellular function.
How do you know if you have high DHEA?
Most patients with high DHEA present with several key symptoms that trigger further testing which results in their Doctor finding high DHEA in their blood.
What kind of symptoms can you expect if you have high DHEA?
Symptoms of excessive serum DHEA-s and DHEA:
- Generalized fatigue or low-energy
- Weight gain
- Male patterned baldness or hair loss (in women and in men)
- Hirsutism
- Acne or oily skin
- Irritability, anger, or depression (and other changes in mood)
- Infertility
- Changes to your voice (a deeper voice in women)
- Changes to muscle structure (increase in muscle mass)
- Reduction in breast size
- Known history of PCOS
- Recent history of stress
The symptoms listed above are NOT normal and the presence of any of them should trigger further testing for adrenal hormones, cortisol, and DHEA levels.
Now that we have some basic information on DHEA let’s talk about what causes high DHEA.
6 Causes of High DHEA in Women
Before we jump into the causes let’s establish what a high level of DHEA is.
You can see an example below:

This patient has high DHEA-S with a value of 363.5 ug/dL with a reference range of 41.2 – 243.7.
This example is easy to diagnose because this patient falls outside of the given reference range.
But it is possible to have high-normal DHEA that causes symptoms in your body.
Part of this has to do with how your cells tolerate DHEA (hypersensitivity syndrome is discussed below).
The point is you need to be looking for an “optimal range” and in this case, it’s usually best for DHEA to be above 100 ug/dL but lower than 200 ug/dL.
In my clinical experience, it seems that women with DHEA-S levels over 200 ug/dL tend to experience the symptoms of androgen excess even though they are technically “normal”.
#1. Chronic Daily Stress
One of the most common causes of high DHEA is constant and persistent daily stress.
This is both a good and a bad thing…
It’s good in the sense that diagnosing the cause is relatively easy, and it’s hard in the sense that removing stress is something that most of us are not very good at.
How does stress lead to high DHEA?
In order to understand this relationship, we need to understand what stress does to the body.
Stress (really any cause of stress) stimulates a reaction in your body that activates a cascade of events in your HPA (hypothalamic-pituitary axis).
The activation of this axis results in hormone precursors that signal to your adrenal glands to produce hormones to combat the stress you are under.
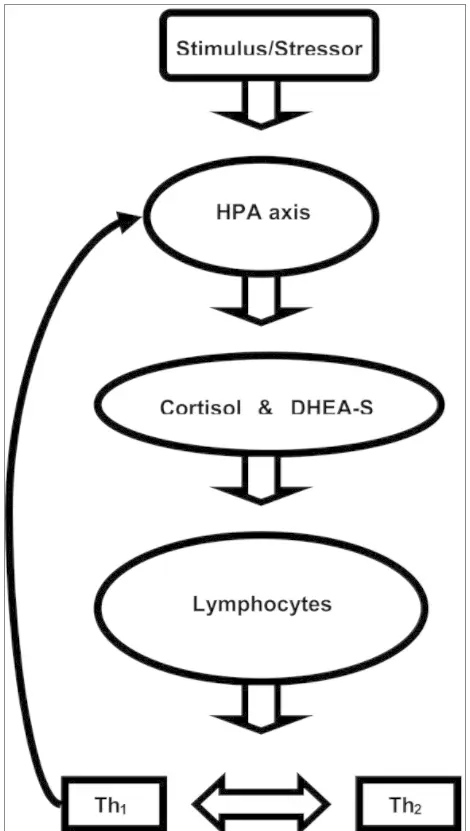
Usually, we associate this cascade with the release of cortisol (which is our “stress” hormone) and little attention is given to DHEA.
The truth is that stress causes the release of BOTH DHEA and cortisol from your adrenal glands.
The adrenal glands are non-discriminatory in the sense that their activation will lead to a release of more than just one hormone.
The release of cortisol and DHEA then acts on your cells and immune system to allow for adaptation to “tolerate” the stress you are under.
This cascade of hormones and changes usually isn’t a problem until the cascade is triggered too often.
Constant daily stress may lead to high circulating levels of DHEA and/or cortisol which then cause disruption to your immune system and other hormone systems.
For instance:
Stress has been shown to result in the rapid development of insulin resistance (3) (which may worsen weight gain) while chronic stress has been shown to suppress both cellular and humoral immunity (4).
The bottom line?
If your DHEA levels have been shown to be elevated AND you believe that stress may be playing a role you will want to take several steps:
- If possible find and eliminate the source of stress -> in some cases this won’t be possible so you may need to take further action to improve your “tolerance” of the stressful stimuli.
- Consider supplementing with the adrenal adaptogen Ashwagandha -> Ashwagandha has been shown in studies to reduce enzyme production in patients with adrenal hyperplasia (5) which may result in a direct reduction in androgen production in some individuals. Ashwagandha has also been shown to help balance cortisol levels which is also helpful if stress is worsening your DHEA. You can read my complete guide to using Ashwagandha here. Use a high-quality supplement with at least 500mg per day but note that some people may need up to 2,000mg per day.
- Consider further supplementation to improve adrenal function and treat chronic fatigue, you can find a complete guide and list here.
- Take steps to reduce the impact stress has on your life by adopting certain behavioral changes: get 8 hours of sleep at night, reduce your intake of refined carbohydrates and sugars, and exercise regularly (but not too much).
These steps will help you get started in the right direction but may not be sufficient for every person.
#2. PTSD
Another very common cause of high DHEA is PTSD (6).
Post-traumatic stress disorder is a disorder that results in multiple changes to hormone systems, the HPA axis, and immune function over time.
What’s more interesting is that the incidence of PTSD is at least 1% which estimates putting it as high as 15% of the general population of the US (7).
This is particularly important as it relates to DHEA.
Why?
Because studies have shown that PTSD results in documented high DHEA (8):

Unlike chronic stress (which we discussed above) PTSD generally results in high DHEA and low cortisol.
The hormonal systems seen in PTSD suggest that this condition exerts power and negative stimulus on the HPA system.
This condition is important to mention for several reasons…
First:
The diagnosis of PTSD may be missed as many patients may present with very generalized and non-specific symptoms.
This means that getting an accurate diagnosis becomes very important.
Second:
Treatment relies heavily upon the correct diagnosis and making targeted changes to reduce the impact of PTSD on your life.
Treatment may be complex and depends on the severity and cause of PTSD in each individual.
In addition to therapies such as counseling, patients may consider advanced techniques such as EMDR (9).
#3. PCOS
Next on the list is PCOS.
PCOS is actually one of the more common causes of elevated DHEA among women (along with stress and PTSD).
In fact, high androgens should prompt further work up into estrogen/progesterone levels to evaluate for PCOS.
It’s important to realize that PCOS is really just a combination of hormone imbalances that include the following:
- Elevated estrogen
- Low progesterone
- High insulin
- High Testosterone/DHEA
Studies have shown that PCOS likely has some hereditary component (10).
The brothers of women who have PCOS seem to show elevated DHEA levels (along with those women).
The difference is that males tend to tolerate higher levels of DHEA because men have higher levels of androgens at baseline.
The good news is that elevated DHEA secondary to PCOS can be treated by targeting the hormone imbalances associated with this condition.
I’ve put together a natural treatment guide for PCOS that you can see here.
I will leave the basic 7-step process below as well:
- Optimize your diet
- Exercise regularly
- Use the right supplements
- Reduce and manage your stress
- Address other hormone imbalances
- Avoid certain medications that may mask PCOS symptoms (birth control medications)
- Consider the use of certain prescription medications (if necessary)
You can also find more information about how to supplement for PCOS in this post.
#4. Elevated Prolactin
#4 isn’t as common as the other 3 but it’s worth mentioning here.
Prolactin is the hormone that normally promotes milk production in humans (and other mammals).
Normally prolactin should really only be produced in high quantities after pregnancy to promote milk production for children.
Some conditions (like microadenomas) may result in excessive production of prolactin during periods that are not considered “normal”.
High prolactin levels tend to suppress the menstrual cycle (which is why some women do experience a birth control-like effect when breastfeeding) by making changes to hormone levels in the body.
Prolactin has also been shown to directly increase DHEA levels and the presence of DHEA levels (11) (with a negative workup) should prompt evaluation into serum prolactin levels.
The good news is that assessing for high prolactin is quite easy and can be accomplished with basic serum testing.
If your prolactin level is elevated studies have shown that taking certain medications may help lower prolactin and therefore lower DHEA levels.
#5. Hypersensitivity to DHEA & Androgens at the Cellular Level
I’ve included this topic on the list because it’s very important but not necessarily a cause of high DHEA.
Instead, this condition may lead to high normal levels of DHEA and DHEA-s accompanied by symptoms associated with high DHEA (all of those we discussed above).
This can make diagnosis difficult for patients who fit into this spectrum which is why we are discussing it here.
Basically what is happening in this condition is that your cells become hypersensitive to even normal levels of androgens and DHEA.
Under normal conditions, DHEA interacts with androgen receptors on certain cells (think hair follicles and immune cells) to promote normal cell function.
In hypersensitivity syndromes, the exact same amount of androgen causes an exaggerated response which triggers cell stimulation and the symptoms of excess DHEA/androgens.
In hair follicles, this might mean increased hair growth or male-patterned baldness.
While this process is not well understood it’s what is felt to occur secondary to immune activation and it is seen in conditions such as benign prostatic hyperplasia (12) and androgenetic alopecia (hair loss) (13).
Remember that patients with this condition may present with completely normal labs but all of the symptoms are associated with high DHEA and high androgens.
Treatment for this condition should be targeted at the immune issues (if present) and any underlying hormone imbalances.
#6. Nonclassic Adrenal Hyperplasia (Late-onset adrenal hyperplasia)
Another uncommon cause of high DHEA is nonclassic adrenal hyperplasia (14) (otherwise known as adult-onset congenital hyperplasia).
This condition is an autosomal recessive genetic disease that tends to present later in life.

Women with this condition tend to have normal menses and pubertal growth patterns but symptoms of androgen excess tend to present later in life.
In addition, serum DHEA levels may be elevated when checked.
The condition stems from the overproduction/efficiency of certain adrenal enzymes which cause the production of excessive amounts of androgens.
Patients with this condition present with high DHEA levels along with symptoms such as acne, hirsutism, alopecia, and issues with fertility/menstruation.
Again, this isn’t a common diagnosis but it should be considered (15) if the cause of your elevated DHEA is unknown.
*Remember that ashwagandha has been shown to be effective in reducing DHEA in this condition (discussed above).
DHEA and Weight Gain
Many women who have high DHEA also tend to have weight gain.
This begs the question:
Does high DHEA cause weight gain?
The answer turns out to be slightly more complex than that.
Remember that the 3 most common causes of high DHEA include the following conditions: Stress, PTSD, and PCOS.
All of these conditions are associated with other hormonal abnormalities which are likely contributing to the weight gain seen in these patients.
Stress by itself has been shown to cause high cortisol, a reduction in sleep, and insulin resistance in addition to high DHEA levels.
PCOS includes high estrogen and leptin resistance which directly causes weight gain.
PTSD is often associated with mood changes/neurotransmitter changes which may alter diet and appetite.
Taken at face value it seems that the DHEA is probably NOT responsible for weight gain directly, but instead weight gain is the result of other hormone imbalances that tend to accompany high DHEA.
What does this mean for you?
If you have high DHEA and you are experiencing weight gain then your goal should be to find and treat the underlying cause of your high DHEA.
This will be the most effective way to lose weight.
Back to you
DHEA is an important hormone that needs to be in just the “right” range.
Everyday conditions such as stress may negatively impact DHEA and cause the symptoms of androgen excess.
If you are experiencing high DHEA the most important thing you can do is find the CAUSE and then target your treatment at that.
I’ve included the 6 most common causes of high DHEA in this article with the 3 most common being PCOS, stress, and PTSD.
Now I want to hear from you:
Do you have high DHEA? Are you experiencing the symptoms of androgen excess?
If so, has treating your high DHEA helped reduce these symptoms?
Leave your comments below!
Scientific References
#1. https://www.ncbi.nlm.nih.gov/pubmed/25022952
#2. https://www.ncbi.nlm.nih.gov/pubmed/20739385
#3. https://www.ncbi.nlm.nih.gov/pubmed/23444388
#4. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC1361287/
#5. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4543599/
#6. https://www.nimh.nih.gov/health/topics/post-traumatic-stress-disorder-ptsd/index.shtml
#7. http://www.healthcommunities.com/posttraumatic-stress-disorder-ptsd/incidence-prevalence-ptsd.shtml
#8. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2829297/
#9. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3951033/
#10. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4428582/
#11. https://www.ncbi.nlm.nih.gov/pubmed/6090494
#12. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4652646/
#13. https://www.ncbi.nlm.nih.gov/pubmed/22134564
#14. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2910408/
#15. http://emedicine.medscape.com/article/273153-workup#c6








